Generalized Ulcerative Palate and Maxillary and Mandibular Gingiva
Can you make the correct diagnosis?
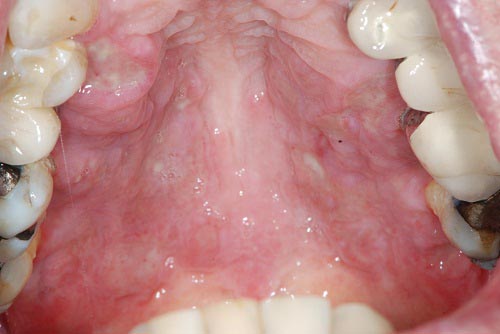
This is an 82-year-old white male who first presented to the UW otolaryngology clinic for ear pain, drainage and hearing loss.
Sorry! you are incorrect
The presentation of generalized and mostly superficial oral ulcers combined with the age of the patient, his health status, and the medications he is on should lead to the consideration of lichenoid drug reaction as part of the differential diagnosis. However, lichen planus/lichenoid drug reaction most commonly presents as symmetrical bilateral buccal mucosa/vestibule lesions, followed in frequency of location by the dorsal/lateral tongue and gingiva. It is highly unusual for lichenoid drug reaction to only involve the gingiva and it is certainly not common on the palate. The histology of this specimen was not supportive of lichen planus or lichenoid drug reaction.
Lichen planus, a common chronic immune mediated disease affecting 1-2% of the population, has a variety of clinical presentations, management, and predisposing factors that render it a family of diseases rather than one entity with a specific treatment modality. To be specific, lichen planus can be immune mediated, drug induced, associated with transplant rejection (also known as graft versus host disease), or associated with galvanic effect (when two separate restorations are in opposite contact with each other). It is also seen in families (though rarely), and is known to undergo a malignant transformation in about 2.5% of cases. Given the versatility of this disease, it is difficult to apply one treatment modality for all presentations.
The most common type of LP is the chronic T-lymphocyte-mediated disease where CD4 (early stage) and CD8 (later stages) T-lymphocytes are stimulated, releasing lymphokines such as tumor necrosis factor which lead to the destruction of the cells in the basal and parabasal cell layers. This type of oral LP tends to come and go, sometimes lasting a lifetime. Lichen planus of the skin usually resolves within 1-3 years while only 20% of oral LP cases resolve in that period of time. Lichen planus occurs in adults between 30 and 70 years of age with a strong female predilection. It is often associated with stressful lifestyles. Skin LP presents as purplish, pruritic papules with a white keratotic surface, commonly on the flexor surfaces of the wrists, trunk and the genitalia. Oral LP presents as keratotic and reticular (the reticular pattern is the most common type), atrophic or erosive (the erosive type is the most important clinically), or plaque-like (the hypertrophic type, which is the least common). Oral LP presents most commonly in a symmetrical manner on the bilateral buccal mucosa, followed by tongue and gingiva. Reticular type LP is asymptomatic and presents with interlacing lines against an erythematosus bluish background; the lines are known as the striae of Wickham. Erosive type LP, on the other hand, is symptomatic—patients complain of sensitivity to hot and cold, spicy, acidic, and alcoholic food and beverages. Erosive LP also presents in locations similar to those of the reticular type. At times, erosive LP can be hard to distinguish from other mucocutaneous diseases such as benign mucous membrane pemphigoid (BMMP) and pemphigus vulgaris (PV). Hyperplastic or plaque LP is uncommon and presents as a confluent white plaque often mistaken for leukoplakia. The hyperplastic type is more common on the dorsal surface of the tongue, gingiva, and palate, making a clinical diagnosis of LP difficult at times, especially if the patient is a smoker. LP can also present on the gingiva alone as a thin and atrophic lesion known as desquamative gingivitis. The clinical differential diagnosis for desquamative gingivitis should include BMMP and PV. A discussion of LP would be incomplete without addressing Lichenoid Drug Reaction, a condition that is especially common in elderly patients. It most frequently presents as erosive lichen planus on the bilateral buccal mucosa. It is associated with the ingestion of a number of medications, including antibiotics, antihypertensive drugs, allopurinol (gout), diuretics, antidiabetics, gold, mercury, antibiotics, and antihistamines, among many others. The malignant potential of oral LP is a significant clinical concern, especially in long-term erosive lichen planus patients; transformation in reticular LP has also been documented, but rarely. The World Health Organization (WHO) defines oral LP as a precancerous condition with the understanding that the risk for transformation is very small, around 2.5%. The locations of transformation are not in the high-risk locations of the conventional oral SCC, but rather involve the buccal mucosa, tongue and gingiva—the same locations as conventional lichen planus.
Treatment ranges from no treatment for the asymptomatic reticular type, to topical steroids, to intralesional steroid therapy (rarely used), to systemic steroid therapy (if the condition is severe such as in erosive LP). The best treatment for lichenoid drug reaction is replacement of the medication causing the condition with a substitute. Treatment for transformation would follow the criteria for the treatment of oral squamous cell carcinoma, which are described in the April 2004 Case of the Month.
Sorry! you are incorrect
Any drug, including over-the-counter drugs, can cause erythema multiforme (EM) of the oral cavity. Given that elderly patients can be taking both prescription medications and over-the-counter supplements, it is important to consider drug-induced oral ulcers on the differential diagnosis of generalized and superficial oral ulcers. However, the histology in this case did not support the diagnosis of EM.
Erythema multiforme is a skin and mucous membrane disease that can cause rashes, bullae, ulcers and epithelial sloughing (skin peeling, which is more common in TEN). It is an IgE immune-mediated hypersensitivity reaction most frequently caused by drug intake, especially that of sulfa drugs; this is not the case with our patient. Erythema multiforme can also be a sequel to viral or mycoplasma infections, and occasionally to an underlying malignant neoplasm or a gastrointestinal disease. It affects both the skin and mucous membranes. Skin lesions are usually the first to appear, followed by mucous membrane blistering and ulcerations, although the reverse is also possible. They present with a rash on the extremities, progressing to the back, buttocks, chest and other skin areas. Areas of mucous membrane occurrence include the mouth, eyes (where it may lead to blindness), genitalia, gastrointestinal tract and respiratory tract. The latter two are serious, especially if they lead to esophageal stricture and respiratory failure due to severe epithelial sloughing. In the oral cavity, EM is more often related to drug reaction, especially sulfa drugs. It presents in acute and chronic types with varying degrees of severity. It may be life-threatening, especially in children. Antibodies target the epithelium and superficial blood vessels, leading to epithelial ulceration, sloughing and vascular leakage. Clinically, it is most common in young males (2:1 M:F ratio) between ages 20-40. It may also affect children. Diagnosis is often made on the basis of the clinical presentation. Neither the hematoxylin and eosine histology nor the immunofluorescence antibody stain is specific. Treatment includes the withdrawal of the causing drug if determined, fluids, supportive care, systemic steroids and immune suppressants dependent on severity. The bullae and ulcers may continue to appear even after the causative agent is discontinued. It takes six to eight weeks for the epithelial lesions to heal. The prognosis is determined clinically on a scoring system known as SCORTEN (grades 1-5); the higher the number, the worse the prognosis. For example, the mortality rate of grade 5 is over 90%.
Sorry! you are incorrect
Generalized and mostly superficial ulcers mostly affecting the gingiva should make one think of benign mucous membrane pemphigoid. However, the ulcers in this case involved the hard palate just as much as the gingiva, which is not typical of BMMP. This disease should nevertheless be part of the differential diagnosis because, if not treated, BMMP can involve the palate and other areas; in this case, the patient has had these ulcers for at least six months. The age and gender are also unusual for BMMP. The histology of this specimen was not supportive of BMMP.
Mucous membrane pemphigoid (MMP) is the preferred name for the overall disease process. It is more common in females (2:1 F:M ratio) around 50-60 years of age. Like many of the vesiculobullous diseases, MMP is a chronic autoimmune disease predominantly affecting mucosa. The oral mucous membrane, specifically the gingiva, is more commonly affected. The immune system recognizes multiple antigens in the region around the basement membrane as foreign, forming a complex attracting inflammatory cells which leads to a separation of the surface epithelium from the connective tissue. As opposed to eye and nose lesions, which tend to heal with scarring, oral lesions may heal without scarring. The oral cavity tends to be the first site of the disease target; it occurs twice as often on the gingiva as “desquamative gingivitis” as it does in any other location. The next most common locations are the eyes (where it can cause blindness through scarring), nose, nasopharynx, genitalia, skin, larynx and esophagus. Patients with MMP may have circulating antibodies.
In the oral cavity, it presents as red gingival patches with loss of stippling. There may be sloughing and desquamation of the epithelium, especially as a result of mechanical pressure such as from brushing and denture irritation. If not treated, it may extend to the palate, tongue, buccal mucosa and other areas in the mouth. It shows a positive Nikolsky sign. A minimum of 12-25% of MMP cases involve the eyes. Histopathology: Sub-basilar split of the intact surface epithelium from the underlying fibrous connective tissue with an intact basal cell layer as part of the detached epithelium. Many inflammatory cells, including eosinophils, are present. Immunofluorescent studies are useful in rendering a definitive diagnosis. MMP is usually positive with IgG and C3 antibodies present in form of uniform line along the basement membrane. The best biopsy site to rule out MMP is a perilesional area rather than the sloughing and detached area. Treatment includes local and systemic steroids and immune suppressants, depending on the severity of the disease. Antibiotics for secondary infections are also prescribed. The histology and IMF studies of this case were not supportive of MMP.
Congratulations! You are correct
Langerhans cell histiocytosis (LCH) is a disease of children under 5 years of age. It is extremely rare in the elderly population, among whom the estimated occurrence rate is 1-2 cases per million. In these cases, LCH tends to be limited to the skin and, as in this case, limited to the oral mucosa, mainly the hard palate and gingiva. Langerhans cell histiocytosis of the oral cavity usually affects the bone, especially the mandible, and is usually isolated but can present in multiples.
Langerhans cells are dendritic cells of bone-marrow origin. LCH is generally a disease of children under 5 with extremely rare occurrence in adults. The former name for this condition is histiocytosis X, which was classified into three types: eosinophilic granuloma (monostotic and polyostotic), Hand-Schuller-Christian, and Letterer-Siwe disease. The first two types (EG and HSC) are less aggressive and are chronic in clinical behavior while the last (LS) is more aggressive and acute in behavior. Today, a more prevalent classification system characterizes LCH cases into unifocal, multifocal/unisystem, and multifocal/multisystem types. This classification also divides patients into low- and high-risk categories. Patients with the unifocal and multifocal/unisystem types are considered low risk, while multifocal/multisystem-type patients are considered high risk. If the disease affects one organ, be it in one site or multiple sites of one organ (i.e. bone, lymph nodes, skin), it is considered to be of the low-risk type. If the disease involves multiple organs such as the lungs, liver, spleen and bone marrow (multifocal and multisystem), it is considered to be of the high-risk type. Langerhans cells are CD1a positive; for that reason, immunohistochemistry staining is very helpful. They are also S-100 and CD45 positive. Langerhans cells can also be comfortably identified by the H & E stain.
In the oral cavity, the typical presentation of LCH is in the form of a lytic lesion in the posterior mandible, usually with pain and swelling, though it can also be asymptomatic. The bony lesions are usually aggressively lytic, especially those of the mandible. As mentioned above, this disease rarely occurs in adults. More than 50% of cases affect children under 10 years of age, with a male predilection.
Oral soft tissue involvement with LCH is very rare, especially in such an old patient. Up to 50% of patients, especially the elderly population, first present with skin lesions which progress to systemic involvement. Skin lesions range from seborrheic dermatitis-like lesions to papules and nodules. In the mouth and genitalia, ulcers are described. In rare cases, LCH is associated with hemopoietic malignancy such as acute leukemia or malignant lymphoma. This patient developed acute leukemia.
Treatment includes curettage, especially of the jaw lesions. Chemotherapy and low-level radiotherapy have also been effective. The unifocal disease has an overall 95% survival rate. Cases with two-organ involvement have a 75% overall survival rate. The prognosis becomes progressively worse as more organs are involved.
References
- Schlosser BJ. Lichen planus and lichenoid reactions of the oral mucosa. Dermatol Ther. 2010 May-Jun;23(3):251-67.
- Chiappelli F, Kung MA et al. Cellular immune correlates of clinical severity in oral lichen planus: preliminary association with mood states. Oral Dis. 1997; 3:64-70.
- Crincoli V, Di Bisceglie MB, Scivetti M, Lucchese A, Tecco S, Festa F. Oral lichen planus: update on etiopathogenesis, diagnosis and treatment. Immunopharmacol Immunotoxicol. 2011 Mar;33(1):11-20.
- Cheng S, Kirtschig G, Cooper S, Thornhill M, Leonardi-Bee J, Murphy R. Interventions for erosive lichen planus affecting mucosal sites. Cochrane Database Syst Rev. 2012 Feb 15;2:CD008092.
- Kohli PS, Kaur J. Erythema Multiforme-Oral Variant: Case Report and Review of Literature. Indian J Otolaryngol Head Neck Surg. 2011 Jul;63(Suppl 1):9-12.
- Joseph TI, Vargheese G, George D, Sathyan P. Drug induced oral erythema multiforme: A rare and less recognized variant of erythema multiforme. J Oral Maxillofac Pathol. 2012 Jan;16(1):145-8.
- Brown RS, Farquharson AA, Morton I, Tyler MT. Oral erythema multiforme major: a triple case report. Gen Dent. 2011 Jul-Aug;59(4):302-8.
- Chan LS et al.: The first international consensus on mucous membrane pemphigoid: definition, diagnostic criteria, pathogenic factors, medical treatment, and prognostic indicators. Arch.Dermatol 2002; 138 (3):370-379.
- Eschle-Meniconi ME Mucous membrane pemphigoid: an update. Curr Opin Ophthalmol. 2005 Oct;16(5):303-307.
- Bagan J, Mucosal disease series. Number III. Mucous membrane pemphigoid. Oral Dis. 2005 Jul;11(4):197-218.
- Wang X, Yang S, Tu P, Li R. A case of Langerhans cell histiocytosis in an adult with initial symptoms confined to the skin. Int J Dermatol. 2010 Mar;49(3):337-9.
- Wang P, Wang X, Hong J, Wang Z. Extensive cutaneous Langerhans cell histiocytosis in an elderly woman. J Dermatol. 2011 Aug;38(8):794-7.
- Baumgartner I, von Hochstetter A, Baumert B et al. Langerhans cell histiocytosis in adults. Med Pediatr Oncol 1997; 28: 9–14.
- Malpas JS, Norton AJ. Langerhans cell histiocytosis in the adult. Med Ped Oncol 1996; 27: 540–6.