Unilocular expansile radiolucency, right posterior mandible
Can you make the correct diagnosis?
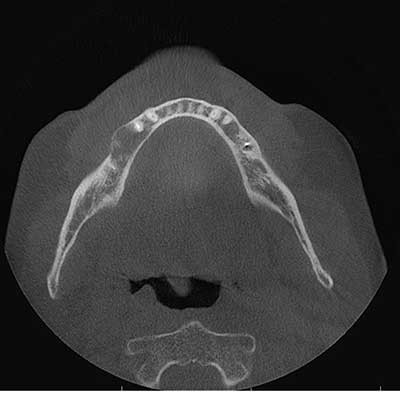
This is a 64-year-old male who presented to a periodontal office for evaluation of a right mandibular edentulous bicuspid area for implant placement.
Differential Diagnosis
- Odontogenic cysts
a. Residual periapical cyst
b. Glandular odontogenic cyst (GOC)
c. Odontogenic Keratocyst (OKC) - Odontogenic tumors
a. Ameloblastoma
b. Odontogenic Myxoma
c. Central odontogenic fibroma - Central giant cell granuloma (CGCG)
- Central odontogenic fibroma & CGCG-like lesion
Sorry, you are incorrect!
A well-demarcated and unilocular radiolucency in the jaws should make one think of cysts especially odontogenic cysts which are the most common conditions fitting this radiographic presentation. In this case, since the radiolucency is in an area of an extracted tooth, residual periapical cyst should be placed high on the differential diagnosis. Residual periapical cysts are usually asymptomatic but can be expansile and painful if inflamed, and can occur in patients of any age or gender.
Another odontogenic cyst to consider is odontogenic keratocyst (OKC). The posterior mandible is a common site for OKC. The age of this patient is slightly on the older side of the typical age range, but OKCs can occur at any age. The expansion, however, is not consistent with the behavior of most OKCs, especially given the relatively small size.
Glandular odontogenic cyst (GOC) is another cyst to consider. The expansion as well as the patient’s age and gender are consistent with GOC. The site, however, is unusual for GOCs since they tend to occur more often in the anterior mandible or in association with third molars in the posterior mandible.
The histology in this case, however, is not consistent with any of these three cysts.
Sorry, you are incorrect!
Several odontogenic neoplasms can present as expansile unilocular radiolucencies in the posterior mandible, including unicystic ameloblastoma, odontogenic myxoma, and central odontogenic fibroma.
For this age range, solid ameloblastoma is the more likely type of ameloblastoma to consider first. However, solid ameloblastomas usually present as multilocular and highly expansile radiolucencies. This lesion is therefore unlikely to be solid ameloblastoma.
Unicystic ameloblastoma presents as a unilocular radiolucency in the posterior mandible; 90% of time associated with an impacted third molar tooth simulating a dentigerous cyst. It is highly unlikely that this radiographic presentation would be that of unicystic ameloblastoma. Furthermore, the typical age range of patients with unicystic ameloblastoma is 10-20 years, much younger than that of this patient’s age. This case is therefore unlikely to be unicystic ameloblastoma.
Odontogenic myxoma is another odontogenic neoplasm that occurs more commonly in the posterior mandible. It is usually multilocular and expansile but can be unilocular and expansile. The age range of patients with odontogenic myxoma is around 23-30 years with a slight predilection for occurrence in females (1:1.5 male-to-female ratio). In this case, the site and radiographic findings are suggestive of odontogenic myxoma, while the age and gender are not.
Central odontogenic fibroma (COF) is another odontogenic neoplasm to consider. It occurs in a wide age range, 5-82, with a mean of 42 years of age at occurrence. COF tends to occur more commonly in the maxilla anterior to the first molar; its second most common site is in the mandible posterior to the first molar. It tends to be more common in females. It usually presents as an expansile unilocular or multilocular expansile radiolucent or mixed radiolucent and radiopaque lesion. It can be unilocular or multilocular. The age, gender and site (anterior to the first molar) in this case are not consistent with COF.
The histology in this case is not consistent with ameloblastoma and odontogenic myxoma. The histology has some components of COF with prominent epithelial component.
Sorry, you are incorrect!
Central Giant Cell Granuloma (CGCG) is described as a non-neoplastic condition that can behave like a neoplastic process in its ability to destroy bone and displace teeth. Over 60% of CGCG cases occur in patients younger than 30 years of age, with twice as many occurrences in females as in males. They occur more commonly in the mandible anterior to the first molar teeth. It can grow towards anterior mandible crossing the midline. Radiographically, they are usually multilocular and expansile but can be unilocular and expansile. The site and the radiographic findings are consistent with CGCG, but not the patient’s age and gender. The histology of this case has a component with CGCG-like features.
Congratulations, you are correct!
The histology in this case is that of a combined central odontogenic fibroma with a prominent epithelial component associated with a central giant cell granuloma-like lesion. To date, at least 30 such cases are described in the literature. Many others, like this case and a handful of other such cases from the Oral Pathology Biopsy Service at University of Washington, School of Dentistry, are diagnosed but not reported for lack of understanding of this condition’s pathogenesis and clinical significance.
Because this condition is of unknown pathogenesis, there is no clear consensus regarding what to call it. A variety of names exist in the literature, including “hybrid” tumor, “collision” tumor, CGCG-like reaction to central odontogenic fibroma, COF-like reaction to central giant cell lesion, and others. Each author makes a case for their interpretation without much tangible evidence; nonetheless, they often offer convincing interpretations of their understanding of the cellular behavior.
There are enough cases reported to state that these lesions are more common in the mandible, particularly in the premolar/molar area. They have been described in a wide age range of 5-73 years of age with a predilection to the first three decades of life. They have a predilection for occurrence in females as demonstrated in several reports except in two case series where males were more predominant. Radiographically, they are unilocular or multilocular and expansile radiolucencies that may perforate bone. Recurrence has been described; one report describes recurrence in two out of eight cases. In this patient, the site of and radiographic findings are consistent with this condition. The patient’s age is on the older range but still within the reported age range and gender was not consistent with the most reported cases.