
In her first few years as an undergraduate student at the UW, Natalie Mazzawi did not see herself in a lab. Participating in research wasn’t on her radar.
research related posts

In her first few years as an undergraduate student at the UW, Natalie Mazzawi did not see herself in a lab. Participating in research wasn’t on her radar.

The IADR/AADOCR has selected Dr. Tracy Popowics and her team of UW researchers as the recipients of the William J. Gies Award for Biomaterials & Bioengineering.
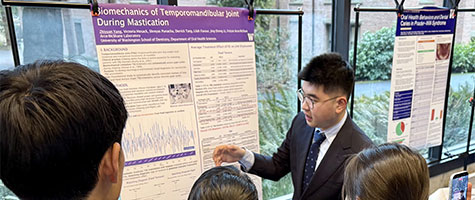
Mark Yang and Sydney Kim each took first place in the Dental Predoctoral Oral Presentation and Graduate Trainee Oral Presentation competitions, respectively, at the 2026 UW School of Dentistry Research Day last week.

Two UW undergraduate students, Summer Cho and Edric Tsang, were awarded Mary Gates Research Scholarships for their work with researchers at the UW School of Dentistry.

Priyanka Prajapati, a student in the UWSOD’s UWIDDS program, has done a tremendous job using interprofessional collaboration to help improve access to oral health care for underserved populations, winning a national award along the way.

The UW School of Dentistry’s Associate Dean for Research Dr. Donald Chi was one of five UW researchers to be named an American Association of the Advancement of Sciences Fellow, according to a March 27 announcement.

Lay Soon and Elissa Elmorr each took first place in the Graduate Trainee and Dental Predoctoral Oral Presentation competitions respectively at the 2025 School of Dentistry Research Day on Wednesday.

A cohort of UW researchers from UWSOD and ISCRM assisted in the discovery of the genetic variant that helps explain Finland’s high frequency and geographic distribution of cleft palate.

Last month, eight UW School of Dentistry students traveled to Minneapolis, MN to participate in the Academy of General Dentistry (AGD) national meeting and e-Poster competitions.

Dr. Claire Mills and Sydney Kim each took first place in the Graduate Trainee and Dental Predoctoral Oral Presentation competitions respectively at the School of Dentistry Research Day this past Wednesday.

The U.S. Food and Drug Administration (FDA) has approved Dr. Jonathan An from the UW Department of Oral Health Sciences to lead the first-ever study to evaluate rapamycin in older adults with periodontal disease.

A team of UW researchers have made a discovery that inflammation in one area of the mouth can cause a shift in the body’s immune responses in other healthy parts of the mouth, subsequently resulting in a shift in the microbiome.

The Summer Research Fellowship program, commonly known as SURF, is the School of Dentistry’s gateway research opportunity for predoctoral students. Over the past 25 years, the program has connected students interested in developing research skills with the School’s strongest research faculty members.
By Alden Woods, UW News
Over 30 years of dentistry, Sami Dogan has treated just about every kind of tooth ailment. Cavities are simple to fill. Dental implants have become routine. But there’s one problem, he said, that annoys even the most experienced dentists: hypersensitivity, the painful sensation sparked by contact with hot, cold or acidic food.

Why are some parents reluctant to let their child receive fluoride treatments from a dental provider? A new study, led by Dr. Donald Chi of the Department of Oral Health Sciences, has some answers.
Dr. Cameron Randall of the University of Washington School of Dentistry and his colleague, Dr. Daniel McNeil of the University of Florida, are continuing to illuminate the ways in which multidisciplinary research can benefit oral health.

Dr. Philip Walczak and Teddy Dong took first place in the Graduate Trainee and Summer Research Fellowship (SURF) Oral Presentation competition respectively this year at the School of Dentistry’s first in-person Research Day since the pandemic began.
Prominent organizations including the World Health Organization and U.S. Department of Agriculture (USDA) have dismissed low-carbohydrate diets that prevent tooth decay in favor of recommending high-carbohydrate diets which rely on fluoride and food fortification to mitigate dental damage and nutritional shortcomings, a University of Washington researcher says.
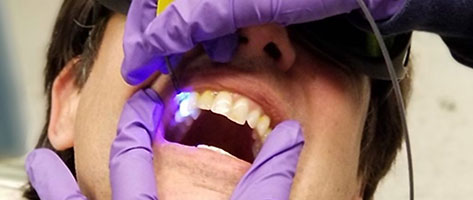
In a new study, School of Dentistry and other University of Washington researchers have developed a tool that can measure acidity levels of plaque on teeth, which can predict dental caries, or tooth decay.

Dr. Rachel Kehr and Deborah Lee took first place in the Graduate Student Research Competition and Dental Student Research Competition respectively at this year’s School of Dentistry virtual Research Day.

A large group of behavioral and social scientists, led by Dr. Cameron L. Randall of the University of Washington and Dr. Daniel W. McNeil of West Virginia University, are on a mission to throw the combined weight of their disciplines behind the effort to improve oral health globally.
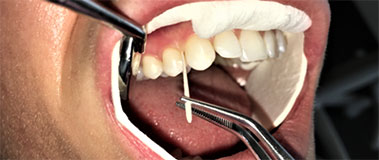
A team led by University of Washington researchers has, for the first time, identified and classified how different people respond to the accumulation of dental plaque, the sticky biofilm that gathers on teeth.
Before too long, you may be able to buy a breath mint that rebuilds your tooth enamel while it whitens your teeth, thanks to a team of University of Washington researchers.
The Timothy A. DeRouen Center for Global Oral Health at the UW School of Dentistry has received a grant from the UW Global Innovation Fund to help train junior researchers in Kenya in skills to facilitate publishing their work.
Oral health isn’t just about teeth. Thoughts and behaviors also play a big part. Dentists have long known the importance of influencing people’s behaviors and attitudes to promote healthy teeth and gums. That explains a good deal of the impetus for the Behavioral and Social Oral Health Sciences Summit, which will be held this Thursday and Friday in a virtual space.
Inside your mouth lives a group of bacteria whose closest relatives can also be found in the belly of a moose, in dogs, cats, and dolphins, and in groundwater deep under the Earth’s surface. In a noteworthy discovery, scientists led by a UW School of Dentistry researcher have found that these organisms have adapted to these incredibly diverse environments without radically changing their genetic makeup, or genomes.
A pair of studies led by University of Washington researchers has cast important new light on the body’s response to viral or bacterial invaders.
Apichai Yavirach, a student in the School of Dentistry’s Department of Oral Health Sciences, and Courtney Lang, a second-year dental student, won top recognition for their poster presentations at the School of Dentistry’s annual Research Day on Tuesday.
A team led by two UW researchers has found that a transplant drug with anti-aging properties can regenerate bone and decrease gum inflammation, pointing the way toward new treatments for common dental problems in aging patients.
Fluoride varnish has become a popular anti-cavity treatment for children, and it isn’t hard to see why. It’s relatively easy to apply, and not just for dentists or dental hygienists.
Dr. Jeffrey McLean, an associate professor of periodontics at the School of Dentistry, has been named to a three-year term as a member of the Oral, Dental and Craniofacial Sciences Study Section at the Center for Scientific Review. The center is part of the National Institutes of Health (NIH).
A larger genetic inventory may help explain how certain dangerous bacteria can persist in a hospital environment and continue to infect patients, according to a new study in the journal Proceedings of the National Academy of Sciences.
Laquita M. Grissett, a PhD candidate at the School of Dentistry, has been named a University of Washington Magnuson Scholar for 2019-20, the university has announced.
Topical fluoride, dental visits, and a diet with little or no sugar are all effective tools to maintain healthy teeth. But how can you maintain dental health when families can’t – or won’t – make use of those tools?
University of Washington researchers are helping to place oral health more squarely in the mainstream of HIV research, taking a major step during a symposium in Kenya’s Machakos County in February.
A team led by University of Washington researchers has uncovered what appears to be the first metabolic predictor of tooth loss.
Pre-doctoral and graduate dental students exhibited poster presentations of their research in diverse fields ranging from histology to oral biology to materials science at the School of Dentistry’s 24th annual Research Day on Monday.
Two University of Washington researchers and their colleagues have helped take a significant step forward in the study of especially tiny bacteria that may be linked to gum disease.