Large multilocular expansile radiolucency: left posterior mandible
Can you make the correct diagnosis?
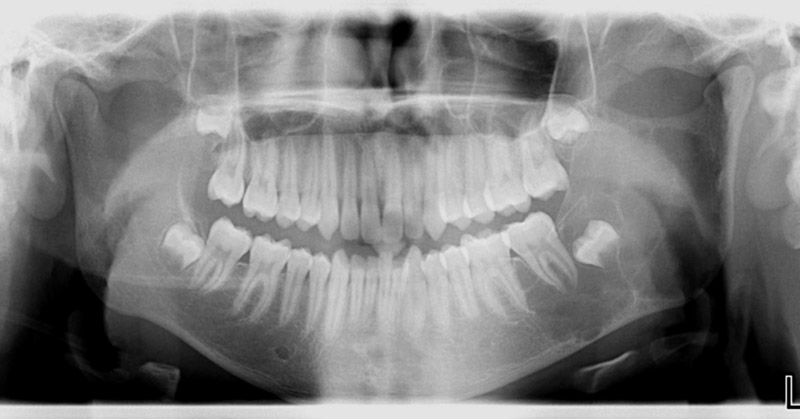
This is a 15-year-old male was referred to an oral for an incidental finding of a well-demarcated, expansile and multilocular radiolucency, left posterior mandible in area of teeth #s 17 and 18 extending partly into the ramus (Figure 1).
Congratulations, you are correct!
The site being posterior mandible, the expansion; the multilocular radiolucency and age of the patient are all consistent with the diagnosis of aneurysmal bone cyst (ABC) which, in this case, should be placed high on the list of the differential diagnosis. Although this lesion is expansile, it is not “ballooning” the jaw as conventional ABC usually presents; a point worth keeping in mind. The clinical description of the surgical site containing areas of “purplish sinusoids” is also consistent with that of the clinical presentation of ABC. The histology is consistent with ABC.
Aneurysmal bone cyst is a disease of the young, usually occurs before the age 20. There is a slight predilection for females and is more common in the posterior mandible. Clinical Features include pain and swelling. Radiographically, ABC presents as multilocular or honeycombed expansile radiolucency with thinning leading to ballooning or ‘blow out’ distention of bone which is highly suggestive of ABC. The histology was that of highly vascular and hemorrhagic granulation tissue with dilated and congested blood vessels and giant cells. Typical features of sinusoids were not identified but spaces lined by occasional giant cells were identified.
Sorry, you are incorrect!
The location in the posterior mandible; the expansion; and the multilocular radiolucency are all typical of solid ameloblastoma. The lack of significant teeth displacement and the young age of this patient argue against solid ameloblastoma. The histology is not consistent with solid ameloblastoma.
Solid ameloblastoma is one of the most common benign neoplasms of odontogenic origin. It is locally aggressive; it is slow-growing and persistent. It affects a wide range of age distribution but is mostly a disease of adults, at an average age of 33, with equal sex distribution. About 85% of ameloblastomas occur in the posterior mandible; most of these occur in the molar-ramus area. Solid ameloblastomas in general are characteristically expansile, radiolucent and multilocular in nature. They can move teeth apart and resorb teeth. They can perforate bone.
Sorry, you are incorrect!
The site being in the posterior mandible is favorable to myxoma. The multilocular and expansile radiolucency is also supportive of the diagnosis of odontogenic myxoma. The age of this patient is on the young age range and the lack of significant teeth displacement argues against myxoma. The histology is not consistent odontogenic myxoma.
Odontogenic myxoma is not common; it usually occurs in jaw bones, in the tooth-bearing areas of the jaw. It is benign, but locally aggressive neoplasm. It has the potential for extensive bony destruction and extension into the surrounding structures. Almost 75% of odontogenic myxomas occur in patients around 23-30 years of age with a slight female predilection (1:1.5 male-to-female ratio). It rarely occurs in patients over 50 or under 10 years of age. It occurs almost equally in the maxilla and mandible with a slight predilection for the posterior mandible. Most cases are expansile and can displace and resorb teeth. Radiographically, the majority present as expansile and multilocular, though some are unilocular with or without scalloped borders, and rare cases present with a diffuse and mottled appearance which can be mistaken for a malignant neoplasm.
Sorry, you are incorrect!
The age and gender are consistent with TBC. The lack of significant displacement of teeth is also consistent with TBC. The clinical description of “aspirating straw-colored fluid” and that the cavity appeared “empty;” are also consistent with the clinical presentation of TBC. However, the expansile multilocular radiographic appearance can, on rare occasions, be consistent with TBC but very rare. The erosion of the inferior border of the mandible argues against TBC. The clinical description of purplish sinusoids present within the surgical site argues against TBC as well. The histology shows significant amount of highly vascular and hemorrhage granulation tissue with small clusters of giant cells. The granulation tissue has congested and dilated blood vessels and what appear as spaces lined by few giant cells. The overall features of cellular and vascular granulation tissue with dilated blood vessels and giant cells arranged in clusters in some areas and at the periphery of one or two spaces are all features that argue against TBC
Traumatic bone cavity (TBC) is not unique to the jawbones; it is also described in the long bones and is known as a simple solitary bone cyst occurring mostly in the humerus or femur, close to the epiphyseal plate. It is more common in males between ages 10-20. Most reports agree that the average age of occurrence is below 20 years of age (6-7). Mandible is the most commonly affected area, where over 95% of the cases occur, especially in the posterior premolar-molar area. They rarely extend to the ramus. They are usually unilocular and radiolucent, typically above the alveolar canal and in many cases with a scalloped superior border spreading between the roots of teeth. Large, expansile and multilocular traumatic bone cavities have been described, but are rare.
Clinically, surgeons report an empty cavity at entrance in about two thirds of the cases and straw-colored fluid filled cavities in about one third of the cases. Blood clot is also present occasionally. The bony cavity is scraped to generate bleeding, which is considered the treatment of choice for this condition.