Scalloped, Expansile Radiolucency, Right Posterior Mandible
Can you make the correct diagnosis?
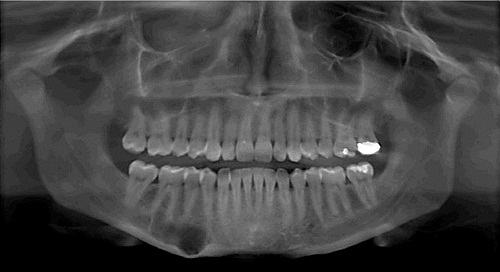
This is a 25-year-old Caucasian female who presented with an expansile and well-demarcated radiolucency in the right posterior mandible.
Sorry! you are incorrect
The radiographic findings of a unilocular radiolucency with scalloped border are typical of an odontogenic keratocyst (OKC). The age of this patient are also supportive of this condition. However, the described expansion of the bone especially with smaller OKC and the lack of proximity to teeth is unlike the behavior of an OKC. The histology is not supportive of an OKC.
Odontogenic keratocyst is an aggressive cyst known for its rapid growth and its tendency to invade the adjacent tissues, including bone. It has a high recurrence rate and is associated with bifid rib basal cell nevus syndrome. The majority of patients are in the age ranges of 20-29 and 40-59, but cases in patients ranging in age from 5 to 80 years have been reported. The distribution between sexes varies from equal distribution to a male-to-female ratio of 1.6:1, except in children. Odontogenic keratocyst predominantly affects Caucasian populations and, if one may judge from the limited evidence provided by the literature, is chiefly of Northern European descent.
Odontogenic keratocysts may occur in any part of the upper and lower jaw, with the majority (almost 70%) occurring in the mandible. They occur most commonly in the angle of the mandible and ramus. Posterior mandible is an area common to many benign odontogenic tumors such as ameloblastoma and odontogenic myxoma and is also a typical location for dentigerous cysts. Radiographically, OKCs present predominantly as unilocular radiolucencies with well-defined, sclerotic or scalloped borders. They may also present as multilocular radiolucencies. Odontogenic keratocysts of the maxilla are smaller in size when compared to those occurring in the mandible; larger OKCs tend to expand bone, but mildly–obvious clinical expansion (which is the case in this patient) should be viewed with suspicion for a neoplasm. OKCs can also present as small and oval radiolucencies between teeth simulating a lateral periodontal cyst, in an area of an extracted tooth simulating a residual cyst, at the apex of a vital tooth mistaken for a periapical cyst, or in the anterior maxilla between the central incisors simulating an incisive canal cyst. OKCs grow to sizes larger than any other odontogenic cysts. They usually penetrate the bone rather than expand it and grow in an anterior to posterior direction. Despite this aggressive growth, they often remain asymptomatic, thus growing to large sizes and hollowing the bone.
Odontogenic keratocysts are significant clinical entities due to their tendency for recurrence and destructive behavior. They are known to have a high recurrence rate, ranging from 13% to 60%. Complete surgical removal is the treatment of choice. Surgery includes enucleation, curettage, enucleation and peripheral ostectomy, and resection depending on the radiographic presentation, location and clinical behavior. Surgery combined with Carnoy’s solution or liquid nitrogen treatment has been effective in reducing recurrence rate. At times, adjacent or associated teeth are extracted in the interest of complete removal. Some investigators advocate marsupialization and occasionally resection of the more aggressive cysts that tend to perforate buccal and lingual bone. Resection is a rare modality of treatment. Most cysts recur within the first three years while others may recur as late as after 16 years. Conservative surgical removal and long-term follow-up is the treatment of choice by most clinicians.
Sorry! you are incorrect
The well-demarcated unilocular radiolucency with scalloped border should make one think traumatic bone cavity (TBC) as a potential diagnosis. However, the expansion and thinning of the inferior border of the mandible, although rarely reported, is highly unusual for TBC. The age and gender of this patient are also not typical of TBC. The histology and the clinical finding of a cavity filled with soft tissue is not supportive of this diagnosis either.
The traumatic bone cyst is best called a traumatic bone cavity since this condition does not represent a true cyst. Traumatic bone cavity (TBC) is not unique to the jawbones; it is also described in the long bones and is known as a simple solitary bone cyst occurring mostly in the humerus or femur, close to the epiphyseal plate. The long bone simple cyst is similar to the jaw traumatic bone cavity radiographically and occurs in the same age range. Trauma has been suggested as the etiology along with other non-substantiated theories such as cystic degeneration of a preexisting tumor or of the fatty marrow in the area.
Some reports suggest that it is more common in males while others report equal distribution between males and females. The long bone counterpart is more common in males by a ratio of 2.5:1. Most reports agree that the average age of occurrence is below 20 years of age. These lesions can occur, but are uncommon, over the age of 30. Kaugars reported a higher number of TBC cases in African-American females compared to the literature. The latter patients were over the age of 30. This may suggest an association with florid cemento-osseous dysplasia. The mandible is the most commonly affected area, where over 95% of cases occur, especially in the posterior premolar-molar area. TBCs are also known to cross the midline anteriorly. In one study, 27% of cases were anterior to the canine and some crossed the midline. They are usually unilocular and radiolucent, typically above the alveolar canal, and in many cases have a scalloped superior border squeezing between the roots of teeth. The latter are vital and are frequently found hanging within the empty cavity. About 25% of the lesions occur in the anterior mandible apical to the canine tooth and are usually round and unilocular; they can therefore be mistaken for periapical lesions, leading to an unnecessary endodontic treatment. Therefore, it is important to test the vitality of the teeth and carefully examine the radiographs for changes consistent with a periapical granuloma or cyst. Though expansion is not characteristic of TBC, it is described in about 26% of cases. TBCs are otherwise asymptomatic. The margins of these lesions range from very well defined to corticated to punched-out radiolucency. Pathologic fractures associated with traumatic bone cavity have been described in the jaws, but are rare. They are, however, more common in association with TBCs of the long bones.
Clinically, surgeons report an empty cavity at entrance in about two thirds of cases and cavities filled with straw-colored fluid in about one third of cases. Blood clots are also present occasionally. The bone cavity is scraped to generate bleeding, which is considered the treatment of choice for this condition. Other methods of treatment have been tried, such as packing the curetted cavity with autogenous blood, autogenous bone and hydroxyapatite. Various other reports demonstrate healing of TBC after injection of autogenous blood, after aspiration and after endodontic treatment. These lesions may spontaneously heal, but rarely. Biopsy material consists of fragments of viable bone and loose connective tissue. Osteoclast-like giant cells have also been described in a few cases. Exploration surgery usually leads to healing. Recurrence is rare.
Sorry! you are incorrect
Although intra-osseous hemangiomas are very rare in the jaw bones, the proximity of this lesion to the inferior alveolar canal should make one consider the diagnosis of intra-osseous hemangioma. They are however more commonly spider-web or multilocular radiolucency. The histology was not supportive of intra-osseous hemangioma.
Hemangioma is a family of benign developmental vascular anomalies, the majority occurring in the first decade of life, including at birth. Specifically, they are benign proliferations of blood vessels. They progress through two stages of growth: a rapid growth phase followed by an involution phase. They are predominantly of soft tissue origin, especially the skin and mucosa, but can occur anywhere else, including within bone. The most common types are the capillary hemangiomas that affect 1% of all newborns in the United States. Half of all hemangiomas occur in the head and neck area, especially the tongue. They are the most common cause of macroglossia. They can also occur on the buccal mucosa and lips. In addition, hemangiomas have a slight predilection for occurrence in females.
Central or intra-osseous hemangiomas are rare. They are more common in the vertebrae and skull bone, but not in the jaw bones. When they occur in the jaws, the mandible is affected twice as commonly as the maxilla; they occur most often in the inferior alveolar canal ramus area. They are typically slow-growing and can be slightly expansile. Radiographically, they are usually radiolucent with a spider-web appearance. They are sometimes multilocular with soap-bubble morphology; occasionally, they have a sun-ray appearance. They can occur in or involve the inferior alveolar canal, rendering it larger and irregular. They can resorb and displace teeth. They occur in the first decade of life, like their soft-tissue counterparts. They may displace teeth and cause bleeding around the involved teeth.
The treatment of hemangioma depends on its size, its relationship to other anatomical structures and the rate of blood flow. Some hemangiomas spontaneously involute, especially capillary hemangiomas. If a hemangioma persists, local injections with corticosteroids or sclerosing agents have been shown to be effective. However, complications with intralesional injections are described. Interferon alfa-2a has also been successfully used. Surgical procedures include excisional scalpel surgery for smaller soft tissue lesions and laser removal for larger lesions. En bloc or larger resections have been used for central hemangiomas. CO2; argon and other types of laser have also been used with various success rates. The prognosis ranges from good to poor with gross facial deformity and compromised function depending on the size and site.
Congratulations! You are correct
It is rare, but the close proximity of the expansile radiolucency to the inferior alveolar canal should make one think intra-osseous peripheral nerve neoplasm as well as intra-osseous hemangioma.
Schwannoma is a benign, encapsulated soft tissue neoplasm of Schwann cell origin that is usually associated with a nerve trunk. Up to 48% of Schwannomas occur in the head and neck area. They are slow-growing, firm, rubbery, smooth-surfaced nodule. This neoplasm more commonly occurs in young and middle aged patients with equal sex distribution. Tongue is the most common location but it can also occur in the lips, buccal mucosa and floor of mouth. It is also described within the jaw bones especially the mandible in association with the inferior alveolar canal.
Intra-osseous schwannomas are rare but when they occur, the posterior mandible is the most common location and is usually in association with the inferior alveolar canal in the body and ramus area. This patient is in the body of the mandible. The literature is clear that intra-osseous schwannomas of the jaws are by far more common in the mandible than in the maxilla. In one report of 44 cases, 39 of the specimens were from the mandible, especially the body and ramus of the mandible. They are usually associated with the inferior alveolar nerve and are often associated with pain, swelling and parasthesia. This patient did not have pain or parasthesia but there was mild swelling. The average age for this population was 34 years of age similar to that of the soft tissue counterpart. As mentioned earlier, schwannomas generally speaking are slow-growing which would include both the soft tissue and intra-osseous types. Radiographically, Intra-osseous schwannomas are well-circumscribed unilocular radiolucencies as is the case with our patient. Conservative surgical removal is the treatment of choice and recurrence is rare.
References
- Shear M. Odontogenic keratocysts: natural history and immunohistochemistry. Oral Maxillofacial Surg Clin N Am. 2003; 15: 347-362.
- Oda D, Rivera V et al. Odontogenic keratocyst: the northwestern USA experience. J Contemp Dent Pract. 2000 Feb 15; 1(2): 60-74.
- Zachariades N, Papanicolaou S et al. Odontogenic keratocysts: Review of the literature and report of sixteen cases. J Oral Maxillofac Surg. 1985; 43: 177-182.
- Kumar ND, Sherubin JE, Raman U, Shettar S. Solitary bone cyst. Indian J Dent Res. 2011 Jan-Feb;22(1):172-4.
- Kahler B. Traumatic bone cyst suggestive of a chronic periapical abscess: A case report. Aust Endod J. 2011 Aug;37(2):73-5.
- Chan YC, Giam YC. Guidelines of care for cutaneous haemangiomas. Ann Acad Med Singapore. 2005 Jan;34(1):117-23.
- Lambrecht JT, Stubinger S, Hodel Y. Treatment of intraoral hemangiomas with the CO2 laser. Schweiz Monatsschr Zahnmed. 2004;114(4):348-59.
- Eliot CA, Castle JT. Intraosseous hemangioma of the anterior mandible. Head Neck Pathol. 2010 Jun;4(2):123-5.
- Hansen T, Kunkel M, Katenkamp D, Eletr S, Wagner W. Hemangioma of the mandible: case report with special emphasis on bone degradation. Oral Maxillofac Surg. 2009 Dec;13(4):239-42.
- Neville B, Damm DD, Allen CM, Bouquot J. 3rd ed. Philadelphia: Saunders; 2009. Oral and Maxillofacial Pathology; pp. 526–528.
- Chi AC, Carey J, Muller S. Intraosseous schwannoma of the mandible: a case report and review of the literature. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2003;96(1):54–65.