Right mandible: mixed RL/RO Expansile Lesion
Can you make the correct diagnosis?
This is a 26-year-old male who was referred to an oral surgeon for the evaluation and treatment of his wisdom teeth and a large “cyst” involving tooth
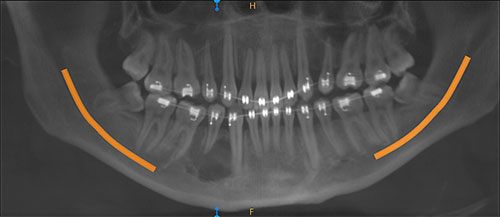
Sorry, you are incorrect!
The differential diagnosis (DDX) in this case is isolated to those conditions that present radiographically as mixed radiolucent (RL) and radiopaque (RO) lesions. Lesions that are not hard-tissue producing, such as giant cell granulomas, will not be considered. Bony septa are not tumor producing hard tissue.
Central odontogenic fibroma (COF) is a mixed RL/RO lesion capable of producing flecks of hard tissue; therefore, it should be considered in this DDX. The site, age, gender, expansion, and mixed RO/RL radiographic morphology are all consistent with the clinical presentation of central odontogenic fibroma, as is the slow growth and tooth resorption. Central odontogenic fibroma is an odontogenic neoplasm of mesenchymal origin that is not common. Gardner classified this neoplasm into 2 types: “simple” and WHO. It tends to occur more in the first two decades of life, but with a wide age range of 5-80 years of age. It is more common in female children; the female-to-male ratio of occurrence in children may be 7:1. It tends to occur equally in the maxilla and mandible. In the maxilla, it occurs anterior to the first molar tooth while in the mandible it tends to occur in the posterior. Clinically, COFs present with swelling and can resorb and displace teeth. Radiographically, they present as unilocular or multilocular expansile lesions. They are radiolucent or mixed RL/RO lesions. They are usually slow growing. Simple surgical excision is the treatment of choice. It has a good prognosis. The histology is not consistent with central odontogenic fibroma.
Sorry, you are incorrect!
The mixed RL/RO findings and the slow-growing expansile lesion in this case are consistent with COC. The site in this case is slightly more posterior than the most common area of occurrence for COC, which is the anterior mandible. The age of the patient is also consistent with typical COC occurrence, which is around 30 years of age with a wide age range. The histology, however, is not supportive of COC.
Calcifying odontogenic cyst is not a common condition, accounting for only 1% of jaw cysts. This condition represents a spectrum of histologies including a simple cyst, a cyst with an odontoma, a cyst with ameloblastomatous proliferations and a more aggressive solid neoplasm, also known as “ghost cell odontogenic tumor,” with a potential to transform especially with multiple recurrences. Calcifying odontogenic cyst is also described on the gingiva alone without a bony component in up to 20% of cases (peripheral COC). Intrabony COC presents as a well-circumscribed unilocular radiolucency with flecks or masses of radiopaque material. The size and amount of the radiopaque material varies. It can expand bone and displace and resorb teeth. In about one third of cases, COC is associated with unerupted teeth, usually the canine tooth. The most common locations are the anterior jaws in the incisor-canine area. This cyst may also be associated with an odontoma, usually complex in type. It can occur at any age, but is most common in patients around 30 years of age; in contrast, odontoma-associated COCs tend to occur in younger females around the age of 17. The solid odontogenic ghost cell tumor is the least common type, but it behaves more aggressively than the others. These lesions are usually conservatively treated by thorough curettage and heal uneventfully. The solid type tends to recur and, for that reason, follow-up visits are recommended. With recurrence, a more aggressive treatment is recommended to prevent further recurrence.
Sorry, you are incorrect!
The site, age of the patient, and radiographic findings of a mixed RL/RO and expansile lesion are all consistent with the clinical and radiographic presentation of Pindborg tumor. The patient’s gender is also supportive of this diagnosis since CEOT has equal gender presentation. The histology in this case, however, is not supportive of CEOT/Pindborg tumor.
Pindborg tumors constitute fewer than 1% of odontogenic tumors. The age of this patient is within the most common age range for this condition, which clusters around 30-50 years. Pindborg tumor has an equal gender distribution. The site is also consistent with this condition since close to 75% of Pindborg tumors occur in the posterior mandible. CEOT is expansile but otherwise asymptomatic, which is consistent with the behavior of this case. Pindborg tumor, like ameloblastoma is a benign but locally aggressive neoplasm that resorbs and displaces teeth and expands the jaw. Radiographically, CEOT presents in several patterns ranging from a well-circumscribed unilocular radiolucency with radiopacity to a multilocular “honeycomb” radiolucency with flecks of radiopaque material, as is the case in this patient.
Congratulations, you are correct!
The radiographic findings of an expansile, mixed RL/RO lesion causing tooth resorption is supportive of a diagnosis of juvenile ossifying fibroma (JOF). The gender of the patient is consistent with JOF. The site is not supportive of JOF and the patient’s age is older than that of most patients with this condition. The histology, however, is that of JOF.
Juvenile ossifying fibroma (JOF) is a benign neoplasm of bone origin and is an aggressive variant of central ossifying fibroma of the jaws. It is by far more common in children under the age of 15. It is most common in the craniofacial bone, especially the maxilla. Two histologic variants are described: trabecular and psammomatoid types. The histology of this case is consistent with that of trabecular JOF. Trabecular JOF occurs more commonly in the jaw bones; it is about twice as common in the maxilla as in the mandible. Psammomatoid JOF occurs more commonly in the paranasal sinuses (about 70% of cases) with 20% of cases occurring in the maxilla and 10% in the mandible. Trabecular JOF tends to occur in younger patients with a range of 8.5-12 years while psammomatoid JOF affects older children and young adults with a mean age of 20-22. Both types are slightly more common in males. Both types are benign but locally aggressive lesions simulating low-grade sarcoma behavior with a tendency for fast growth, invading the surrounding tissue and destroying bone. Both histological types have a high recurrence rate ranging from 30 to 56%. Treatment ranges from thorough curettage to resection to curettage with systemic subcutaneous interferon injections. The latter is reported to be effective in inhibiting tumor growth and recurrence.