Diffuse and Deep Ulceration; left ventral tongue
Can you make the correct diagnosis?
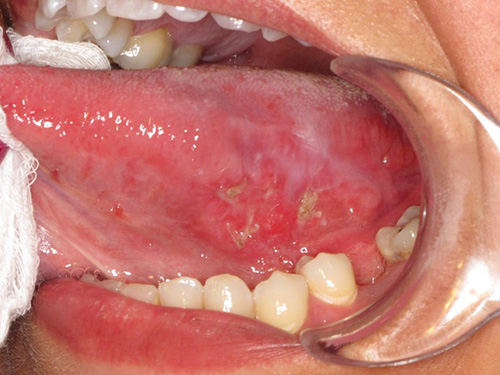
This is a 32-year old white female who presented at the Auburn Oral & Maxillofacial Surgery Clinic with a 3-month history of a painful, slowly enlarging “ulcer” on the left ventral/lateral border of the tongue.
Sorry! you are incorrect
The oral cavity is frequently afflicted with surface ulcerations: single and multiple, superficial and deep, acute and chronic, of local and of systemic origin. For that reason, it is very important that clinicians view oral ulceration with some attention to etiology. The diffuse and deep nature of this ulceration does not preclude it from being traumatic ulcerative granuloma with stromal eosinophilia (TUGSE). Since the ventral and base of tongue are not directly in the area where trauma from a deep bite can occur, other sources of injury should be ruled out including sharp teeth and sharp fillings. Neither were present in this patient and therefore trauma was ruled out. The histology was not supportive of TUGSE.
Traumatic ulcerative granuloma with stromal eosinophilia (TUGSE) ulcers are also known by other names, including eosinophilic ulcer, ulcerative eosinophilic granuloma of the tongue (which is not related to eosinophilic granuloma of the bone as in Langerhans Cell Histiocytosis), and traumatic granuloma. Traumatic ulcerative granuloma with stromal eosinophilia commonly occurs on the dorsal and lateral tongue, usually in patients with a history of trauma. The latter is not always clearly demonstrated. Although the tongue is the most common location, TUGSE has also been described in other areas such as the lips, buccal mucosa, gingiva and vestibule. TUGSE affects patients of all ages but is more common in adult males. It is described in children as young as infants with Riga-Fede, a disease that occurs during the first year of life as a result of chronic trauma in the sublingual area and ventral tongue occurring during breastfeeding due to the sharp-edged central lower incisors. The clinical presentation of TUGSE ranges from a small ulcer with rolled borders to an exophytic large lesion simulating a pyogenic granuloma. It can also present as a very large, indurated and deep ulcer simulating a squamous cell carcinoma or any other malignancy of the mouth. The duration of the non-healing ulcer can range from two weeks to many months. TUGSE tends to occur more in males than females. Histologically, these ulcers are deep lesions involving the underlying muscle, which may explain the process of slow healing and the tissue eosinophilia. Healing may take up to eight weeks, sometimes more.
Congratulations! You are correct
Although the site and the clinical presentation are typical of oral squamous cell carcinoma, the age and gender of this patient are not. Based on the clinical presentation alone, oral SCC has to be placed high on the differential diagnosis. Oral SCC becomes a more significant consideration with the clinical history of fourteen years of tobacco use.
Oral squamous cell carcinoma is a highly aggressive neoplasm that currently ranks as the fifth most common malignant neoplasm worldwide and accounts for an estimated 90% of all oral malignancies. It is predominantly diagnosed in males over the age of 40 years, with an observed male-to-female ratio of 2:1 generally and 1.4:1 in the United States. The incidence of oral SCC in patients under the age of 40 is relatively low, around 5%. Prolonged histories of tobacco and alcohol consumption are the main risk factors in both populations. Other risk factors including human papilloma virus, especially type 16, have been reported to be significant, especially in the young male population with tonsillar and laryngeal squamous cell carcinomas. Other factors include poor oral hygiene, syphilis, chronic candidiasis, iron and dietary deficiencies, herpes simplex and various other immunologic factors, and lichen planus – especially persistent erosive lichen planus. The most common sites of occurrence for oral squamous cell carcinoma are the tongue, the ventral and lateral surfaces, and the floor of mouth. Excluding the outer lip, the most common sites (in decreasing order) are the ventral and lateral surfaces of the tongue (25-50%), floor of mouth (15%), gingiva (12%) and palate (9%). The buccal mucosa and retromolar pad areas (3%) have a relatively low incidence of occurrence unless the patient is a chronic smokeless tobacco user. Oral SCC varies in presentation from deceptively benign looking to obviously malignant. It may present as a non-healing ulcer, or as red, white or mixed red-and-white lesions. Characteristic signs of oral SCC are non-healing ulcer, ulcer with rolled borders, fungation, fixation and induration. Rarely, oral SCC may present as unexplained asymptomatic lateral neck lymphadenopathy. Determination of the prognosis of oral SCC is based on its clinical stage and histological classification. Although oral SCC is a diagnosis made by histology, surgeons tend to depend exclusively on the TNM classification system for clinical staging and treatment decisions. Prognosis is dependent on the TNM staging system; the most important prognostic sign is the presence or absence of metastases at the time of diagnosis. The prognosis thus improves when the lesion is detected early. Oral SCC patients die mainly of infection due to lowered resistance or of hemorrhage if the tumor erodes through one of the main blood vessels.
References
- Açikgõz A,Uzun-Bulut E, Ozden B, Gündüz K. Prevalence and distribution of odontogenic and nonodontogenic cysts in a Turkish Population. Med Oral Patol Oral Cir Bucal. 2011 Jul 15.
- Ramachandra P, Maligi P, Raghuveer H. A cumulative analysis of odontogenic cysts from major dental institutions of Bangalore city: A study of 252 cases. J Oral Maxillofac Pathol. 2011 Jan;15(1):1-5.
- Oda D, Rivera V et al. Odontogenic keratocyst: the northwestern USA experience. J Contemp Dent Pract. 2000 Feb 15; 1(2): 60-74 .
- Kumar ND, Sherubin JE, Raman U, Shettar S. Solitary bone cyst. Indian J Dent Res. 2011 Jan-Feb;22(1):172-4.
- Kahler B. Traumatic bone cyst suggestive of a chronic periapical abscess: A case report. Aust Endod J. 2011 Aug;37(2):73-5.
- Williams HK, Mangham C, Speight PM. Juvenile ossifying fibroma. An analysis of eight cases and a comparison with other fibro-osseous lesions. J Oral Pathol Med. 2000;29:1318.
- Eversole LR, Leider AS, Nelson K. Ossifying fibroma. A clinicopathologic study of sixty-four cases. Oral Surg Oral Med Oral Pathol. 1985;60:505–511.
- Samir El Mofty Psammomatoid and trabecular juvenile Ossifying Fibroma of the craniofacial skeleton: Two distinct Clinicopathological entities. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2002; 93:296-304.
- Johnson LC, Yousefi M, Vinh TN, Heffner DK, Hymans VJ and Hartman KS. Juvenile active ossifying fibroma, its Nature, Dynamics and Origin Acta Otolaryngol 1991; suppl 1 488: 1-40.
- Whitaker SB, Vigneswaran N, Budnick SD, Waldron CA. Giant cell lesions of the jaws: evaluation of nucleolar organizer regions of varying behavior. J Oral Pathol Med 1993; 22(9):402-5.
- Tallan EM, Olsen KD, McCaffrey TV, Unni KK, Lund BA. Advanced giant cell granuloma: a twenty-year study. Otolaryngol Head Neck Surg 1994; 110(4):413-8.
- Carlos R, Sedano HO. Intralesional corticosteroids as an alternative treatment for central giant cell granuloma. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2002; 93(2):161-6.
- O´Regan EM, Gibb DH, Odell EW. Rapid growth of giant cell granuloma in pregnancy treated with calcitonin. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2001; 92(5):532-8.
- Collins A. Experience with anti-angiogenic therapy of giant cell granuloma of the facial bones. Ann R Australas Coll Dent Surg 2000; 15:170-5.
Sorry! you are incorrect
Some infections of the oral cavity, especially the deep granulomatous type of infectious diseases, may present as diffuse, deep ulcers with rolled borders on the lateral ventral tongue comparable to the clinical presentation of malignant neoplasms such as squamous cell carcinoma. For that reason, infectious-type diseases should be included on the differential diagnosis, especially if the patient is immune compromised. While this patient is not immune compromised and is otherwise healthy, infectious disease-type ulcers should still be considered on the differential diagnosis. The histology is not supportive of any infectious-type disease.
The oral cavity is a site where a number of acute and chronic infectious diseases occur as a local primary disease or as a manifestation of a systemic disease. They include diseases of viral, fungal and bacterial origin. They usually present in multiples or in a diffuse manner ranging from ulcers to small and nodular lesions to verrucoid lesions. Occasionally, granulomatous-type infectious diseases present as diffuse and deeply ulcerative lesions with rolled borders, simulating oral SCC. These cases include ulceration induced by mycobacterium tuberculosis, deep fungal infections such as blastomycosis and histoplasmosis, and chancre of primary syphilis. Oral manifestations of tuberculosis and histoplasmosis are unusual without lung involvement and a disseminated disease; they occur more often in immune-compromised patients. The gingiva and the mandibular vestibule are more common locations, but the tongue can occasionally be affected. Chancre can occur in any location, including the tongue, lips and hard palate.