Well Demarcated Mixed Radiolucent/Radiopaque Mass, Right Posterior Maxilla
Can you make the correct diagnosis?
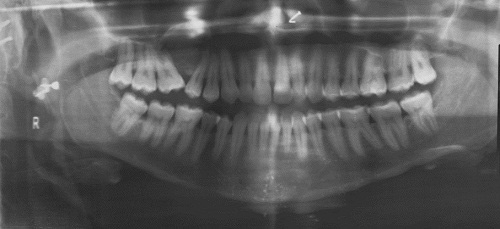
This is a 30-year-old female who self-referred for wisdom tooth removal. The oral surgeon noted a swelling in the right posterior maxilla of unknown duration which was confirmed by a panoramic radiograph.
Sorry! you are incorrect
The location, the buccal and palatal expansion and superior expansion into the maxillary sinus are all consistent with the behavior of fibrous dysplasia, so is the mixed radiolucent radiopaque radiographic morphology. The well-demarcated radiographic morphology however, is not and neither is the age of this patient. Fibrous dysplasia tends to be diffuse with periphery of the lesion blending in with the surrounding tissue. In addition, FD tends to occur at childhood and at puberty rather than in 30-years-old patients The histology however is not supportive of FD.
The etiology of fibrous dysplasia is unknown. The monostotic (one bone or bone complex area) form constitutes approximately 80% of all fibrous dysplasia cases while the polyostotic affects one or more bones with multiple lesions. FDs are expansile and disfiguring lesions, whether single or multiple. Monostotic FD, which involves the jaws, affects males and females equally. It occurs in childhood and at puberty and usually stops growing at age 30. It appears as an asymptomatic swelling of the maxilla or mandible; the maxillary lesion is the most common. It may involve bones other than the maxilla, including the zygoma, sphenoid and others. It is usually unilateral and is known to displace the teeth, but otherwise is firmly seated. The growth is usually slow, but rapid growth has been described, especially during puberty. The radiographic appearance, especially of the maxilla, is classically described as a ground glass appearance where fine radiopacity is noted. The mandibular lesions are much more deceptive because they tend to vary more, thus making diagnosis with a radiograph difficult. They range from cystic unilocular radiolucency to multilocular radiolucency to the classical ground glass radio-opacity. Surgery is indicated for functional and esthetic reasons. Radiation therapy is contraindicated since significant incidence of development of osteosarcoma in the irradiated FD has been documented. Malignancies such as osteosarcoma arising in an area of FD that has not been irradiated have been described, but rarely; these occur mainly in irradiated lesions.
Sorry! you are incorrect
The radiographic findings, the age, the location are all supportive of calcifying odontogenic cyst. The histology however is not.
Calcifying odontogenic cyst is not a common condition, accounting for only 1% of jaw cysts. This condition represents a spectrum of histologies including a simple cyst, a cyst with an odontoma, a cyst with ameloblastomatous proliferations and a more aggressive solid neoplasm, also known as “ghost cell odontogenic tumor,” with a potential to transform especially with multiple recurrences. It is therefore important to render a specific histological diagnosis. Calcifying odontogenic cyst is also described on the gingiva alone without a bony component in up to 20% of cases (peripheral COC). Intrabony COC presents as a well-circumscribed unilocular radiolucency with flecks or masses of radiopaque material. The size and amount of the radiopaque material varies depending on the type of cyst and whether or not it is associated with an odontoma. It can expand bone, displace and resorb teeth. In about one third of cases, COC is associated with unerupted teeth, usually the canine tooth. The most common locations are the anterior jaws in the incisor-canine area. It can occur at any age, but is most common in patients around 33 years of age; however, the odontoma-associated COCs tend to occur in younger females around the age of 17. This cyst may also be associated with an odontoma, usually complex in type. The solid odontogenic ghost cell tumor is the least common, but behaves more aggressively than the others. These lesions are usually conservatively treated by thorough curettage and heal uneventfully. The solid type tends to recur and, for that reason, follow-up visits are recommended. With recurrence, a more aggressive treatment is recommended to prevent further recurrence.
Sorry! you are incorrect
The radiographic findings of mixed RL/RO, well-demarcated and expansile lesion, combined with the age and gender of the patient are supportive of central ossifying fibroma (COF). The location however is unusual for COF but good for juvenile ossifying fibroma. The histology is not supportive of COF.
Central ossifying fibroma is a benign neoplasm of bone origin. It presents as a well-demarcated to corticated radiolucent or mixed radiolucent/radiopaque mass with a peripheral radiolucent rim. Central ossifying fibroma is a slow-growing, expansile lesion with characteristic downward expansion of the inferior border of the mandible. It can also expand buccally and lingually. The associated teeth are vital. It is common in young adults around 35 years of age and is five times more likely to occur in females than males. It affects the posterior mandible in about 90% of cases.
Sorry! you are incorrect
The radiographic findings of mixed RL/RO, well-demarcated and expansile lesion, combined with the location is supportive of juvenile ossifying fibroma (JOF). The age of the patient, however is not. The histology is not supportive of JOF.
Juvenile ossifying fibroma (JOF) is a benign neoplasm of bone origin and is an aggressive variant of central ossifying fibroma of the jaws. It is by far more common in children under the age of 15. It is most common in the craniofacial bone, especially the maxilla. Two histologic variants are described, the trabecular and psammomatoid types. Trabecular JOF is histologically characterized by cellular connective tissue stroma interspersed with strands of trabeculae young bone with prominent osteoblastic rimming. Psammomatoid JOF is characterized by cellular connective tissue stroma with small and uniform cementum-like hard tissue resembling Psammoma bodies. Trabecular JOF occurs more commonly in the jaw bones; it is about twice as common in the maxilla as in the mandible. Psammomatoid JOF occurs more commonly in the paranasal sinuses (about 70% of cases) with 20% of cases occurring in the maxilla and 10% in the mandible. Trabecular JOF tends to occur in younger patients with a range of 8.5-12 years while psammomatoid JOF affects older children with a mean age of 20-22. Both types are slightly more common in males. Both types are benign but locally aggressive lesions simulating low-grade sarcoma behavior with a tendency for fast growth, invading the surrounding tissue and destroying bone. Both histological types have a high recurrence rate ranging from 30 to 56%. Treatment ranges from thorough curettage to resection to curettage with systemic subcutaneous interferon injections. The latter has been reported to be effective in inhibiting tumor growth and recurrence.
Congratulations! You are correct
Central odontogenic fibroma is a rare odontogenic neoplasm. Gardner presented a clarification of what should be considered central odontogenic fibroma since there was lack of clarity. He classified this neoplasm into 2 types: Simple and WHO types. In the past, some pathologists were diagnosing hyperplastic dental follicles as central odontogenic fibromas and for that reason this lesion was considered to be common at some point. It is of mesenchymal origin. It occurs most frequently in children and young females. The female-to-male ratio is 7:1 in some reports. It occurs most often in the maxilla anterior to first molar tooth. There are other reports that describe them to be more common in the posterior mandible. It presents with swelling and can resorb and displace teeth. It is otherwise, asymptomatic. It can present as a unilocular or multilocular expansile radiolucency or mixed radiolucent/radiopaque lesion. Simple surgical excision is the treatment of choice. It has a good prognosis. This lesion may recur and has been described to transform to odontogenic fibrosarcoma.
References
- Gorlin RJ, Pindborg JJ et al. The calcifying odontogenic cyst–a possible analogue of the cutaneous calcifying epithelioma of Malherbe. An analysis of fifteen cases. Oral Surg Oral Med Oral Pathol. 1962;15:1235-1243.
- Moleri AB, Moreira LC et al. Comparative morphology of 7 new cases of calcifying odontogenic cysts. J Oral Maxillofac Surg. 2002;60:689-696.
- Su L, Weathers DR, et al. Distinguishing features of focal cemento-osseous dysplasia and cemento-ossifying fibromas: II. A clinical and radiologic spectrum of 316 cases. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 1997 Nov; 84: 540-549.
- Chang CC, Hung HY, Chang JY, Yu CH, Wang YP, Liu BY, Chiang CP. Central ossifying fibroma: a clinicopathologic study of 28 cases. J Formos Med Assoc. 2008 Apr;107(4):288-94.
- Williams HK, Mangham C, Speight PM. Juvenile ossifying fibroma. An analysis of eight cases and a comparison with other fibro-osseous lesions. J Oral Pathol Med. 2000;29:13–18.
- Eversole LR, Leider AS, Nelson K. Ossifying fibroma. A clinicopathologic study of sixty-four cases. Oral Surg Oral Med Oral Pathol. 1985;60:505–511.
- Samir El Mofty Psammomatoid and trabecular juvenile Ossifying Fibroma of the craniofacial skeleton: Two distinct Clinicopathological entities. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2002; 93:296-304.
- Johnson LC, Yousefi M, Vinh TN, Heffner DK, Hymans VJ and Hartman KS. Juvenile active ossifying fibroma, its Nature, Dynamics and Origin Acta Otolaryngol 1991; suppl 1 488: 1-40.
- Neville B, et al. Textbook of oral and maxillofacial pathology. Central odontogenic fibroma. Pages 726-727. Third edition, 2009.