December 2005: Unilocular radiolucency right maxillary sinus
Dolphine Oda, BDS, MSc
doda@u.washington.edu
Can you make the correct diagnosis?
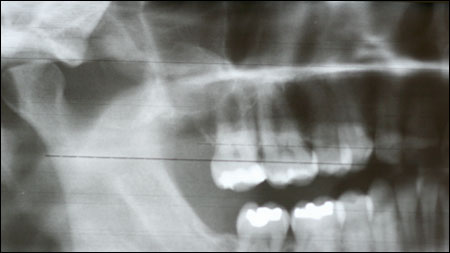
This is a 39-year-old white male who was referred by his ENT physician to Dr. Audia after refractory treatment for chronic sinusitis.
Sorry! you are incorrect
Ameloblastoma is one of the most common benign neoplasms of odontogenic origin. It accounts for 11% of all Odontogenic neoplasms/hamartomas (4-6). It is a slow-growing, persistent, and locally aggressive neoplasm of epithelial origin. It affects a wide range of age distribution but is mostly a disease of adults, at an average age of 33, with equal sex distribution. Reports from Africa and India show male predilection. It is prevalent in black patients (5).
About 85% of ameloblastomas occur in the posterior mandible, most in the molar-ramus area, some in the anterior mandible. About 15% occur in the maxilla, the vast majority in the posterior maxilla as is the case in our patient. Ameloblastomas of the maxilla tend to occur in older age population consistent with our patient (4-6). Ameloblastomas of the maxilla tend to have a worse prognosis than those of the mandible. They tend to recur more and behave more aggressively in terms of early invasion of the maxillary sinus (4, 6). They can also invade the optical nerve and the brain and kill the patient. The notion of ameloblastomas of the maxilla being more aggressive in behavior may be biological in nature such as the histologic type (plexiform ameloblastoma reported to be more aggressive than follicular ameloblastoma) or because of the anatomic location being difficult to reach surgically making complete eradication of a the neoplasm a challenge.
Ameloblastoma is rarely described in children. It is characteristically expansile, radiolucent and multilocular in nature. It can however be unilocular and associated with impacted teeth resembling a dentigerous cyst (4-6). The latter are known to be less aggressive than the multilocular solid lesions. Three clinical types of ameloblastoma are described, the solid type (radiographically multilocular), the cystic (radiographically unilocular and usually associated with an impacted tooth) and peripheral type (soft tissue usually gingival ameloblastoma) (4-6). Our case qualifies for the solid type, although radiographically was not multilocular in appearance. For more information on the behavior of the various types of ameloblastomas, please read the October 04 newsletter under clinical case discussion.
Ameloblastoma, if not treated, can reach very large sizes with facial disfiguring. It loosens, displaces and resorbs adjacent teeth. With the exception of jaw expansion, it is usually asymptomatic unless infected where it can be mildly painful. Parasthesia, anesthesia is extremely rare, unless they are very large in size. Also, ameloblastoma tends to expand rather than perforate the cortical bone. If the later occurs with extension into the adjacent soft tissue, it would have a higher tendency for recurrence and therefore would have a worse prognosis than those completely encased by bone (4-6).
As mentioned above, three clinical types of ameloblastomas are described, the solid being the most common is further subtyped histologically into follicular (most common type), acanthomatous sometimes mistaken for intrabony squamous cell carcinoma, plexiform favoring maxilla over the mandible and suggested to be more aggressive in behavior, granular cell, basal cell and desmoplastic types. The last three are the least common (6).
The solid type is treated with complete surgical removal with clean margins through resection or en bloc. Curettage is not recommended for the solid type because it is associated with a higher recurrence rate than the resected counterpart. Resected jaws may require secondary reconstruction (7). It has an overall good prognosis but is known to have high recurrence rate, particularly in the posterior maxilla, inadequate surgery (tumor extending to the surgical margins). Long-term follow-up is required. Recurrence is related to the treatment modality. The histology of this case is not supportive of ameloblastoma.
Congratulations! You are correct
Odontogenic keratocyst is an aggressive developmental odontogenic cyst known for its rapid growth and its tendency to invade the adjacent tissues, including bone. It has a high recurrence rate and is associated with bifid rib basal cell nevus syndrome (1, 2). The majority of patients are in the age ranges of 20-29 and 40-59, but cases in patients ranging in age from 5 to 80 years have been reported. The distribution between sexes varies from equal distribution to a male-to-female ratio of 1.6:1, except in children (1, 2). Odontogenic keratocyst predominantly affects Caucasian populations and, if one may judge from the limited evidence provided by the literature, is chiefly of Northern European descent (1).
Odontogenic keratocysts may occur in any part of the upper and lower jaw, with the majority (almost 70%) occurring in the posterior mandible and ascending ramus. They occur most commonly in the angle of the mandible and ramus (1). Maxilla is less commonly involved; a 2:1 mandible to maxilla ratio. In the maxilla, the third molar areas are the most common location followed by the anterior maxilla. The OKCs of the anterior maxilla tend to occur in older patients. Radiographically, OKCs present predominantly as unilocular radiolucencies with well-defined, sclerotic or scalloped borders. They may also present as multilocular radiolucencies. Odontogenic keratocysts of the maxilla are smaller in size when compared to those occurring in the mandible; larger OKCs tend to expand bone, but mildly—obvious clinical expansion should be viewed with suspicion for a neoplasm. OKCs can also present as small and oval radiolucencies between teeth simulating a lateral periodontal cyst, in an area of an extracted tooth simulating a residual cyst, at the apex of a vital tooth mistaken for a periapical cyst, or in the anterior maxilla between the central incisors simulating an incisive canal cyst (2). OKCs grow to sizes larger than any other odontogenic cysts. They usually penetrate the bone rather than expand it and grow in an anterior to posterior direction (3). Despite this aggressive growth, they often remain asymptomatic, thus growing to large sizes and hollowing the bone.
Odontogenic keratocysts are significant clinical entities due to their tendency for recurrence and destructive behavior. They are known to have a high recurrence rate, ranging from 13% to 60% (1, 2). Complete surgical removal is the treatment of choice. Surgery includes enucleation, curettage, enucleation and peripheral ostectomy, to resection depending on the radiographic presentation, location and clinical behavior. Surgery combined with Carnoy’s solution or liquid nitrogen treatment have been effective in reducing recurrence rate (1, 2). At times, adjacent or associated teeth are extracted in the interest of complete removal. Some investigators advocate marsupialization and occasionally resection of the more aggressive cysts that tend to perforate buccal and lingual bone. Resection is a rare modality of treatment. Most cysts recur within the first three years while others may recur as late as after 16 years (1, 2). Conservative surgical removal and long-term follow-up is the treatment of choice by most clinicians. The histology of this case is not supportive of Odontogenic keratocyst.
Treatment
An enucleation of the cyst with peripheral ossectomy was performed on October 24, 2005. Clinical findings revealed a well encapsulated cystic structure which was intimately associated with tooth #2. The cystic mass was removed in its entirety along with tooth #2 (Fig 5). A peripheral ossectomy was performed with a rotary instrument and curette. The snidarian membrane was preserved and the wound was closed primarily. The surgical soft tissue specimen and the tooth were submitted for microscopic evaluation. The histology of the cystic structure was consistent with that of the biopsy specimen.
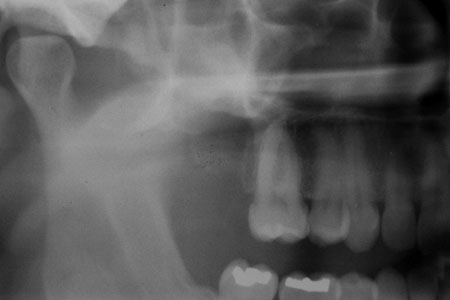
Figure 5. This is a panoramic radiograph taken after the cyst was surgically removed. The cyst was associated with the maxillary second molar. The cyst was curetted and tooth # 2 was extracted.
References
- Shear M. Odontogenic keratocysts: natural history and immunohistochemistry. Oral Maxillofacial Surg Clin N Am. 2003; 15: 347-362.
- Oda D, Rivera V et al. Odontogenic keratocyst: the northwestern USA experience. J Contemp Dent Pract. 2000 Feb 15; 1(2): 60-74.
- Zachariades N, Papanicolaou S, Triantafyllou D. Odontogenic keratocysts: Review of the literature and report of sixteen cases. J Oral Maxillofac Surg. 1985; 43: 177-182.
- Reichart PA, Philipsen HP, Sonner S. Ameloblastoma: biological profile of 3677 cases. Eur J Cancer B Oral Oncol 1995;31B:86–99.
- Adekeye EO, McLavery K. Recurrent ameloblastoma of the maxillofacial region. Clinical features and treatment. J Maxillofac Surg 1986;14:153-157.
- Gardner DG. Some current concepts on the pathology of ameloblastomas. J Oral Maxillofac Surg 1996;82:660-669.
- Omandi BI, Guthua SW, Awange DO et al. Maxillary obturator prosthesis rehabilitation following maxillectomy for ameloblastoma: case series of five patients. Int J Prosthodont. 2004;17:464-468.
- Roden MM, Zaoutis TE et al. Epidemiology and outcome of zygomycosis: a review of 929 reported cases . Clin Infect Dis. 2005;41:634-653.
- Safar A, Marsan J et al. Early identification of rhinocerebral mucormycosis. J Otolaryngol. 2005;34:166-1671.
- Vazquez JA, Zygomycosis, an update-March 2005. E-Medicine.com
Sorry! you are incorrect
Zygomycosis, or mucormycosis, is an opportunistic fungal infection that rarely affects immune competent individuals (8-10). The micro-organisms known as zygomycetes include Mucor, Rhizomucor and Rhizopus; these grow in soil and decaying fruits. They are opportunistic micro-organisms which cause disease in uncontrolled diabetics and in immune-compromised individuals such as AIDS patients, organ transplant patients, patients undergoing steroid therapy and patients with leukemia and lymphoma (8-10). Zygomycosis is transmitted through inhalation. The infection is usually acute and rapidly growing. This is a serious disease that tends to invade major blood vessels causing ischemia and necrosis; it may be fatal.
Zygomycosis can affect the head and neck area (rhinocerebral), the lungs, the skin, or the abdomen, or it can be a general disease. The rhinocerebral type is the most common as well as the most serious, affecting mostly uncontrolled insulin-dependent diabetics with acidosis. It involves the sinuses, nose, eyes, brain and occasionally the meninges. It has a poor prognosis, with an 85% mortality rate (10).
The clinical presentation may include headache, facial pain, nasal congestion, epistaxis, swelling of the palate and maxillary alveolar ridge (9-10). In more advanced cases, black necrosis of the palate and overlying mucosa and skin may occur if the condition is not treated.
Radiographically, the disease is not easily diagnosed. A panoramic radiograph may demonstrate radiopacity with bony effacement and mucosal thickening while a CT scan may show a clearer picture of bone and soft tissue destruction (8-10).
A tissue biopsy is the more reliable method of diagnosis. The micro-organisms are identified by both the hematoxylin and eosin stain and by special stains for fungal micro-organisms. Treatment includes thorough surgical curettage, antifungal infection and correction of the diabetes acidosis. This patient is not diabetic or immune compromised and the histology is not supportive of zygomycosis.
Sorry! you are incorrect
The posterior hard palate, anterior and posterior soft palate are the ideal locations for malignant salivary gland neoplasms such as adenoid cystic carcinoma, mucoepidermoid carcinoma and polymorphous low grade adenocarcinoma. Although the latter does not readily invade bone, the former two do. These neoplasms usually present as swellings in the soft tissue of the palate, at times however, they may be hidden and grow inwardly into the palate and maxillary sinus rather than the usual outward, visible swelling.
We also need to emphasize that although, the palate is the most common oral location for these neoplasms, malignant salivary gland neoplasms can also arise within the sinus salivary gland tissue.
Salivary gland neoplasms in general favor adults with equal sex distribution (sometimes favoring females). They are slow-growing and asymptomatic. Adenoid cystic carcinoma and polymorphous low grade adenocarcinoma tend to invade nerve, therefore leading to clinical symptoms ranging from pain to anesthesia. Nerve invasion is characteristically a sign of advanced disease. Neither, the histology nor the clinical presentation of this case are supportive of a salivary gland neoplasm diagnosis.