Single Purplish-Red, Right Anterior Buccal Gingiva & Maxillary Vestibule
Can you make the correct diagnosis?
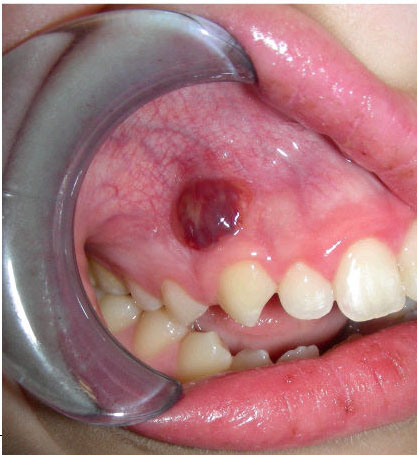
This 12-year-old white female was referred to the oral surgeon in October 2011 for the evaluation of a purplish-red and smooth surfaced nodule in the anterior maxillary vestibule.
Sorry! you are incorrect
The most common gingival swelling, especially in patients under the age of 20, is pyogenic granuloma. For that reason, it should be high on the differential diagnosis list. The color of this lesion, the age of the patient and the location are all supportive of a clinical diagnosis of pyogenic granuloma. The histology, however, is not supportive of PG.
Pyogenic granuloma constitutes 85% of all reactive gingival swellings. It presents as a profuse mass of vascular granulation tissue. It can be induced by local irritants such as excessive plaque, sharp fillings and dental calculus; it sometimes forms in an extraction socket in response to an irritant left in the socket. It can occur anywhere in the oral cavity and skin, especially the tongue, lips, fingers and nail beds. In the mouth, it occurs most commonly on the gingiva, especially the maxillary buccal and interproximal gingiva. Occasionally, it may surround the tooth. It is usually highly vascular, fast-growing, exophytic, lobular, sessile, and ulcerated or covered by pseudomembrane. The color changes from red to pink when it starts to heal. It occurs at any age and sex with a slight predilection for young females; it affects 1% of pregnant females. Pyogenic granuloma is usually painless except during eating, when bleeding and pain is described. Histologically, it presents as a mass of loose and vascular granulation tissue, usually with ulcerated or eroded surface epithelium and many inflammatory cells. A range of treatment modalities are available, including excision with removal of the local irritant, laser surgery, or intralesional injection with absolute alcohol, steroids or botulinum toxin. Scaling and polishing prior to surgical removal helps shrink the lesion. The prognosis is good, although recurrence is possible, especially during pregnancy.
Sorry! you are incorrect
The third most common gingival swelling, especially in this age group, is peripheral giant cell granuloma (PGCG). The color of this lesion and the age are supportive of PGCG. The location however is slightly higher than where PGCG would occur. The histology is not supportive of PGCG.
Peripheral giant cell granuloma constitutes less than 5% of all reactive gingival swellings. It consists of a hyperplastic mass of vascular granulation tissue with many osteoclast-like multinucleated giant cells. It presents as a lobular, purplish-blue exophytic nodule exclusively on the gingiva, both edentulous and dentate, and usually anterior to the molars. It originates from either the periodontal ligament or the periosteum. It occurs across a wide age range, especially in children, young adults, and females (2:1 female to male ratio). It presents as either sessile or pedunculated and smooth surfaced or lobular; though usually painless, it can occasionally be ulcerated, painful and accompanied by bleeding. Like pyogenic granuloma, it is usually present either on the buccal or lingual gingiva or between teeth, but it can occasionally surround the teeth and act aggressively by displacing teeth much like a sarcoma. It can also resorb the underlying bone in a smooth and concave “saucer-like” manner. Complete excision including curettage of underlying bone is the preferred treatment. It has a good prognosis with a recurrence rate of approximately 10%.
Sorry! you are incorrect
Although pyogenic granuloma would be very high on the list for this presentation, parulis (gumboil) should be placed as high if not higher, given the location (midroot). The color is a little too red but nonetheless gumboils with exuberant granulation tissue can be very vascular. The tooth is vital and the patient is too young for periodontal pocket and has no history of juvenile periodontitis. The histology is not supportive of a parulis.
Parulis or gumboil represents an accumulation of pus surrounded by a mass of hyperplastic granulation tissue present on the buccal gingiva as an exophytic mass simulating a gingival swelling. The origin of the pus is either from the apex of a non-vital tooth or a deep periodontal pocket. There is usually a sinus tract between the swelling and the apex of the tooth or the periodontal pocket. A gutta-percha point can be of assistance in tracing the origin of the abscess. Treatment includes treatment of the source. Surgical removal of the exophytic lesion may or may not be necessary once the source of the abscess if treated.
Sorry! you are incorrect
The color and the age of the patient are certainly good for a hemangioma and therefore should be included on the differential diagnosis. The location however is not and neither is the histology.
Hemangioma is a family of benign developmental vascular anomalies occurring at infancy. They progress through two stages of growth: a rapid growth phase followed by an involution phase. Vascular lesions are most common in infants. Lymphangiomas occur at birth and progress with age, while hemangiomas typically occur a few weeks after birth and continue to grow rapidly for the first year; they stop growing and begin to involute within the subsequent few years. Hemangiomas are benign proliferations of blood vessels with many classifications; capillary and cavernous hemangiomas are the most common types. Capillary hemangiomas affect 1% of all newborns in the United States. Half of all hemangiomas occur in the head and neck area, especially the tongue. They are the most common cause of macroglossia. They can also occur on the buccal mucosa and lips. In addition, hemangioma has a slight predilection for occurrence in females. The lesion can present as flat or exophytic, smooth-surfaced or lobular, and localized or diffuse; though usually single and localized, it can also present in multiples. Superficial hemangiomas are bright red, while the deep lesions are purplish-red in color; they blanch on pressure unless thrombosed. The vast majority will regress and resolve within the first ten years of age. Treatment of hemangioma depends on its size, its relationship to other anatomical structures and the rate of blood flow. Observation is important since many spontaneously involute, especially capillary hemangiomas. If a hemangioma persists, local topical application of injections with corticosteroids has a 75% success rate of involution within two weeks to two months post-injection. Several complications are described with local and systemic use of steroids; interferon alfa-2a has also been successfully used. Surgical procedures include excisional scalpel surgery for smaller lesions and laser removal for larger lesions. Laser use includes CO2; argon and other types of laser have also been used with variable rate of success Prognosis depends on the size and whether it is a soft tissue or bony lesion: it can range from good to extremely poor with gross facial deformity and compromised function.
Congratulations! You are correct
The age of this patient is good for this condition. However, neither the clinical presentation, nor the location or the color is typical of the oral manifestation of Langerhans cell histiocytosis (LCH). The histology and the Immunohistochemistry staining are definitively that of LCH.
Langerhans cells are dendritic cells of bone-marrow origin. The disease Langerhans’ cell histiocytosis is generally a disease of children rarely affecting adults. The old name for this condition is histiocytosis X classified into eosinophilic granuloma (monostotic and polyostotic, Hand-Schuller-Christian and Letterer-Siwe disease. The first two types (EG and HSC) are less aggressive and are chronic in clinical behavior while the last (LS) is more aggressive and acute in behavior. The currently used classification breaks patients into unifocal, multifocal/unisystem and multifocal/multisystem. This classification also divides patients into low and high risk categories. Low-risk patients would include the unifocal and multifocal/unisystem and the high-risk would include multifocal/multisystem patients. If the disease affects one organ be it in one site or multiple sites of one organ (i.e. bone, lymph nodes, skin), it is considered to be low-risk type. If the disease involves multiple organs such as the lungs, liver, spleen and bone marrow (multifocal and multisystem), it is considered to be high-risk type. Langerhans cells are CD1a positive and for that reason, immunohistochemistry staining is very helpful. They are also S-100 and CD45 positive. Langerhans cells can also be comfortably identified by the H & E stain.
The typical presentation of LCH in the mouth is in form of a lytic lesion in the posterior mandible usually with pain and swelling but can also be asymptomatic. The bony lesions are usually aggressively lytic especially those of the mandible. As mentioned above, this disease rarely occurs in adults and that more than 50% of the cases affect children under 10 years of age, with male predilection. Oral soft tissue involvement with LCH is very rare especially as an isolated nodule as is the case in this patient.
Adult LCH most commonly affects the bones especially the jaws and skull bones in general. LCH of the jaw bone usually presents as either localized severe periodontitis or generalized severe periodontitis. It can also affect the skin, lymph nodes, pituitary (not common) and lungs (not common). Radiographically, the bony lesions are sharply radiolucent and the jaw lesions give the impression of teeth “floating” in space due to the significant bone destruction.
Treatment includes curettage especially of the jaw lesions. Chemotherapy and low-level radiotherapy have also been effective. The unifocal disease has an overall 95% survival rate, the two organ involvement has a 75% overall survival rate and the more organs are involved, the less favorable the prognosis.
References
- Fantasia JE, Damm DD. Red nodular lesion of tongue. Pyogenic granuloma. Gen Dent. 2003 Mar-Apr;51(2):190, 194.
- Ichimiya M, Yoshikawa Y, Hamamoto Y, Muto M. Successful treatment of pyogenic granuloma with injection of absolute ethanol. J Dermatol. 2004 Apr;31(4):342-4.
- Pham J, Yin S, Morgan M, Stucker F, Nathan CA. Botulinum toxin: helpful adjunct to early resolution of laryngeal granulomas. J Laryngol Otol. 2004 Oct;118(10):781-5.
- Flaitz CM, Peripheral giant cell granuloma: a potentially aggressive lesion in children. Pediatr Dent. 2000 May-Jun;22(3):232-3.
- Chaparro-Avendano AV, Berini-Aytes L, Gay-Escoda C. Peripheral giant cell granuloma. A report of five cases and review of the literature. Med Oral Patol Oral Cir Bucal. 2005 Jan-Feb;10(1):53-7; 48-52.
- Neville BW, Damm DD, Allen CM, Bouquot JE. Peripheral giant cell granuloma. In: Oral and Maxillofacial Pathology, 2nd edition. Philadelphia: W.B. Saunders, 2002. p. 449-451.
- Chan YC, Giam YC. Guidelines of care for cutaneous haemangiomas. Ann Acad Med Singapore. 2005 Jan;34(1):117-23.
- Whang KK, Cho S, Seo SL. Excision of hemangioma and sculpting of the lip using carbon dioxide laser. Dermatol Surg. 2004 Dec;30(12 Pt 2):1601-2; author reply 1602.
- Benedetto AV. News in treatment of angiomas. J Eur Acad Dermatol Venereol. 2004 Mar;18(2):122-3.
- Lambrecht JT, Stubinger S, Hodel Y. Treatment of intraoral hemangiomas with the CO2 laser. Schweiz Monatsschr Zahnmed. 2004;114(4):348-59.
- Bonet J, Manuel MJ et al. Eosinophilic granuloma of the jaws: a report of three cases. Med. Oral. 2001; 6: 218-224.
- Favara BE, Feller AC, Pauli M et al. Contemporary classification of histiocytic disorders. Med Pediatr Oncol 1997; 29: 157–66.
- Baumgartner I, von Hochstetter A, Baumert B et al. Langerhans cell histiocytosis in adults. Med Pediatr Oncol 1997; 28: 9–14.
- Malpas JS, Norton AJ. Langerhans cell histiocytosis in the adult. Med Ped Oncol 1996; 27: 540–6.