Return to Case of the Month Archives
Slightly exophytic yellowish lesion lateral tongue
Dolphine Oda, BDS, MSc
doda@u.washington.edu
Contributed by
Dr. Ed Truelove, Dr. Thomas Morton, Ms. Negin Bardideh
Department Oral Medicine, University of Washington
Case Summary and Diagnostic Information
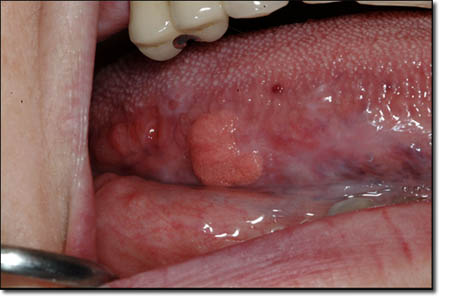
This is a 63-year-old white female who presented with a slightly exophytic, orange-yellow and well demarcated lesion on the right posterior and lateral border of tongue (Fig 1). It was about 1 x 1 cm in size, of one year’s duration and asymptomatic. The surface of this lesion was slightly corrugated to verrucoid in configuration. The patient has a history of lichen planus on the bilateral buccal mucosa (Fig 3), mandibular (Fig 2) and maxillary vestibule, alveolar ridge and lateral tongue (Fig 1). The patient has no history of alcohol or tobacco use. The lesion is asymptomatic but the patient complains of chronic and generalized oral burning sensation interpreted to be due to her chronic lichen planus.
Diagnostic Information Available
This is a 63-year-old white female who presented with a slightly exophytic, orange-yellow and well demarcated lesion on the right posterior and lateral border of tongue (Fig 1). It was about 1 x 1 cm in size, of one year’s duration and asymptomatic. The surface of this lesion was slightly corrugated to verrucoid in configuration. The patient has a history of lichen planus on the bilateral buccal mucosa (Fig 3), mandibular (Fig 2) and maxillary vestibule, alveolar ridge and lateral tongue (Fig 1). The patient has no history of alcohol or tobacco use. The lesion is asymptomatic but the patient complains of chronic and generalized oral burning sensation interpreted to be due to her chronic lichen planus.

The patient has type 2 diabetes controlled with medications, including daily insulin injections. The patient is otherwise in good general health.
Physical examination revealed an expansile lesion in the anterior mandible between teeth #s 22 and 28 (Fig 1). Panoramic radiographs showed a large, expansile, well demarcated to corticated unilocular radiolucency (Fig 1). This lesion recurred in 1992 after thorough curettage of the area. The first recurrence (Fig 2) was small and well demarcated between teeth #s 28 and 29, but less well defined in area of missing teeth #s 26-27. This lesion was also thoroughly curetted and several teeth were extracted (teeth #s 22-24 and 28-30). The second recurrence (Fig 3) took place in 2005, 13 years after the first recurrence. It was mostly in the anterior mandible and was a well demarcated to corticated unilocular radiolucency. It was also slightly expansile.

Figure 1. Verruciform xanthoma of the lateral posterior surface of tongue at the primary clinical presentation. Note the yellowish-orangey color with warty surface appearance. These are characteristic features of this lesion.
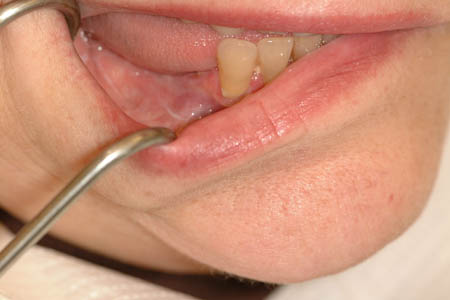
Figure 2. Lichen planus of the mandibular vestibule extending to the alveolar ridge. Note the white interlacing striae of Wickham typical of lichen planus.
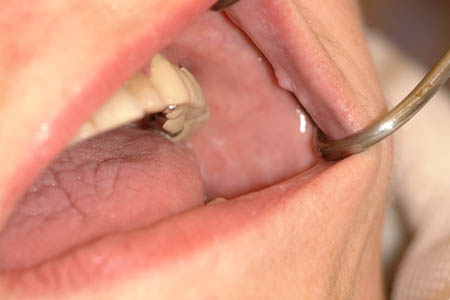
Figure 3. Lichen planus of the buccal mucosa (bilateral). Note the white interlacing striae of Wickham typical of lichen planus.
The incisional biopsy was read by Dr. Thomas Morton from the Oral Pathology Biopsy Service, University of Washington. The H & E stained glass slide revealed a hyperplastic and papillary surface epithelium with clefts filled with keratin (Figs 5). The papillary projections were slightly above the surface with parakeratin spikes. They were supported by connective tissue papillae containing sheets of xanthoma cells (Fig 6). These cells were mostly within the connective tissue papillae.
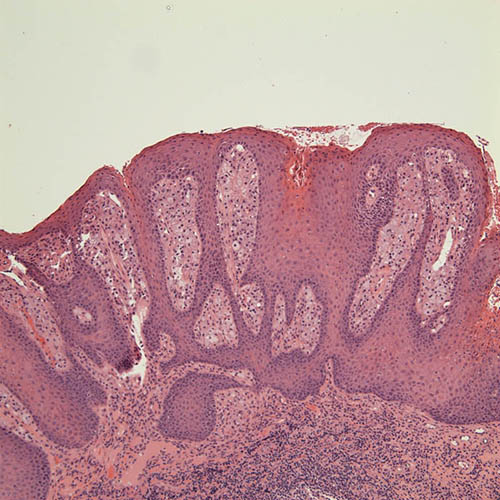
Figure 5. Low power (x100) histology shows papillary lesion with uniformly elongated rete pegs and papillary connective tissue with sheets of xanthoma cells.
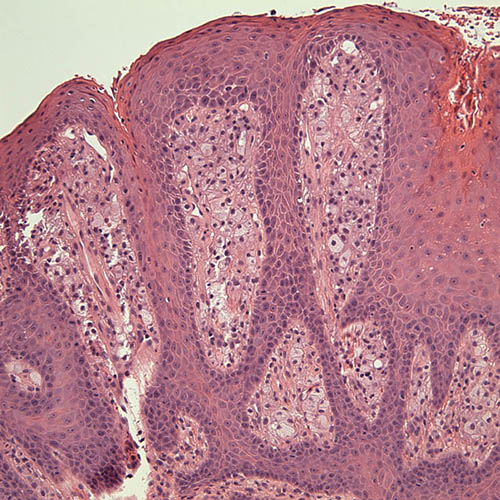
Figure 6. High power (x200) histology shows closer look of the papillary connective tissue with sheets of xanthoma cells.
After you have finished reviewing the available diagnostic information