Multilocular Radiolucent/Radiopaque Lesion, Anterior Mandible
Can you make the correct diagnosis?
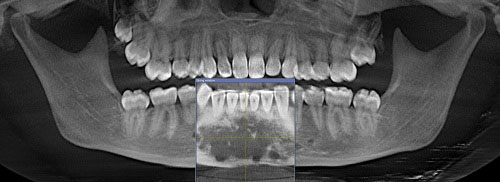
This is a 17-year-old female with expanding anterior mandible. A panoramic view of the anterior mandible shows a large and slightly well-demarcated multilocular radiolucent lesion interspersed with foci of mixed radiolucent/radiopaque component.
Sorry! you are incorrect
The location and the presentation of a multilocular radiolucency with a scalloped border are characteristics of glandular odontogenic cyst (GOC); for that reason, it should be considered on the differential diagnosis. The age of the patient, the gender and the areas of mixed radiolucent/radiopaque radiographic presentation are not supportive of GOC. The histology is also not supportive of a cyst, including GOC.
Glandular odontogenic cyst is a developmental cyst of tooth origin characterized by unusual lining epithelium and occasional aggressive behavior. The uniqueness of this cyst lies in its histology. The lining epithelium is stratified squamous in type, but covered by cuboidal or columnar cells (sometimes ciliated) interspersed with microcystic spaces simulating salivary gland ducts, giving rise to the name “glandular.” It is a rare cyst and, though mostly inert, it can sometimes be aggressive in behavior. Because it occurs in association with teeth, it is believed to be of tooth origin and not of salivary gland origin. Glandular odontogenic cyst was first described in 1987 and was initially called sialodontogenic cyst. Its name was later modified to GOC since it is not of salivary gland origin. It is more common in adults of an average age of 49, with slight male predominance. It has, however, been reported in all age ranges, including teenagers. It occurs three times more commonly in the mandible than in the maxilla, especially in the anterior mandible. Radiographically, they tend to present as unilocular and, less commonly, as multilocular radiolucencies. Multilocular GOCs tend to recur more than unilocular ones. These lesions grow to large sizes in the majority of cases and can perforate bone in a manner similar to the behavior of odontogenic keratocyst, a known aggressive cyst of tooth origin. Like OKCs, GOCs can be aggressive in terms of bone destruction and recurrence rate. Histologically, GOC has some features that can be similar to those of a dentigerous cyst: mucous cell metaplasia, with botryoid odontogenic cyst, and, at times, low-grade intra-osseous mucoepidermoid carcinoma. Treatment depends on the lesion’s size and radiographic features. Enucleation and curettage have been successfully used with the smaller and unilocular radiolucent lesions, while en bloc resection is used with the larger and more multilocular lesions since they tend to behave more aggressively. Some are treated with a combination of curettage and Carnoy’s or liquid nitrogen cauterization. The recurrence rate range is 21-55%. Enucleation and curettage alone carry a high recurrence rate of 25%. Marsupialization has been successfully used; in one case, the decompression was continued for two years. It showed gradual reduction of the size of the cavity bone fill and reservation of the contour of the maxillary sinus walls.
Sorry! you are incorrect
The age of this patient is within the age range in which this neoplasm is likely to occur, and the radiographic findings are also suggestive of this condition. The location, however, is not typical of juvenile ossifying fibroma. The histology is not supportive of this condition.
Juvenile ossifying fibroma (JOF) is a rare benign but aggressively behaving neoplasm of fibro-osseous origin that affects the jaws and craniofacial bones. It is an aggressive variant of a more common benign jaw bone neoplasm known as central ossifying fibroma (COF) occurring more commonly in the posterior mandible, inferior to the premolar and molar teeth with a distinct predilection for occurrence in females at a 5:1 ratio around 35 years of age. Central ossifying fibroma grows in a centrifugal manner; it can expand the bone buccally and lingually as well as superior and inferior aspects. It is radiographically diagnostic in that it is well demarcated with a corticated border and the central portion of the neoplasm ranges from radiolucent (early stages) to mature radiopacity (late stages) with a connective tissue capsule radiographically identified as a radiolucent rim.
Juvenile ossifying fibroma of the jaws, although a variant of COF, is distinct in several respects: its behavior, the location, the age of the patient and histologic features. As mentioned previously, this neoplasm is locally aggressive. It can simulate the behavior of a low-grade sarcoma with its tendency for fast growth, invading the surrounding tissue and destroying bone, displacing teeth and, at times, causing exophthalmos and diplopia. Tenderness and mild pain is also described, but not paresthesia, as was the case in this patient. It is more common in the maxilla and the craniofacial bones and sinuses.
Two histologic variants of JOF are described: trabecular and psammomatoid types. Trabecular JOF is histologically characterized by cellular connective tissue stroma interspersed with strands of trabeculae young bone with prominent osteoblastic rimming. Psammomatoid JOF is characterized by cellular connective tissue stroma with small and uniform cementum-like hard tissue resembling Psammoma bodies. Trabecular JOF occurs more commonly in the jaw bones; it is about twice as common in the maxilla as in the mandible. The psammomatoid type occurs more commonly in the paranasal sinuses. Both types are suggested to be of equal gender predilection or slightly more common in males. Psammomatoid JOF occurs more commonly in the paranasal sinuses (about 70% of cases) with 20% of cases occurring in the maxilla and 10% in the mandible. Generally, JOF is more common in children under 15 years of age; trabecular JOF tends to occur in younger patients with a range of 8.5-12 years while psammomatoid JOF affects older children with a mean age of 20-22. This patient’s case was more trabecular in type mixed with areas of psammomatoid morphology.
Radiographically, JOF ranges from a well-demarcated radiolucency, as is the case in this patient, to mixed radiolucent/radiopaque or predominantly radiopaque depending on the stage of the disease and degree of calcification. It can be unilocular or multilocular, well defined or ill defined. Both histological types have a high recurrence rate ranging from 30 to 56%. Treatment ranges from thorough curettage to resection to curettage with subcutaneous interferon injections. The latter has been reported to be effective in inhibiting tumor growth and recurrence.
Sorry! you are incorrect
The age of this patient, the swelling, and the location in the anterior mandible crossing the midline are all clinical characteristics that can be consistent with central giant cell granuloma (CGCG). The histology, however, is not supportive of CGCG.
Jaffe first coined the term “reparative” for central giant cell granuloma. Most pathologists have since dropped the term “reparative” for lack of evidence that the pathogenesis is a reparative process. CGCG is described as a non-neoplastic process and yet can behave in a very aggressive and expansile manner, destroying bone and displacing teeth. Over 60% of CGCG cases occur in patients younger than 30 years of age, with twice as many occurrences in females as in males. CGCG is classified into aggressive and non-aggressive types; the aggressive type tends to occur in younger patients and causes disfiguration, especially after surgery. Over 70% of cases occur in the mandible anterior to the first molar tooth. This lesion has also been described in other cranio-facial and small long bones such as those of the hands and feet.
The usual treatment for CGCG is surgery, ranging from curettage and en bloc to resection. The latter is used in aggressive and recurring cases. In the past ten years or so, alternatives to surgery have emerged with successful results, saving some patients from facial disfigurement. Steroid injections are the most successful alternative treatment thus far; they require injections weekly or every 2-3 weeks, have no known side effects (even in children), and are the least expensive alternative treatment. Other treatments include: calcitonin injections or nasal spray, which require daily injections or a nasal spray of salmon calcitonin for about a year and are safe for pregnant females; and interferon alfa-2a injections, which are administered 2-3 times per week for several months and are the most expensive alternative treatment. A report by Carlos and Sedano from Guatemala presented four patients with large CGCG cases treated with steroid injections. They demonstrated that regular steroid injections led to remarkable responses in all four patients without any side effects. All four patients had initial biopsies confirming the histological diagnosis of CGCG and had endocrine testing to rule out hyperparathyroidism. Two were pediatric patients, two-and-a-half and six years of age, with large lesions of the mandible and maxilla, respectively. They responded more rapidly to steroid injections than did the other two patients, who were adults of 31 and 34 years of age with large lesions of the maxilla and mandible, respectively. Injections were administered every two to three weeks. Complete healing, with small residual radiolucency requiring no further treatment, was noted in three of the patients. One patient, the six-year-old boy, had a maxillary swelling that was reduced from 5 cm in size to only 0.5 cm after four injections. The surgical specimen from the six-year-old consisted of fibrocollagenous stroma with few giant cells in comparison to the original biopsy, which consisted of loose and vascular granulation tissue with many giant cells. Fibrocollagenous stroma, with or without giant cells, has been described in association with both calcitonin and steroid treatment. There was no evidence of recurrence in these patients after 2-7 years of follow-up, nor were there any steroid-related complications in any of the patients. One must keep in mind that this report involves a very small number of cases; few firm conclusions can be reached, but the results are remarkable and show a more favorable outcome than surgical intervention, particularly in large and aggressively behaving pediatric cases.
Congratulations! You are correct
The radiographic changes, the clinical behavior of expansion and the age of the patient are all consistent with fibrous dysplasia. Although the location is unusual for FD, it can still be included on the differential diagnosis. The histology is supportive of FD.
The etiology of fibrous dysplasia is unknown. The monostotic (one bone or bone complex area) form makes up approximately 80% of all fibrous dysplasia cases; the polyostotic form affects one or more bones with multiple lesions. FDs are expansile and disfiguring lesions, whether single or multiple, which differentiates them from the usually flat osteomas of Gardner’s syndrome. Monostotic FD, which involves the jaws, affects males and females equally. It occurs in childhood and at puberty and usually stops growing at age 30. It appears as an asymptomatic swelling of the maxilla or mandible; maxillary lesions are the most common. It may involve bones other than the maxilla, such as the zygoma and the sphenoid. It is usually unilateral and is known to displace the teeth, but otherwise is firmly seated. The growth is usually slow, but rapid growth has been described, especially during puberty. The radiographic appearance, especially of the maxilla, is classically described as a ground glass appearance where fine radiopacity is noted. The mandibular lesions are much more deceptive because they tend to vary more, thus making diagnosis with a radiograph difficult. They may consist of a cystic unilocular radiolucency, multilocular radiolucency, or the classical ground glass radio-opacity. Treatment may be necessary and is preferably performed after cessation of growth due to the high incidence of re-growth and requirement for secondary procedures. Radiation therapy is contraindicated since significant incidence of development of osteosarcoma in the irradiated bone has been documented. Malignancies such as osteosarcoma arising in an area of FD that has not been irradiated have been described, but rarely; these occur mainly in irradiated lesions. The overall prognosis is good with close follow-up.