Generalize ulcerative gingiva and oral mucosa
Dolphine Oda, BDS, MSc
doda@u.washington.edu
Can you make the correct diagnosis?
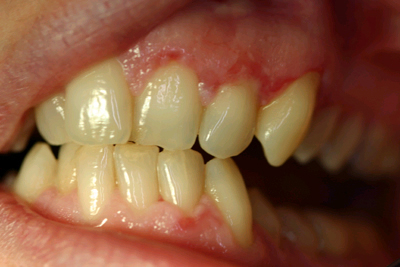
This is a 39-year-old white female who first noticed a few nonhealing oral ulcers that started at the end of 2004.
Sorry! you are incorrect
Mucous membrane pemphigoid is the preferred name for the overall disease process (1). Given the gender, comparatively young age, and the location of the first lesions, mucous membrane pemphigoid should be seriously considered as a likely diagnosis. It usually affects females (2:1 F:M ratio) around 50-60 years of age (1-5).
Like many of the vesiculobullous diseases, MMP is a chronic autoimmune disease predominantly affecting mucosa. The oral mucous membrane, specifically the gingiva, is more commonly affected (1, 5). The immune system recognizes multiple antigens in the region around the basement membrane as foreign, forming a complex attracting inflammatory cells which leads to a separation of the surface epithelium from the connective tissue (1-4). As opposed to eye and nose lesions, which tend to heal with scarring, oral lesions may heal without scarring (2-4). The oral cavity tends to be the first site of the disease target (it occurs twice as often on the gingiva as “desquamative gingivitis” than anywhere else) (3-4) followed by the eyes (which can cause blindness through scarring), nose, nasopharynx, genitalia, skin, larynx and esophagus. Patients with MMP may have circulating antibodies.
In the oral cavity, it presents as red gingival patches with loss of stippling. There may be sloughing and desquamation of the epithelium, especially as a result of mechanical pressure such as from brushing and denture irritation. If not treated, it may extend to the palate, tongue, buccal mucosa and other areas in the mouth (1-5). It shows a positive Nikolsky sign. About 12-25% or more of the MMP cases involve the eyes (5). Histopathology: Sub-basilar split (with an intact basal cell layer as part of the detached epithelium) of the intact surface epithelium from the underlying fibrous connective tissue. Many inflammatory cells, including eosinophils, are present. immunofluorescent studies are useful in rendering a definitive diagnosis. MMP is usually positive with IgG and C3 antibodies present in form of uniform line along the basement membrane. The best biopsy site to rule out MMP is a perilesional area rather than the sloughing and detached area. Treatment includes local and systemic steroids and immune suppressants, depending on the severity of the disease. Antibiotics for secondary infections are also prescribed. The histology and IMF studies of this case were not supportive of MMP.
Congratulations! You are correct
Pemphigus vulgaris is the most common lesion of the pemphigus family (1, 6-10); there are various other pemphigus subtypes including vegetans, foliaceus erythematosus, and paraneoplastic. This condition is less common in the mouth than lichen planus (3, 9). It is an autoimmune disease that causes desquamation of the oral mucosa and skin. The antibody targets intercellular desmosomal adhesion molecules called desmogleins, which results in the breakdown of the middle part of the spinous layer, leaving the basement membrane intact. This is histologically referred to as acantholysis and suprabasilar separation (1, 6-10).
Pemphigus vulgaris is a serious and life-threatening disease and can kill the patient if not treated; it has a mortality rate of 60-90% in non-treated patients, compared to 5% in the treated patients (1, 6-10). Complications from steroid treatment and infection can be fatal. Patients with pemphigus vulgaris also develop circulating antibodies; the antibody titer in this disease may be related to the severity of the local disease. Drugs such as penicillamine can induce PV, and neoplasms such as leukemia and lymphoma can induce paraneoplastic pemphigus. Several proteins are targeted in paraneoplastic pemphigus (1, 3, 9).
This disease has a high prevalence in patients of Jewish and Mediterranean origin, such as, Greeks, and Italians. Females are affected more commonly than males (2:1 F:M ratio). It occurs more often in patients ages 40 to 60, and rarely occurs in children (6-10). Oral lesions are usually the first to occur, as is the case in this patient. In the mouth, the soft palate and buccal mucosa are common sites for PV, but it can also affect the gingiva and lateral tongue mainly because of trauma from brushing and chewing on the lateral tongue. The erosions and sloughing epithelium is painful especially with hot drinks, alcoholic beverages and spicy and acidic food. These patients have difficulty brushing their teeth. PV affects other mucosae including the nasopharynx, anogenital and esophagus (1, 10). Skin lesions frequently present with vesicles and bullae that easily rupture forming ulcers. Nikolsky sign is positive.
Histopathology, this condition presents with supra-basilar clefting, leading to splitting of the epithelium above the basal cell layer and blister formation. This is the result of acantholysis in the middle spinous layer epithelial cells, releasing cells within the cleft known as Tzanck cells. Immunofluorescent (IMF) studies (both direct and indirect) can be useful (6-10). The epithelial cells in the spinous layer are positive with IgG and C3 complement forming a fishnet pattern around the epithelial cells. Treatment includes systemic steroids and local steroids as well as immune suppressant-type medications dependent on the severity of the disease.
Treatment
With a diagnosis of pemphigus vulgaris, the patient was started on steroid treatment with prednisone taper starting with 60 mg a day for three weeks; the dose eventually tapered to 30 mg a day. She was also started on Imuran on June 21 at 100 mg a day. Currently, she is on 40 mg of prednisone every other day, t.i.d. decadron swish and expectorate, and a low dose of azathioprine. Dr. Fleckman plans to taper her dose of prednisone and increase the azathioprine. She reports that her oral lesions have cleared since she began taking these medications. She also reports increased tearing but no overt conjunctivitis.
References
- Chan LS et al.: The first international consensus on mucous membrane pemphigoid: definition, diagnostic criteria, pathogenic factors, medical treatment, and prognostic indicators. Arch.Dermatol 2002; 138 (3):370-379.
- Eschle-Meniconi ME Mucous membrane pemphigoid: an update. Curr Opin Ophthalmol. 2005 Oct;16(5):303-307.
- Bagan J, Mucosal disease series. Number III. Mucous membrane pemphigoid. Oral Dis. 2005 Jul;11(4):197-218.
- Burgess JA et al. Pharmacological management of recurrent oral mucosal ulceration. Drugs. 1990 Jan;39(1):54-65.
- Weedon D. Skin Pathology. 2001. Churchil Livingstone. Pages 141-142.
- Camacho-Alonso F Pemphigus vulgaris. A presentation of 14 cases and review of the literature. Med Oral Patol Oral Cir Bucal. 2005 Aug-Oct;10(4):282-8.
- Bystryn JC and Rudolph JL. Pemphigus. Lancet 366 (9479):61-73, 2005
- Jonkman MF et al. Loss of desmoplakin tail causes lethal acantholytic epidermolysis bullosa. Am J Hum Genet. 2005 Oct;77(4):653-60. Epub 2005 Aug 17
- Scully C. Mucosal diseases series. Oral Dis. 2005 Mar;11(2):57.
- Ettlin DA. Pemphigus. Dent Clin North Am. 2005 Jan;49(1):107-25
- O’Regan E Linear IgA disease presenting as desquamative gingivitis: a pattern poorly recognized in medicine. Arch Otolaryngol Head Neck Surg. 2004 Apr;130(4):469-72.
- Eguia del Valle A Oral manifestations caused by the linear IgA disease. Med Oral. 2004 Jan-Feb;9(1):39-44.
- Cohen DM Linear IgA disease histopathologically and clinically masquerading as lichen planus. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1999 Aug;88(2):196-201.
- Stoopler ET Oral herpetic infections (HSV 1-8). Dent Clin North Am. 2005 49(1):15-29
- Stoopler ET Herpes viruses. Gen Dent. 2003 May-Jun;51(3):281-6.
- Birek C.Herpesvirus-induced diseases: J Calif Dent Assoc. 2000 Dec;28(12):911-21
Sorry! you are incorrect
For details on erosive lichen planus (LP) and the clinical presentation and behavior of LP, including erosive LP and lichenoid drug reaction, please read E-PIE, Spring 2004 issue under Clinical Case Discussion. Neither the clinical presentation nor the histology or the immunofluorescent studies in this case are supportive of LP or lichenoid drug reaction.
Sorry! you are incorrect
The clinical presentation of progressive ulceration over a six-month period is very unusual in primary herpes of the mouth, as is the age of the patient. Primary herpetic gingivostomatitis affects children and young adults (14-16). More than 80% of cases are subclinical. It affects up to 60% of the population in countries with a high average socioeconomic status such as the U.S., while it can affect virtually the entire population of developing countries. Clinically, these patients present with fever, irritability, headache, pain upon swallowing, and extremely inflamed mucosa, including the lips, gingiva, tongue, buccal mucosa, palate, pharynx, and tonsils. Lymphadenopathy is also frequently present (14-16). The lesions are usually in form of small vesicles that rupture to form shallow, ragged painful ulcers. They heal in 10-14 days after which the virus travels along the nerve to remain latent in the ganglion supplying the area. HSV-1 usually harbors the trigeminal ganglion while HSV-2 harbors the lumbosacral ganglion. Stimuli such as immunodeficiency will release the virus and initiate secondary lesions. Patients can also develop complications such as pneumonia and meningitis. Histology, if available, is distinct and diagnostic for herpetic changes but will not distinguish between Herpes 1, 2, or varicella-zoster. Treatment ranges from supportive to systemic acyclovir.
Sorry! you are incorrect
This is a rare subepidermal blistering disease with two clinical variants: chronic bullous dermatosis of childhood (formerly known as juvenile dermatitis herpetiformis) and adult linear IgA bullous dermatosis (11-13). These lesions have a linear deposition of IgA antibody at the basement membrane. The antigen targeted is in the lamina lucida, hence the name derivation. The childhood type affects children under ten years of age while the adult type affects adult females more commonly (2:1 F:M ratio) and is considered a type of mucous membrane pemphigoid (11-13). 80% of adult cases involve the mucosa, eyes, mouth and genitalia, with extensive scarring (11-13). In about 33% of cases, the adult patients are gluten sensitive. Incidence may follow the use of a number of medications including captopril, somatostatin, lithium, phenytoin and NSAIDS. These lesions respond to Dapsone with low-dose systemic steroids.