Small unilocular radiolucent lesion mesial to tooth #21
Can you make the correct diagnosis?
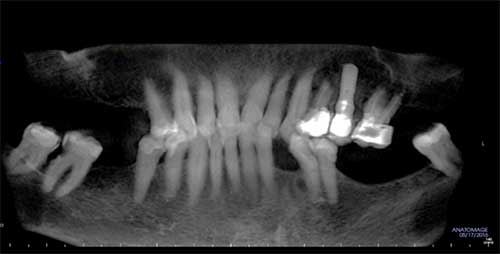
This is a 68-year-old Caucasian female who presented to a periodontal office for evaluation of the area of extracted tooth #22 in preparation for the placement of a dental implant.
Differential Diagnosis
1. Lateral periodontal cyst (LPC)
2. Odontogenic keratocyst
3. Squamous odontogenic tumor (SOT)
4. Central giant cell granuloma (CGCG)
5. Central odontogenic fibroma with giant cell reaction
Sorry, you are incorrect!
The site of the lesion being in the mandibular and bicuspid area, the lack of clinical symptoms, the patient’s age (over 30 years), and the radiographic findings of a well-demarcated unilocular radiolucency in the superior third of the root are all findings that are consistent with the favored diagnosis of lateral periodontal cyst. The gender of the patient is not consistent with LPC. The histology is also not consistent with LPC.
Sorry, you are incorrect!
A well-demarcated unilocular radiolucency with no clinical evidence of expansion or other symptoms is also consistent with odontogenic keratocyst (OKC). The site of the lesion being on the superior third of the root is unusual for an OKC, which tends to occur in the inferior third of the root when present between teeth. The lesion being in the bicuspid area is unusual for OKC, as nearly 80% of these cysts occur in the molar/ramus area of the mandible. OKCs are usually described in patients aged 10-40 years, but these cysts have been described in a wide age range. OKCs tend to occur more in males. The histology is not consistent with OKC.
Sorry, you are incorrect!
The small, well-demarcated radiolucency should bring to mind a diagnosis of a cyst rather than a neoplasm, especially when the lesion is present in the superior third of the root. However, a slow-growing, benign neoplasm like a squamous odontogenic tumor cannot be ruled out based on size alone. The patient’s age is on the older side but is consistent with SOT. The gender does not apply since SOTs are not gender specific. The well-demarcated nature of this radiolucency is consistent with the clinical presentation of SOT, but the lack of expansion and clinical symptoms such as pain point away from this diagnosis. SOTs tend to be painful, expansile, and may cause tooth mobility. The gross appearance of dark-brown is also not consistent with SOT. The histology is not consistent with SOT.
Sorry, you are incorrect!
Central giant cell granulomas tend to occur anterior to the first molar and more commonly in the mandible. They usually present as a single, well-demarcated, multilocular, and expansile radiolucent lesion, but can also present as a unilocular radiolucency. The nonexpansile nature of this patient’s lesion is not consistent with CGCG. The patient’s gender is consistent with CGCG, as it is twice as likely to occur in females than in males. However, the age of this patient argues against CGCG, as over 60% of cases occur in patients younger than 30 years of age. The histology of this case has a component with CGCG-like features.
Congratulations, you are correct!
The histology in this case is that of a combined central odontogenic tumor associated with a central giant cell granuloma-like reaction. For more discussion on this condition please refer to last month’s case of the month (May 2017). This month, we present another case of the so-called “hybrid tumor,” central odontogenic fibroma and CGCG-like lesion or central odontogenic fibroma with giant cell reaction and others. This a unique case because it was discovered as an incidental finding on CBCT imaging obtained in preparation for an implant placement in the area of missing tooth #22
This condition is reported more commonly in the mandible, particularly in the premolar/molar area. These lesions have been described in a wide age range of 5-73 years, with a predilection for the first three decades of life. They are more commonly found in females as demonstrated in several reports, with the exception of two case series in which where males were predominant. Radiographically, they are expansile, unilocular or multilocular radiolucencies that may perforate bone. We present a case that was not clinically symptomatic adding to the spectrum of the clinical presentation of this condition. Recurrence has been described, with one particular report describing recurrence in two out of eight cases.