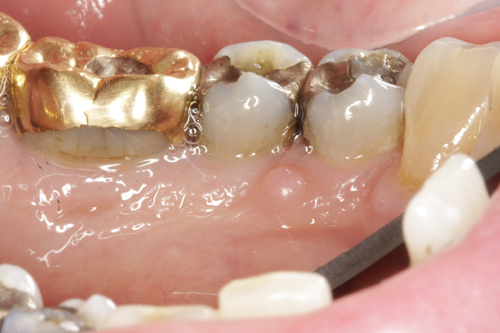
June 2009: Single small nodule lingual tooth #28
Can you make the correct diagnosis?
This is a 61-year-old white male seen at a periodontology clinic in October 2008 for an extraction and implant placement on tooth #13. Upon examination, this small (about 3mm), unilateral, exophytic, sessile and smooth-surfaced lesion was noted on the lingual gingiva of tooth #28 (Figure 1). It was of unknown duration and was asymptomatic. Radiographic findings were within normal limits with no evidence of bony involvement. The patient was unaware of its presence.
Sorry! you are incorrect
Fibroma is the most common soft tissue swelling in the oral cavity. The most common location is the buccal mucosa and the most common cause is trauma such as chronic chewing. However, the gingiva are not a common location for traumatic fibroma. Gingiva is a common location for a variant of fibroma known as giant cell fibroma. Giant cell fibroma should not be mistaken for peripheral giant cell granuloma, which is a completely different disease. The histology is not supportive of giant cell fibroma.
Giant cell fibroma is a benign nodule of fibrous connective tissue origin, a variant of fibroma but with an unknown etiology; trauma is not implicated, as is the case with irritation fibroma. It occurs in patients younger than those with the conventional irritation fibroma, usually in the first three decades of life. It is usually smaller than the irritation fibroma, averaging 5 mm in diameter. It can be sessile or pedunculated. It can be smooth-surfaced, or bluntly papillary or lobular; the latter is sometimes clinically mistaken for a papilloma. It most commonly occurs on the gingiva, especially mandibular gingiva, followed by the tongue and palate. Histologically, it is made up of a nodule of delicate connective tissue mass with stellate fibroblasts, some with multiple nuclei. The surface epithelium is corrugated with slender rete pegs. The histology is similar to that of retrocuspid papilla. Treatment ranges from simple surgical excision to laser surgery; it has a good prognosis and rarely recurs.
Sorry! you are incorrect
Small gingival swelling would be ideal for peripheral ossifying fibroma and should be seriously considered on the differential diagnosis. However, the histology in this case is not supportive of peripheral ossifying fibroma.
Peripheral; ossifying fibroma occurs exclusively on the gingiva. It has been reported, but rarely, on edentulous alveolar mucosa. It is believed to arise from the periodontal ligament or the periosteum. Clinically, this lesion is more common in young patients between 10 and 19 years of age and has a predilection for females, in whom almost two thirds of cases occur. They occur exclusively on the gingival; some report occurrences anterior to molar with a slight predilection for the maxilla. They present as well-demarcated sessile nodules, firm or hard depending on the amount of ossification and calcification. Color is usually pink but can be red focally if ulcerated. The specimen is made up of moderately cellular fibrous connective tissue with calcified bone or osteoid and some cementum-like hard tissue. The surface is usually ulcerated. Treatment includes surgical excision deep to include the periodontal ligament. If it recurs more than twice despite proper treatment, the associated tooth should be extracted. This lesion has a 16-20% recurrence rate and for that reason, the patient should be kept on follow-up visits for five years.
Sorry! you are incorrect
A single gingival swelling should raise suspicion of the presence of a gingival abscess. Abscesses, however, are inflamed, and the swelling is usually red with yellow center representing pus. At times, there will be a draining fistula. Neither the color nor the histology in this case is supportive of a gingival abscess.
Parulis or gumboil represents an accumulation of pus surrounded by a mass of hyperplastic granulation tissue present on the buccal gingiva as an exophytic mass simulating a gingival swelling. The origin of the pus is either from the apex of a non-vital tooth or a deep periodontal pocket. There is usually a sinus tract between the swelling and the apex of the tooth or the periodontal pocket. The use of a gutta-percha point can be of assistance in tracing the origin of the abscess. The source of the abscess should be treated to allow the gingival lesion to heal. Surgical removal of the exophytic lesion may or may not be necessary once the source of the abscess if treated.
Congratulations! You are correct
Ameloblastoma is one of the most common benign neoplasms of odontogenic origin. It accounts for 11% of all odontogenic neoplasms/hamartomas. Almost 99% of ameloblastomas are intra-osseous (within bone) and about 1% are present completely outside bone, usually in the gingiva; these are called peripheral ameloblastomas.
The intra-osseous ameloblastomas are divided into two types: multilocular ameloblastomas, which are aggressive and are treated with resection or en bloc, and unicystic ameloblastomas, which are less aggressive and are treated with curettage. Peripheral ameloblastomas are a slow-growing and non-aggressive counterpart of intra-osseous ameloblastomas. They are believed to originate from the basal cell layer of the surface epithelium and present as a small, well-circumscribed, firm nodule on the gingiva, mainly of the posterior mandible in middle-aged patients around 50 years of age. They are slightly more common in males. It is usually asymptomatic, pink as the surrounding mucosa, smooth-surfaced and sessile but can be can be rough surfaced, dark-colored and pedunculated. It can look very similar to peripheral ossifying fibroma, pyogenic granuloma or peripheral giant cell granuloma. It does not cause any bony resorption, therefore causing no radiographic changes. Histologically, peripheral ameloblastomas will show connection to the surface epithelium but with defined odontogenic epithelial islands in the connective tissue. The epithelial islands have palisaded and polarized columnar cells at the periphery and stellate reticulum cells in the center typical of follicular ameloblastoma morphology. They can also have acanthomatous morphology, which can be mistaken for well-differentiated squamous cell carcinoma. Treatment includes conservative surgical removal and follow-up for five years. Recurrence is rare.
References
- Dayan D, Bodner L, Hammel I, Wolman M. Histochemical characterization of collagen fibers in fibrous overgrowth (irritation fibroma) of the oral mucosa: effect of age and duration of lesion. Arch Gerontol Geriatr. 1994 Jan-Feb;18(1):53-7.
- Esmeili T, Lozada-Nur F, Epstein J. Common benign oral soft tissue masses.Dent Clin North Am. 2005 Jan;49(1):223-40
- Magnusson BC, Rasmusson LG. The giant cell fibroma. A review of 103 cases with immunohistochemical findings. Acta Odontol Scand. 1995 Oct;53(5):293-6.
- Hanemann JA, Pereira AA, Ribeiro Junior NV, Oliveira DT. Peripheral ossifying fibroma in a child: report of case. J Clin Pediatr Dent. 2003 Spring; 27(3):283-5.
- Walters JD, Will JK, Hatfield RD, Cacchillo DA, Raabe DA. Excision and repair of the peripheral ossifying fibroma: a report of 3 cases. J Periodontol. 2001 Jul; 72(7):939-44.
- Cuisia ZE, Brannon RB. Peripheral ossifying fibroma–a clinical evaluation of 134 pediatric cases. Pediatr Dent. 2001 May-Jun;23(3):245-8
- Gertner ME, Kebebew E. Multiple endocrine neoplasia type 2. Curr Treat Options Oncol. 2004 Aug;5(4):315-25.
- Vanoven BJ, Parker NP, Petruzzelli GJ. Peripheral ameloblastoma of the maxilla: a case report and literature review. Am J Otolaryngol. 2008 Sep-Oct;29(5):357-60.
- Damm DD. Exophytic mass of lingual mandible. Peripheral ameloblastoma. Gen Dent. 2008 Jul-Aug;56(5):490, 492-3.
- Curran AE, Byerly PD. Peripheral desmoplastic ameloblastoma: report of a rare case. J Oral Maxillofac Surg. 2008 Apr;66(4):820-5.
- Kishino M, Murakami S, Yuki M, Iida S, Ogawa Y, Kogo M, Toyosawa S. A immunohistochemical study of the peripheral ameloblastoma. Oral Dis. 2007 Nov;13(6):575-80.
Sorry! you are incorrect
The size, the color and the lingual gingiva are supportive of a traumatic neuroma but not the superior part of the gingival as an unlikely location for the mental foramen area. The histology is not supportive of a traumatic neuroma.
Traumatic neuroma is a reactive lesion resulting from an episode of repair of a damaged nerve. In the oral cavity, the most common site is the mental foramen, tongue and lips. It is seen more in edentulous patients with thin mandibular alveolar ridge and ill-fitting dentures. It can occur as a result of surgical trauma following an extraction (e.g. third molar removal) or removal of a neoplasm such as pleomorphic adenoma. It presents as a small smooth-surfaced nodule which can be painful on palpation; in about 25% to one-third of cases, it elicits pain which ranges from mild to severe and at times patients complain of burning sensation. It is particularly painful to palpation (called Tinnel’s sign) and those of the mental foramen area are painful to dentures impinging on them. Central lesions may occur and are usually radiolucent. Traumatic neuroma is usually small and slow growing. It occurs at any age but is most common during middle age. It has a slight predilection for females. Histologically, it is made up of hyperplastic nerve bundle surrounded by dense fibrous connective tissue. Treatment of choice is surgical excision with consideration for nerve repair procedure if involving the inferior alveolar or lingual nerves. Multiple neuromas have been associated with MEN (Multiple Endocrine Neoplasia) 2b syndrome, which should be identified early to avoid the development of medullary carcinoma of the thyroid, which can be fatal. Traumatic neuroma has an excellent prognosis following excision. As for the neuromas associated with MEN family syndromes, the prognosis depends on the other associated diseases.