March 2008: White lesions right buccal mucosa and left lateral tongue
Can you make the correct diagnosis?
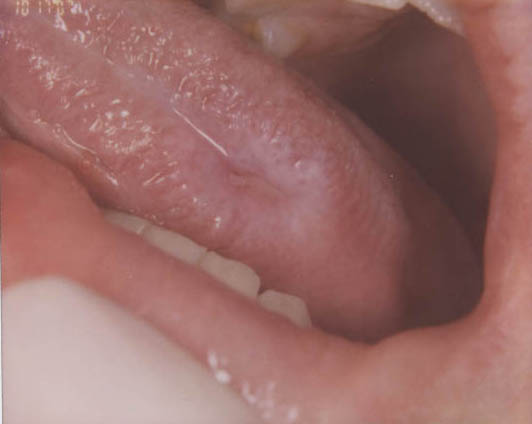
This is a 15-year-old boy who presented with a painful non-healing ulcer on the left lateral border of tongue (Figure 1). The ulcer was surrounded by a white plaque. The right buccal mucosa also had a white lesion which had a reticular pattern (Figure 2). The right buccal mucosa lesion was not ulcerated and was not painful. The left buccal mucosa had a hint of a white reticular lesion but was not as prominent as that of the right side. The ulcer was of one month’s duration while the right buccal mucosa lesion was of unknown duration. An incisional biopsy of the lateral tongue was performed.
Sorry! You are incorrect
Cannon first coined the term for this lesion in 1935 (1). Today, it is identified as a genetic condition caused by a point mutation in cytokeratin types 4 and 13 (2). This is a rare hereditary autosomal dominant condition that predominantly affects the non-keratinized mucosa including the oral cavity, nose, esophagus, vagina and rectum. The oral mucosa is more frequently affected. It is of variable penetrance (3). It typically occurs before age 20, usually it occurs at birth or during childhood or late adolescence (1-3). White sponge nevus can be mistaken for other types of leukoplakias. The history of the presence of these lesions since childhood combined with a family history of the disease and the histology are adequate in rendering a definitive diagnosis (2). Clinically, it presents as white, folded plaques that can peel away. The spongy mucosa can look translucent, simulating leukoedema. It can occur anywhere in the oral cavity but most commonly on the buccal mucosa followed by the lips, floor of mouth and the alveolar ridge (1-3). Histologically, the epithelium is thick and is covered by a thick and shaggy parakeratin with keratin plugging and intracellular edema of the spinous layer. Condensations around the nuclei are present in the upper spinous layer. No treatment is necessary. It has an excellent prognosis.
You are correct!
Lichen planus of the mouth is especially rare in children but is commonly encountered in adults. Lichen planus in children is particularly uncommon in the Western World but is reported in sub-Saharan Africa (4). One study documenting lichen planus in children from South East Nigeria (13 children, eight boys and five girls) aged between 3 and 15 years reports it to be more common on the skin than in the oral cavity.
Lichen planus is a common chronic immune mediated disease affecting 2% of the general adult US population. It has a variety of clinical presentations, management, and predisposing factors that renders it a family of diseases rather than one entity with a specific treatment modality (5). To be specific, lichen planus can be immune mediated, drug induced, associated with transplant rejection (also known as graft versus host disease), or associated with galvanic effect (when two separate restorations are in opposite contact with each other). It is also seen in families (though rarely), and is known to undergo a malignant transformation in about 2.5% of cases. Given the versatility of this disease, it is difficult to apply one treatment modality for all presentations (4-6).
The most common type of LP is the chronic T-lymphocyte-mediated disease where CD4 (early stage) and CD8 (later stages) T-lymphocytes are stimulated, releasing lymphokines such as a tumor necrosis factor, which lead to the destruction of the cells in the basal and parabasal cell layers (5). This type of oral LP tends to come and go, sometimes lasting throughout one’s lifetime. Lichen planus of the skin usually resolves within 1-3 years while only 20% of oral LP cases resolve in that period of time. Lichen planus occurs in adults between 30 and 70 years of age with a strong female predilection (4-6). It is very rare in children and for that reason, this case especially unique. It is often associated with stressful lifestyles. Skin LP presents as purplish, pruritic papules with a white keratotic surface, commonly on the flexor surfaces of the wrists, trunk and the genitalia. Oral LP presents as keratotic and reticular (the reticular pattern is the most common type), atrophic or erosive (the erosive type is the most important clinically), or plaque-like (the hypertrophic type, which is the least common). Oral LP presents most commonly in a symmetrical manner on the bilateral buccal mucosa but can occasionally affect on side of the buccal mucosa. Besides bilateral buccal mucosa, the tongue and gingival are commonly affected. Reticular type LP is asymptomatic and presents with interlacing lines against an erythematosus bluish background; the lines are known as the striae of Wickham. Erosive type LP, on the other hand, is symptomatic—patients complain of sensitivity to hot and cold, spicy, acidic, and alcoholic food and beverages. Erosive LP also presents in locations similar to those of the reticular type. At times, erosive LP can be hard to distinguish from other mucocutaneous diseases such as mucous membrane pemphigoid (MMP) and pemphigus vulgaris (PV). Hyperplastic or plaque LP is uncommon and presents as a confluent white plaque that is often mistaken for leukoplakia. The hyperplastic type is more common on the dorsal surface of the tongue, gingiva, and palate, making a clinical diagnosis of LP difficult at times, especially if the patient smokes. LP can also present on the gingiva alone as a thin and atrophic lesion known as desquamative gingivitis. The clinical differential diagnosis for desquamative gingivitis should include mucous membrane pemphigoid and pemphigus vulgaris.
A discussion of LP would be incomplete without addressing Lichenoid Drug Reaction, a condition that is especially common in elderly patients. It most frequently presents as erosive lichen planus on the bilateral buccal mucosa. It is associated with the ingestion of a number of medications including antibiotics, antihypertensive drugs, allopurinol (gout), diuretics, antidiabetics, gold, mercury, antihistamines and many others. The malignant potential of oral LP is a significant clinical concern, especially in long-term erosive lichen planus patients; transformation in reticular LP has also been documented, albeit rarely so (5). The World Health Organization (WHO) defines oral LP as a precancerous condition (6) with the full understanding that the risk for transformation is only around 2.5%. The locations of transformation are not in the high-risk locations of the conventional oral SCC, but rather involve the buccal mucosa, tongue and gingiva— the same locations as the conventional lichen planus.
Lichen planus is a disease that requires both clinical and histological features to arrive to a definitive diagnosis. Depending on the LP type, the epithelium ranges from thin and erosive to thick and keratotic (4-6). All types have a band-like infiltrate of T-lymphocytes. The basal cell layer shows evidence of degeneration; rete pegs are or are not present, basement membrane zone is thickened, and cystoid bodies (Civatte bodies) may be present. The immunofluorescence (IMF) features include positive staining with antibody to fibrinogen present along the basement membrane. Treatment ranges from no treatment for the asymptomatic reticular type, to topical steroids, intralesional steroid therapy (rarely used), and systemic steroid therapy (if the condition is severe such as in erosive LP). The best treatment for lichenoid drug reaction is replacement of the causing medication with a substitute. Treatment for transformation would follow the criteria for the treatment of oral squamous cell carcinoma. The reticular white patch on the buccal mucosa combined with the H & E histology and IMF findings renders this case to be lichen planus.
References
- Cannon AB, White sponge nevus of the mucosa (nevus spongious albus mucosa), Arch Dermatol Syphilol 31 (1935), pp. 365–370.
- Shibuya, J. Zhang, S. Yokoo, M. Umeda and T. Komori, Constitutional mutation of keratin 13 gene in familial white sponge nevus, Oral Surg Oral Med Oral Pathol Oral Radiol Endod 96 (2003), pp. 561–565
- Martelli H Jr Pereira SM, et al. White sponge nevus: report of a three-generation family. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2007 Jan; 103(1):43-7.
- Nrouka EN, Lichen planus in African children: a study of 13 patients. Pediatric Dermatology 2007; 24: 495-498.
- Silverman S, Gorsky M et al. A retrospective study of findings and management in 214 patients with oral lichen planus. Oral Surg Oral Med Oral Pathol 1991; 72:665–670.
- Silverman S. Oral lichen planus: a potentially premalignant lesion. J Oral Maxillofac Surg 2000; 58:1286–1288.
- Bundgaard T, S Bentzen, et al. Histopathologic, stereologic, Epidemiologic, and clinical parameters in the prognostic evaluation of squamous cell carcinoma of the oral cavity. Head & Neck. 1996. 18:142-152.
- Barasch A, Morse DE. Smoking, gender, and age as risk factors for site-specific intraoral squamous cell carcinoma. Cancer 1994. 73:509-513.
- Holmstrup P, JJ Thorn. Malignant development of lichen planus-affected oral mucosa. J Oral Pathol. 1988. 17:219-25.
- Sherman RG, Oral candidiasis. Quintessence Int. 2002 Jul-Aug; 33(7):521-32.
- Lynch DP.Oral candidiasis. Oral Surg Oral Med Oral Pathol. 1994 Aug;78(2):189-93.
Sorry! You are incorrect
Squamous cell carcinoma in a child of this age is extremely rare. Oral squamous cell carcinoma (OSCC) of the mouth is a highly aggressive neoplasm that currently ranks as the fifth most common malignant neoplasm worldwide and accounts for an estimated 90% of oral malignancies (7). Oral SCC occurs predominantly in males over the age of 40 years, with an observed male-to-female ratio of 2:1 generally and 1.4:1 in the USA (7-8). Excluding the outer lip, the most common sites (in decreasing order) are ventral and lateral surfaces of tongue (25-50%), floor of mouth (15%), gingiva (12%) and palate (9%). The buccal mucosa and retromolar pad areas (3%) have a relatively low incidence of occurrence (8) unless the patient is a chronic smokeless tobacco user. Oral SCC varies in presentation from deceptively innocent-looking to obviously malignant. It may present as a non-healing ulcer, or as red, white or mixed red-and-white lesions. Characteristic signs of oral SCC are non-healing ulcer, ulcer with rolled borders, fungation, fixation and induration. Rarely, OSCC may present as unexplained asymptomatic lateral neck lymphadenopathy (9). Oral SCC is most commonly associated with chemically induced mutagenesis, specifically tobacco and alcohol use and others such as long-standing erosive lichen planus (9). The age, the and the histology in this case are not supportive of SCC.
Sorry! You are incorrect
Given the diffuse nature of the white lesions in this patient, candidiasis should be considered. However, candidiasis is an opportunistic disease; and this patient did not fit any of the criteria under which candidiasis occurs in the mouth. Also, the white lesions did not wipe out, which they typically do in psuedomembranous types of candidiasis. The histology was also not supportive of this disease.
Candidiasis is the most opportunistic infection in the world. If it occurs in non-compromised patients it usually involves the tongue, skin folds, vagina and urinary tract. It tends to occur in compromised patients, especially in the GI tract, lungs, heart valve, kidneys and meninges (10-11). It is caused by Candida albicans, which presents in the form of delicate pseudo hyphae and budding spores. Candida is normally found, in up to 50% of the population, in the oral cavity (10). It affects high-risk patients such as infants under six months of age for lack of immunity, pregnant females, debilitated patients with chronic diseases, diabetics, patients who are immunosuppressed, and patients on long-term broad-spectrum antibiotics. It is classified into acute and chronic types. The acute type includes the acute pseudomembranous form found in chronically ill patients and infants (10). It presents as white, soft, slightly elevated plaques on the buccal mucosa and tongue. It can be wiped out leaving a relatively normal appearing mucosa, or slightly red mucosa. The acute atrophic form is erythematous and painful. The chronic type includes the chronic hyperplastic form which is a firm, white, persistent plaque on the lip, tongue and buccal mucosa. It is difficult to wipe off this kind of lesion. In terms of histology, besides candidal hyphae there is hyperparakeratosis, acanthosis and chronic mucositis. Biopsy would show hyphae and spores, and a cytology smear is just as effective. Treatment includes nystatin suspension for oral lesions. If the patient does not respond to treatment, check for diabetes, AIDS, or other endocrinopathies and immune suppressive diseases (11).