Bilateral unilocular radiolucency associated with mandibular second molars
Can you make the correct diagnosis?
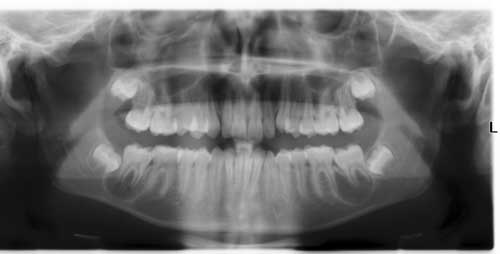
This is a 13-year-old white male who presented with mild swelling and tenderness in the left posterior mandible. The right posterior mandible was asymptomatic where no pain was reported or swelling noted.
Sorry, you are incorrect!
The age, gender, multifocal radiolucencies and the site being posterior mandible are all consistent with LCH affecting multiple site of the mandible. The corticated radiolucency with buccal and lingual bone being intact is not consistent with the radiographic and clinical presentation of LCH in the jaw bone. The typical radiographic presentation of LCH in the mandible is that of localized severe periodontitis with teeth “floating in space” not consistent with the radiographic features shown in figure 1. The H & E histology and the immunohistochemistry (IHC) staining with CD1a antibody are not consistent with LCH.
The typical presentation of LCH in the mouth is in form of a lytic lesion in the posterior mandible usually associated with pain and swelling but can also be asymptomatic. The bony lesions are usually aggressively lytic especially those of the mandible. More than 50% of the LCH cases affect children under 10 years of age, with male predilection; it rarely occurs in adults.
Radiographically, the jaw lesions usually present as localized but on rare occasions, the jaw lesions can be generalized giving the impression of severe periodontitis.
Langerhans cells are dendritic cells of bone-marrow origin. The disease Langerhans’ cell Histiocytosis is generally a disease of children rarely affecting adults. The currently used classification breaks patients into unifocal, multifocal/unisystem and multifocal/multisystem. This classification also divides patients into low and high risk categories. Low-risk patients would include the unifocal and multifocal/unisystem and the high-risk would include multifocal/multisystem patients. If the disease affects one organ be it in one site or multiple sites of one organ (i.e. bone, lymph nodes, skin), it is considered to be a low-risk type. If the disease involves multiple organs such as the lungs, liver, spleen and bone marrow (multifocal and multisystem), it is considered to be a high-risk type. Langerhans cells are CD1a positive and for that reason, immunohistochemistry staining is very helpful.
Congratulations, you are correct!
The age, gender, site (being second molar but usually more so first molar), the bilateral presentation and the corticated radiolucencies is typical clinical and radiographic presentation of mandibular buccal infected cyst. The clinical presentation of the right side being “asymptomatic” despite the radiographic findings of a radiolucency associated with tooth #31 is unusual but has been described. The histology is consistent with bilateral mandibular buccal infected cysts.
While the main cause of a dental abscess in a child is a periapical lesion due to a badly carious or fractured and non-vital tooth, abscesses can occasionally be attributed to reasons other than the obvious bad tooth. Such is the case with a mandibular buccal infected cyst, also known as paradental cyst, and buccal bifurcation cyst. Mandibular buccal infected cyst is an inflammatory cyst involving the buccal and disto-buccal aspects of the mandibular permanent molars, and is usually attached to the cervical margins extending down to the root bifurcation. It has been shown to involve the permanent premolar teeth but rarely. These cysts are frequently misdiagnosed as inflammatory dentigerous cysts, lateral radicular or lateral periodontal cysts. They affect children around 8-13 years of age, and are more common in males. Paradental variant tends to occur in older patients around 24 years of age. Patients usually present with buccal gingival swelling, pain, and at times a sinus tract releasing pus. These cysts are often bilateral. Radiographically, these cysts are readily diagnostic with specific features, including the presence of a periodontal defect buccal and distal to the involved tooth, buccal expansion of the buccal cortical bone. Teeth are displaced lingually and usually the adjacent non-erupted tooth shows no evidence of an increased follicular space.
Sorry, you are incorrect!
The bilateral radiolucency around molar teeth in a young patient should make one think of localized aggressive periodontitis (LAP) and localized prepubertal periodontitis (LPP).
Localized aggressive periodontitis (LAP) usually affects the permanent incisors and the permanent molars and is associated with loss of attachment and bone destruction leading to mobility of teeth. In the US, it is more common in blacks than the white population and can be inherited. In this case, the age and site are consistent with LAP but not the clinical presentation of loss of attachment and mobility. In addition, only one of the molars was affected in either site and the incisors were intact with no evidence of pathology. There was no family history of LAP.
As to localized prepubertal periodontitis (LPP), the site is consistent being the molars but the age of this patient is more on the older age range since LPP tends to occur more commonly in the primary dentition. Like LAP, this condition is more common in the black population and can be inherited as autosomal dominant.
Neither the clinical presentation, nor the histology is definitive for periodontitis
Sorry, you are incorrect!
If one is to consider OKC for the differential diagnosis of bilateral unilocular radiolucencies of the posterior mandible, one should be thinking more of the bifid rib basal cell nevus syndrome (Gorlin syndrome). It is exceptionally rare for multiple OKCs to occur in a non-syndromic patient. This patient’s age is consistent with the typical age for OKCs to occur in this syndrome.
Gorlin syndrome is an autosomal dominant condition involving the jaw bones, skin, central nervous system and the skeletal system. It is a condition with almost 100 signs and symptoms. The clinical symptoms of this syndrome range from multiple and recurring OKCs, intracranial calcifications, multiple and recurring basal cell carcinomas of the skin to a rare occurrence of medulloblastoma. Basal cell carcinomas occur between 13 and 30 years of age but have been described as early as two years of age. The face is characterized by hypertelorism, frontal bulging, sunken eyes, heavy and fused eyebrows, etc. Jaws present with either multiple or single and recurring OKCs. The syndrome-related OKCs occur after age 7 and peak at the second and third decades. Occasionally they do not occur until after age 40. They are more common in the mandible than maxilla. Histologically, OKCs in the syndrome have the same histology as non-syndrome OKCs. The same applies to all other lesions including the basal cell carcinomas.
This patient had none of the clinical symptoms described above and there was no family history of this syndrome. The histology is also not consistent with OKC.