Large, Necrotic Exophytic Mass, Left Posterior Mandible
Can you make the correct diagnosis?
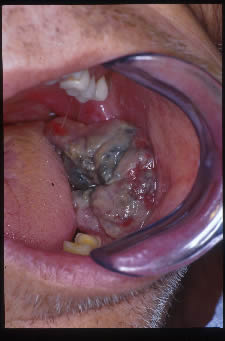
The patient is a 62-year-old white male who presented to the University of Washington emergency room complaining of mouth pain and limited ability to swallow his medications. He also complained of shortness of breath which decreased when he sat down. A large mass was noted to be growing out of the socket of an extracted lower left molar tooth
Sorry! you are incorrect
Given the patient’s chronic and heavy cigarette use over the last forty years, squamous cell carcinoma should be included on the differential diagnosis. Clinical presentation of SCC emerging from a non-healing ulcer, although not common, is fairly well described in SCC of the gingiva. Oral squamous cell carcinoma is a highly aggressive neoplasm that currently ranks as the fifth most common malignant neoplasm worldwide and accounts for 90% of oral malignancies (1). The incidence of oral SCC is incessantly increasing. For details on SCC, please read the April 2004 Case of the Month. The five-year survival rate lies between 35% and 50% (2) and has not significantly improved despite increasingly sophisticated medical accomplishments. Oral SCC occurs predominantly in males over the age of 40 years, with an observed male to female ratio of 1.4:1 in the USA (1). Excluding the outer lip, the most common sites (in decreasing order) are ventral and lateral surfaces of tongue (25-50%), floor of mouth (15%), gingiva (12%) and palate (9%). The buccal mucosa and retromolar pad areas (3%) have a relatively low incidence of occurrence (3). Gingival SCC has a tendency to destroy bone in about 50% of cases. Oral SCC varies in presentation from deceptively innocent-looking to obviously malignant. The latter is the case in this patient. It may present as a non-healing ulcer, or as red, white or mixed red-and-white lesions. Characteristic signs of oral SCC are non-healing ulcer, ulcer with rolled borders, fungation (this patient), fixation and induration. Rarely, OSCC may present as unexplained, asymptomatic lateral neck lymphadenopathy (1-3). The location, age, risk factors and clinical presentation of this case are typical of OSCC. The histology of this specimen was that of a poorly differentiated carcinoma, but was not consistent with a squamous cell carcinoma.
Sorry! you are incorrect
Aggressive fibromatosis represents a group of fibrous neoplasms with various clinical behaviors and histologic presentations. One of the names that this disease carries is nonmetastasizing fibrosarcoma (4), best describing this disease as a locally infiltrative and aggressive neoplasm with a potential for multiple local recurrences, but no potential for metastasis. Head-and-neck aggressive fibromatosis usually occurs in children under 20 years of age (5). It is more prevalent in adult females by a ratio of 2:1 (5). Neither the age or the gender are compatible with this case. It typically presents as a firm, painless, rapidly growing asymptomatic mass. It can destroy bone, infiltrate adjacent structures, displace teeth, and induce periosteal reaction, rendering it clinically and radiographically difficult to differentiate from a malignant neoplasm such as a sarcoma. It presents in multiple locations within the oral cavity, including the gingiva, lips and other oral soft tissue areas. For more information, please review the February 2004 Case of the Month. The histology of this case is not supportive of aggressive fibromatosis.
Sorry! you are incorrect
Several malignant neoplasms of mesenchymal origin can occur in the oral cavity, but constitute a small number of malignancies. The most common of the sarcomas would be osteosarcoma, which affects individuals around 34 years of age and favors the mandible over the maxilla (6). It can be very aggressive and cause both bone destruction and soft tissue mass production. In particular, chondrosarcoma should be included in the differential diagnosis because it is a disease of adults over the age of 30. It is less aggressive in behavior than an osteosarcoma and occurs more commonly in the maxilla than the mandible. Other sarcomas such as fibrosarcoma and rhabdomyosarcoma can occur as primary lesions in the oral cavity, but are rare and occur more often in the younger population (7). Pleomorphic rhabdomyosarcoma is a disease of adults rather than children. The histology in this case was not supportive of a sarcoma (6, 7).
Sorry! you are incorrect
The oral cavity is a site where a number of deep fungal infections can occur. However, deep fungal infections are not commonly found in the U.S. These diseases tend to occur in developing countries in areas such as Latin America and Africa. This type of tissue necrosis and swelling can be associated with an infection such as blastomycosis, which can occur in the United States and Canada and tends to occur mostly in otherwise healthy adult males with a male-to-female ratio of 9:1. Histoplasmosis, on the other hand, is a disease that is seen in elderly and debilitated patients, especially those who are chronically ill and immunocompromised (8). It occurs in the Ohio-Mississippi River area and it can affect the general population, usually as a subclinical disease. It is unusual to develop histoplasmosis of the mouth without lung involvement. Other deep fungal infection such as zygomycosis (mucormycosis) can also occur in the oral cavity, especially in the maxillary sinuses and nose, breaking through the palate. These lesions occur in uncontrolled diabetics and immunocompromised patients. Although the clinical presentation of fast growth and soft tissue necrosis is compatible with a deep fungal infection, the histology in this case was not supportive of such disease.
Congratulations! You are correct
Final Diagnosis
Poorly differentiated carcinoma consistent with metastatic, poorly differentiated non-small cell lung carcinoma.
Disease Description
Given the patient’s history of lung cancer, tumor metastasis has to be considered very seriously in this case. Cancer metastasis to the oral cavity is neither specific nor common. Although it constitutes less than 1% of all oral malignant neoplasms, it may have a devastating result to the patient mainly because metastasis to other sites has already developed or is inevitable (9-10). Theoretically, any malignant neoplasm can metastasize to the oral cavity, but in actuality few do and out of the ones that do, the majority are carcinomas rather than sarcomas. The most common malignant neoplasms that metastasize to the mouth are from the breast, lung, kidney and prostate (9-10). Malignant neoplasms from the thyroid, pancreas, colon, and liver have also been described. Breast cancer is the most common neoplasm to metastasize to the oral cavity regardless of gender. However, lung and prostate cancers are the most common neoplasms to metastasize to the oral cavity in men. In the most cases, the oral presentation is a secondary diagnosis where the primary diagnosis of the distant organ has been already made and the patient has had or is undergoing treatment for it. This was true of our patient. Although rare, it is known that on occasion, the oral lesion is the first manifestation of the disease. By far the most common location is the posterior mandible, where 80% of cases occur, followed by the gingiva. The maxilla is a rare location for tumor metastasis. It is mostly described in adults over the age of 30 and rarely in children. Pain and swelling are the most common clinical symptoms, which was the case with this patient. They may also present as asymptomatic, simulating a periapical lesion, gingival swelling like a pyogenic granuloma or it can cause anesthesia and parasthesia, especially when it involves the inferior alveolar canal. The latter results in so-called “numb-chin syndrome.” Tooth loosening, displacement and sharp resorption have also been described. This patient presented with a lesion erupting from a non-healing extraction site, which is seen at times. The radiographic appearance of irregular bony destruction is also common for metastatic tumor. The majority of neoplasms cause bony destruction with ill-defined borders, the moth-eaten appearance of some bony destruction indicating aggressive behavior. It is also important to mention that at times, well-demarcated lesions with a benign morphology, as well as cystic radiographic morphology, have also been described. Metastatic neoplasms from the prostate may also be bone-forming, resulting in a radiopaque of mixed radiolucent and radiopaque lesion misdiagnosed as a benign fibro-osseous lesion.
As in this case, the diagnosis of tumor metastasis to the oral cavity carries a poor prognosis because the oral cavity is usually not an isolated site and tends to project more disseminated clinical behavior (9-10). Patients are typically treated with chemotherapy and the five-year survival rate is very low.
Treatment
An incisional biopsy was performed of the central mass and peripheral gingiva under local anesthesia. The tissue was noted to be friable, bled easily, and would not hold sutures.
Surgical bulking of left oral cavity malignant mass and true vocal injection with Cymetra was performed following the definitive histologic diagnosis was obtained. Patient was admitted to the hospital for continued treatment of the recurrent and metastatic lung cancer.
References
- Examinations for oral cancer – United States. MMWR. Morb.MortalWkly Rep. 1992; 43:198.
- Barasch A, DE Morse, et al. Smoking, gender, and age as risk factors for site-specific intraoral squamous cell carcinoma. Cancer 1994; 73:509-513.
- American Joint Committee for Cancer Staging and End Result Reporting. 1983.
- Donahue WB, Malexos D, Pham H. Aggressive fibromatosis of the maxilla. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1990; 69:420-426.
- Fletcher CDM. Diagnostic Histopathology of Tumors, Volume 2. 2000; 1498-1500.
- Oda, D. Bavisotto, L.et al. Osteosarcoma of the Head and Neck: The University of Washington experience. Head & Neck. 1997; 19; 513-523
- Chigurupati, R, Aflatooni, A et al. Rhabdomyosarcoma of the head and neck in children, review of literature and addition of four cases. J Oral Oncology. 2002; 38: 508-515.
- Oda, D., McDougall, L., et al. Oral histoplasmosis as a presenting disease in the Acquired Immune Deficiency Syndrome. Oral Surg, Oral Med, Oral Path 1990; 70: 631-636.
- A. Hirshberg and A. Buchner , Metastatic tumours to the oral region. An overview. Oral Oncol. 1995; 31: 355–360.
- van der Waal, RIF, Buter, J. Oral metastases: report of 24 cases. Br J Oral Maxillofac Surg. 2003; 41: 3-6.