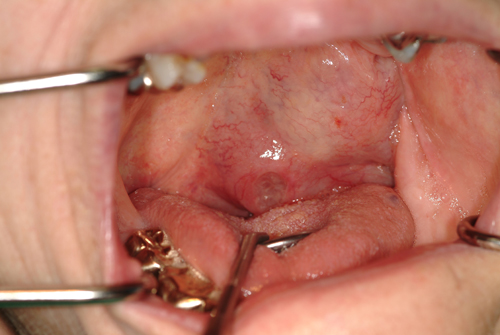
Large swelling, left soft palate and tonsillar area
Can you make the correct diagnosis?
This is an 88-year-old white female whose chief complaint was a progressively enlarging swelling of the left soft palate and tonsil. It was large, around 5 x 5 cm in size; pink-to-red in color; and focally ulcerated (Figure 1). She complained of pain and difficulty swallowing. The lesion is of six months’ duration.
Sorry! you are incorrect
Given the location, nasopharyngeal carcinoma should be considered on the differential diagnosis. However, given the gender, race and country of origin, it is unlikely that this is NPC. The histology is not supportive of NPC.
Nasopharyngeal carcinoma (NPC) is a malignant neoplasm of epithelium from the mucosa lining the nasopharyngeal area. World Health Organization classifies it into keratinizing, non-keratinizing and basaloid squamous cell carcinoma (1-4, 11). Lymphocytes constitute the second histological component of NPC but this is considered a secondary feature; therefore the old terminology of lymphoepithelioma is a misnomer. This neoplasm is rare in the United States but constitutes 18% of all malignancies in China, especially Southern China. In China, it is more common in males by a 3:1 ratio and is also more common in adults around 40-60 years of age (1-4, 11). Epstein Barr Virus plays a significant role in the etiology of NPC. In addition, diets high in nitrosamines, such as salted fish, have also been implicated, especially in Hong Kong boat dwellers who happen to have a higher incidence of NPC than Hong Kong house dwellers (11). Other risk factors include smoking and exposure to chemical fumes such as formaldehyde (11). Clinically, the lateral wall of the nasopharynx is the most common site of origin. One of the most common clinical presentations of NPC is cervical lymph node enlargement which is usually painless. Other aspects of the clinical presentation include soft palate swelling, nasal obstruction or nasal blood-tinged dripping, epistaxis, hearing loss and headaches (1-4, 11). Radiation therapy or combined radiotherapy and chemotherapy are the treatment of choice based of the stage of the disease. The five-year survival rate depends on the stage of the disease, gender and age of the patient. Younger patients, patients at an earlier stage, and females have a better prognosis than older males at a later clinical stage of the disease.
Sorry! you are incorrect
Given the location, the diffuse swelling and the soft consistency, a salivary gland neoplasm such as mucoepidermoid carcinoma should be included on the differential diagnosis. The histology, however, is not supportive of this diagnosis.
Mucoepidermoid carcinoma is a malignant neoplasm of salivary gland origin that can present as a smooth-surfaced swelling or a non-healing ulcer on the palate. It occurs in a wide age range (5-7). Three histologic types are reported: low, intermediate and high; the low-grade type is more common in the oral cavity (5). Mucoepidermoid carcinoma accounts for 10% of all salivary gland neoplasms (5-7). While the majority occur in the parotid gland, some also occur in minor salivary glands, especially the palate, tongue, buccal mucosa, lips, and retromolar pad areas (5-7). It can occur at any age with a predilection for occurrence in young people (5). Studies by the Armed Forces Institute of Pathology (AFIP) find 44% of cases occurring in patients under 20 years of age, most commonly on the palate (5). Their youngest patient was nine months old. The low-grade lesions are slow-growing and painless, and not encapsulated; they sometimes resemble a mucocele, especially those at the retromolar pad area (6-7). Retromolar pad area mucoceles are rare, and for that reason it is best to biopsy early to exclude the possibility of a mucoepidermoid carcinoma masquerading as a mucocele. High-grade lesions tend to be more common in the parotid gland; they present as rapidly growing, painful lesions with facial nerve paralysis and sometimes with regional lymph node metastasis. Histologically, mucoepidermoid carcinoma consists of a variety of cell types and architectural patterns which constitute the three histologic gradings. Although low-grade mucoepidermoid carcinoma is characterized by an abundance of mucous-producing cells and duct-like structures with cystic dilation, the mere presence of certain types of cells and architecture should not be used to determine the histologic grade. Complete surgical removal with clean margins is the preferred treatment for the low-grade type. Radiotherapy has also been successfully used, especially when the tumor involves the surgical margins (5-7).
Congratulations! You are correct
Malignant lymphoma is frequently encountered in the tonsillar area and less commonly in the oral cavity. The tonsil is part of the Waldeyer’s ring (tonsil, nasopharynx and base of tongue) (11). Oral cavity and tonsillar area non-Hodgkin’s lymphoma constitute 13% of all extranodal lymphomas; 70% of the cases occur in the tonsils (8-12). Waldeyer’s ring lymphomas constitute 50% of all of extranodal head and neck lymphomas and are most commonly B-cell lymphomas, especially the diffuse large B-cell lymphoma type (DLBCL) which is aggressive in behavior and is slightly more common in males (8-12). It is more common in individuals around the fifth to seventh decade of age. Clinically, it presents as a sore throat with difficulty swallowing because of a large mass in the tonsillar area; it is usually unilateral and may or may not be ulcerated. Patients may also complain of difficulty hearing, pain, and airway obstruction (8-12). Radiation therapy and chemotherapy are the treatment of choice, sometimes combined given the stage of the disease. Histologically, the neoplasm is made up of medium-to-large B-lymphocytes with large round-to-oval nuclei and multiple nucleoli present at the periphery. The neoplastic cells with large nuclei and centrally located prominent nucleoli are more consistent with the immunoblastic type. The neoplasm may also demonstrate the presence of many macrophages, high mitotic activity, necrosis and apoptosis. Surgery may be performed to relieve some of the clinical symptoms. The five-year survival rate ranges from 60-90% based on the stage of the disease. The lower the clinical stage, the better the prognosis.
References
- Yu MC, Yuan JM. Epidemiology of nasopharyngeal carcinoma. Semin Cancer Biol 2002;12: 421–9.
- Agulnik M, Epstein JB. Nasopharyngeal carcinoma: Current management, future directions and dental implications. Oral Oncol 2008;44:617–27.
- Wang WC, Chen YK, Lin LM. Oral care experiences with 181 nasopharyngeal carcinoma patients receiving radiotherapy in a Taiwanese hospital. Auris Nasus Larynx 2008;35:230–4.
- Neville BW, Damm D, Allen CM, Bouquot E. Oral and maxillofacial pathology , 3rd edition. Philadelphia : Saunders; 2009: 428-429.
- Auclair PL, Ellis GL. Mucoepidermoid carcinoma. In Ellis GL, Auclair PL, Gnepp DR, editors. Surgical pathology of the salivary glands. Philadelphia: W.B. Saunders, 1991. p. 269-298.
- Hicks J, Flaitz C. Mucoepidermoid carcinoma of salivary glands in children and adolescents: assessment of proliferation markers. Oral Oncol. 2000 Sep;36(5):454-60
- Brandwein MS, Ivanov K, Wallace DI, Hille JJ, Wang B, Fahmy A, Bodian C, Urken ML, Gnepp DR, Huvos A, Lumerman H, Mills SE. Mucoepidermoid carcinoma: a clinicopathologic study of 80 patients with special reference to histological grading. Am J Surg Pathol 2001; 25:835-45.
- Epstein JB, Epstein JD, Le ND, Gorsky M. Characteristics of oral and paraoral malignant lymphoma: a population-based review of 361 cases. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2001, 92:519-525.
- Urquhart A, Berg R. Hodgkin’s and non-Hodgkin’s lymphoma of the head and neck. Laryngoscope 2001, 111:1565-1569.
- Kolokotronis A, Konstantinou N, Christakis I et al . Localized B-cell non-Hodgkin’s lymphoma of oral cavity and maxillofacial region: a clinical study. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2005; 99: 303–10.
- Barnes L, Eveson JW, Reichart P and Sidransky D. WHO classification of tumours; pathology and genetics of head and neck tumours. 2005.
- van der Waal RI, Huijgens PC, van der Valk P, van der Waal I. Characteristics of 40 primary extranodal non-Hodgkin lymphomas of the oral cavity in perspective of the new WHO classification and the International Prognostic Index. Int J Oral Maxillofac Surg 2005, 34:391-395.