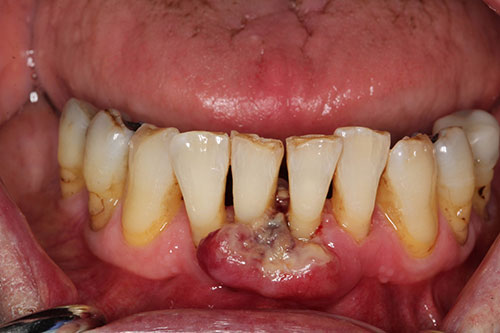
Ulcerated gingival swelling between teeth #s 24 & 25
Can you make the correct diagnosis?
This is an 85-year-old male who presented with an ulcerated gingival swelling between teeth #s 24 & 25 of three weeks duration.
Sorry, you are incorrect!
This exophytic, ulcerated reddish, sessile and firm gingival lesion of three weeks duration should make one think of reactive gingival swellings that include pyogenic granuloma (PG), peripheral giant cell granuloma (PGCG) and peripheral ossifying fibroma (POF). Reactive gingival swellings usually respond to local stimuli such as excessive plaque, calculus, open margins and others.
Pyogenic granuloma (PG) is the most common reactive gingival swelling. The surface ulceration and red purplish color is typical of PG and therefore considered as a potential diagnosis in this case. Pyogenic granulomas tend to be vascular and red in color and are usually ulcerated all clinical features consistent with this case. For the same reason, PGCG would be considered. They usually present as red, gray, or purplish in color. However, the age and gender is not consistent with either of the two reactive gingival swelling since both occur in young females. The site is also not consistent since anterior mandible or maxilla are not typical site for PG or PGCG but are more likely sites for peripheral ossifying fibroma (POF). The color however is not consistent with POF since they are usually pink. The age and gender are also not consistent since POFs tend to occur more commonly in females between 10-20 years of age. The histology in this case is not consistent with PG, PGCG or POF.
Sorry, you are incorrect!
The age and gender combined with ulcerated, red and fast growing gingival lesion should make one think of primary malignancy such is squamous cell carcinoma (SCC) of the gingiva. Gingiva is the third most common site for oral SCC in chronic tobacco users but there is no history of chronic tobacco use in this patient. The histology was not supportive of gingival squamous cell carcinoma.
Squamous cell carcinoma (SCC) of the gingiva is uncommon, especially in a non-smoker. Gingiva constitutes around 12% of oral SCCs. Oral SCC occurs predominantly in males over the age of 40 years, with an observed male-to-female ratio of 2:1 generally and 1.4:1 in the USA. Excluding the outer lip, the most common sites (in decreasing order) are ventral and lateral surfaces of tongue (25-50%), floor of mouth (15%), gingiva (12%) and palate (9%). The buccal mucosa and retromolar pad areas (3%) have a relatively low incidence of occurrence unless the patient is a chronic smokeless tobacco user. Oral SCC varies in presentation from deceptively innocent-looking to obviously malig¬nant. It may present as a non-healing ulcer, or as red, white or mixed red-and-white lesions. Characteristic signs of oral SCC are non-healing ulcer, ulcer with rolled borders, and fixation and induration. Oral SCC is most commonly associated with chemically induced mutagenesis, specifically tobacco and alcohol use. Determination of the prognosis of OSCC is based on its clinical stage using the TNM classification. The prognosis improves when the lesion is detected early.
Congratulations, you are correct!
The clinical presentation of fast growing ulcerated gingival swelling when combined with patient’s age and gender and past medical history of malignant mesothelioma, one has to include metastatic disease on the differential diagnosis. The histology was consistent with malignant mesothelioma metastatic to the gingiva.
Cancer metastasis to the oral cavity is neither specific nor common; such cases constitute less than 1% of all oral malignant neoplasms. They can be devastating to the patient because metastasis to other sites has already developed or is inevitable. Theoretically, any malignant neoplasm can metastasize to the oral cavity, but in actuality few do and of the ones that do, the majority is carcinomas. The most common malignant neoplasms that metastasize to the mouth are from the breast, lung, prostate and kidney. Malignant neoplasms from the colon, pancreas, esophagus, thyroid, cervix, and liver have also been described.
Breast cancer is the most common neoplasm to metastasize to the oral cavity altogether. Lung and prostate cancers are the most common neoplasms to metastasize to the oral cavity in men. In about 70% of cases, the oral presentation is a secondary diagnosis when the primary diagnosis of malignancy in a distant organ has been already made and the patient has had or is undergoing treatment for it. In about 30% of cases, the oral lesion is the first manifestation of the disease. By far the most common location is the posterior mandible, where 80% of cases occur, followed by the gingiva. This condition is mostly described in adults over the age of 30 and rarely in children.
Malignant pleural mesothelioma metastasizing to the gingiva is reported but is exceedingly rare. This is the first of such case for this author. Patient had clinical history of stage 4 malignant pleural mesothelioma.