Red, slightly raised nodule, dorsal surface of tongue.
Can you make the correct diagnosis?
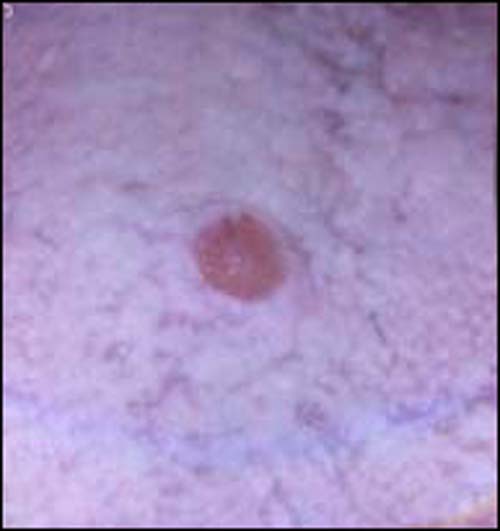
This is an 18-year-old male who was referred to Dr. Jackson for the extraction of his third molar teeth. He was seen initially on December 19, 2005, when he complained of soreness to his third molars. Extra-oral examination was unremarkable. Intra-oral examination revealed no signs or symptoms of an acute infection, but revealed a lesion of unknown duration on the mid-dorsal tongue.
Congratulations! You are correct
Osseous and cartilaginous choristomas are defined as exophytic nodules of normal tissue (bone or cartilage) occurring in an abnormal area where neither of the two hard tissues typically grow. They present as smooth-surfaced nodules with a particular predilection for the posterior tongue (1-2), near the foramen cecum in at least 67% of cases; 25% of cases are in the lateral tongue, and 7.5% are in the middle tongue as is the case with our patient (2). It can also present in the buccal mucosa, lips and submandibular area (4). It occurs more commonly in females and in adults around 30 years of age, with an age range of 12-64 (1-3). These lesions are benign and self-limiting. Their sizes range from a few millimeters to 5 cm, with an average of one centimeter (1-3). They are slow-growing and may be present for a long duration ranging from months to years (1-3). They are usually asymptomatic, and are smooth-surfaced with a hard consistency. When located in the posterior tongue, they may cause nausea, dysphagia and irritation (2). Histologically, the lesions are made up of a nodule of bone or cartilage depending on the type. The bony nodules are usually lamellar in type with focal areas of less mature bone. Conservative surgical excision is the treatment of choice. After excision, the area usually heals well; recurrence is rare.
Treatment
Under general anesthesia, all four molar teeth were extracted and the mid-dorsal tongue lesion was excised. The tissue surrounding the tongue lesion was undermined and closed with 3-0 silk sutures. After one week, the patient reported back for a follow up check and suture removal; at this time he was healing well with no complaints. At a six week follow-up, his tongue was well healed with no evidence of a residual lesion or abnormality. He was to return in three to four months for a soft tissue check up.
References
- Lin CC, Chen CH, Chen YK, Shen YH, Lin LM. Osseous choristoma of oral cavity–report of two cases and review of the literature. Kaohsiung J Med Sci. 1998 Nov;14(11):727-33
- Vered M, Lustig JP, Buchner A. Lingual osteoma: a debatable entity. J Oral Maxillofac Surg. 1998 Jan;56(1):9-13.
- Gaitan-Cepeda LA, Quezada-Rivera D, Ruiz-Rodriguez R. Osseous choristoma of the oral soft tissue. Case report. Med Oral. 2003 May-Jul;8(3):220-3.
- Johann AC, Garcia BG, Nacif TR, de Freitas JB, do Carmo MA, Mesquita RA. Submandibular osseous choristoma. J Craniomaxillofac Surg. 2006 Jan;34(1):57-9. Epub 2005 Dec 15.
- Poveda R. Granular cell tumour. Med Oral. 2004 Aug-Oct;9(4):362.
- Giuliani M, Lajolo C, Pagnoni M, Boari A, Zannoni GF. Granular cell tumor of the tongue (Abrikossoff’s tumor). A case report and review of the literature. Minerva Stomatol. 2004 Jul-Aug;53(7-8):465-9.
- Carinci F, Piattelli A, Rubini C, Fioroni M, Stabellini G et al. Genetic profiling of granular cell myoblastoma. J Craniofac Surg. 2004 Sep;15(5):824-34.
- Bae GY, Choi HJ, Chang SE, Lee MW, Sung KJ, Koh JK. A case of median rhomboid glossitis. J Dermatol. 2003 May;30(5):423-5.
- Pindborg JJ. Revival of “median rhomboid glossitis”? Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1995 Jul;80(1):2-3.
- Dayan D, Bodner L, Hammel I, Wolman M. Histochemical characterization of collagen fibers in fibrous overgrowth (irritation fibroma) of the oral mucosa: effect of age and duration of lesion. Arch Gerontol Geriatr. 1994 Jan-Feb;18(1):53-7.
- Walinski CJ. Irritation fibroma removal: a comparison of two laser wavelengths. Gen Dent. 2004 May-Jun;52(3):236-8.
- Esmeili T, Lozada-Nur F, Epstein J. Common benign oral soft tissue masses. Dent Clin North Am. 2005 Jan;49(1):223-40
Sorry! you are incorrect
This is a benign neoplasm of uncertain histogenesis first described by Abrikossoff in 1926 (6). It has been called by a number of names, including myoblastoma, a name which implies muscle origin (6-7). This implication is based on the H & E histology in about 70% of cases in which the granular cells are closely associated with the skeletal muscle fibers (5-7). A small percentage of these tumors are also found in close association with nerve fibers, implying their origin from the neural crest. The immunohistochemistry markers support the origin of this tumor from the neural crest and not from muscle, hence the name change to granular cell tumor (7).
The tongue is the most common site of occurrence of this tumor; almost one third of cases occur in the tongue (5-7). The skin is another common site, but this lesion is known to occur in a variety of sites and tends to be benign in most cases. A malignant form is described, but is rare.
In the mouth, the buccal mucosa is second to the tongue in site predilection, and the lesion is more common in females than males (2:1 ratio). It tends to occur in adults over 30 years of age but it has also been described in children with an average age 14.5 and a range of 3-19 (5-6). It is usually asymptomatic and can be of a long-term duration ranging from months to years. The dorsal-lateral tongue is a common location and in about 80% of cases, it is superficial and submucosal (5-7). The color ranges from pink or white with a keratotic surface to yellow-orange. A newborn counterpart is described and is known as congenital epulis of the newborn; it is believed to be a separate entity with different cell origin (7).
Histologically, granular cell tumor is composed of strands and fascicles of large cells with distinct cell borders containing abundant granular cytoplasm. The nuclei are small and round to oval in shape, and are eccentrically located. These cells are at times intimately related to surrounding skeletal muscle fibers and at times to nerve. The lesion can be well demarcated and confined or infiltrative. The overlying epithelium can be normal in thickness or can show pseudoepitheliomatous hyperplasia (PEH) (6-7). The latter, when extensive in rare cases, can be mistaken for well differentiated squamous cell carcinoma, especially if the biopsy is superficial.
The tumor cells are positive with S-100 protein and neuron specific enolase (NSE) indicating a neural crest origin. Treatment includes conservative surgical excision. Recurrence is extremely rare. The clinical presentation of this case, especially the location, is supportive of GCT; however, the histology and the hard consistency are not.
Sorry! you are incorrect
MRG was first described by Brocq in 1914. It affects 1/1000 of the population in the US and is more common in adult males by nearly a 2:1 ratio (8-9). It presents in the middle and posterior dorsal surface of tongue. It can be flat or raised, and pink or red (8-9); the pink and red color is believed to be due to the atrophy of the filiform papillae. The lesion is usually asymptotic. This condition has varied etiologies; it was originally believed to be a developmental disease, but with time this theory has become less accepted (9). Today, it is thought to be a chronic and localized fungal infection. It is seen more often in denture wearers and in smokers (9). It tends to last for several years if not treated. Lesions that are present chronically tend to be raised, a characteristic consistent with hyperplastic candidiasis. Outdated literature suggests that this is a congenital and developmental disease caused by the failure of the tuberculum impar to retract. The lack of clinical evidence in support of this theory, i.e. the presence of this lesion in children, renders this theory unlikely.
Histologically, it is made up of surface epithelium with atrophied and thick spinous layer. It is usually covered with parakeratin that is superimposed with candidal hyphae. The connective tissue shows focal fibrosis and is usually mildly infiltrated by lymphocytes and plasma cells. This lesion can be persistent and the treatment usually involves eliminating the causative agents including treating for candidiasis, cessation of smoking and keeping the dentures clean. The clinical presentation of this case may be supportive of MRG, but the hard consistency and the histologic findings are not.
Sorry! you are incorrect
Fibroma is a mass of collagenous connective tissue which typically presents as an exophytic, dome-shaped, smooth surfaced, sessile or pedunculated nodule on the buccal mucosa (10). The most common etiology for a fibroma or fibrous hyperplasia is irritation, especially from chronic chewing of the area. Occasionally, it may represent a true benign neoplasm of fibrous connective tissue origin. It can affect patients of any age, but it is more common in adults around 30 years of age with no sex predilection (10). It occurs anywhere in the oral cavity, but most commonly on the buccal mucosa along the plane of the occlusal line, lips, lateral tongue and gingiva. Dorsal surface of tongue is an unusual location for a fibroma, but it occasionally occurs as a result of acute trauma such as a sharp bite (10). It can be pink, white or red (if ulcerated) in color (10-12). In individuals with dark skin, it can be grey or brown. Sizes range from a few millimeters to several centimeters in diameter, averaging 1-2 cm. Unless they are ulcerated, fibromas are usually asymptomatic.
Histologically, the lesion is made up of a nodule of connective tissue, usually collagenous. The surface epithelium ranges from thin to thick and is usually covered by parakeratin or orthokeratin. Conservative surgical removal, whether conventional or laser, and cessation of the chewing habit qualify as appropriate treatment (10-11). The likelihood of recurrence depends on whether the habit of cheek chewing continues. The clinical presentation of dorsal tongue is an unusual location for a fibroma or fibrous hyperplasia but deep bites can include the dorsal tongue. Neither the histology nor the consistency of the lesion in this case are supportive of a fibroma/fibrous hyperplasia.