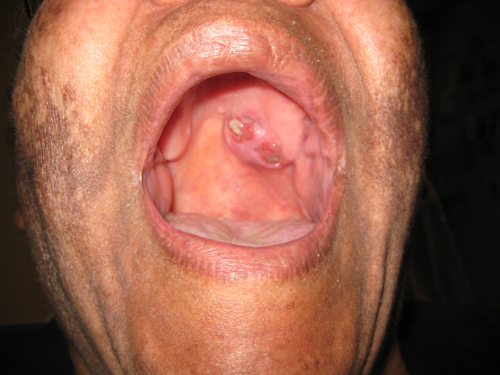
July 2009: Large ulcerated swelling left posterior palate
Can you make the correct diagnosis?
This is a 69-year-old African American female with a slowly growing lesion initially described to be “like a scar” or a “bony spicule” on the left posterior, lateral soft palate bordering on the junction of hard palate. The patient is edentulous and wears full dentures. The lesion grew continuously for two years and the dentist trimmed the maxillary denture to avoid “rubbing” against the denture. The swelling was initially pink but became red and purple and eventually ulcerated. However, it was not painful. At the patient’s first presentation at the Oral Surgery clinic, the lesion measured 2.5 x 3.5 cm and was exophytic and ulcerated. It was located at the junction of hard and soft palate (Figure 1).
Sorry! you are incorrect
The age, location, gender, duration and clinical presentation are all consistent with pleomorphic adenoma (PA). PA is the most common salivary gland neoplasm and should be considered whenever a case potentially falls into this category. The ulcerated surface, however, is not supportive of a diagnosis of PA; it can be supportive of carcinoma ex-mixed tumor (ex-PA) but not of a benign PA. The histology is not supportive of PA.
Pleomorphic adenoma is the most common benign salivary gland neoplasm of both the major and minor salivary glands. It originates from the myoepithelial cells and the reserve cells of the intercalated ducts. It accounts for 80% of all benign salivary gland neoplasms. It occurs in both major and minor salivary glands and accounts for up to 77% of parotid, 68% of submandibular, and 43% of minor salivary gland tumors (1-4). It is most common in females 30-50 years of age, but it is also described in children (1). One study reports 1% of cases affecting children under 10 years of age and 5.9% between the ages of 10-20 (1, 3). It presents as a small, painless, slowly enlarging nodule. If left untreated, it can enlarge significantly, sometimes increasing by several pounds in weight (1-4). It occurs in the oral cavity, especially the palate and lips (1-3). On the palate, it is usually located in the posterior hard palate or anterior soft palate but can also be in the posterior soft palate; PA usually occurs in the posterior and lateral palate, as opposed to torus palatines, which usually occurs in the middle hard palate and in the anterior. The posterior hard palate mixed tumor is fixed due to the bone-bound anatomy of the region; the tumor is otherwise movable. Histologically, mixed tumor has a wide variety of cellular and pattern manifestations; the main cellular components are epithelial duct-like structures and mesenchymal-like tissue such as myxochondroid matrix. These lesions are generally encapsulated, ranging from predominantly myxoid (36%) to extremely cellular (12%) (1-4). Complete surgical removal with clean margins is the preferred treatment (1-4). Palatal lesions respond well to excision in one piece with the periosteum and overlying mucosa. PA has a good prognosis, but it has a tendency for recurrence (up to 44%) if not treated thoroughly (1-4). Risk of recurrence is less if it occurs in the minor salivary glands (up to 20%). The risk of malignant transformation is about 5% (1, 3).
Sorry! you are incorrect
In this case, the location, age, color change to purple, and ulcerated surface is consistent with mucoepidermoid carcinoma and therefore should be considered on the differential diagnosis. The histology, however, is not supportive of mucoepidermoid carcinoma.
Mucoepidermoid carcinoma is a malignant neoplasm of salivary gland origin that can present as a smooth-surfaced swelling or a non-healing ulcer on the palate. It occurs in a wide age range (5-7). Three histologic types are reported: low, intermediate and high; the low-grade type is more common in the oral cavity (5). Mucoepidermoid carcinoma accounts for 10% of all salivary gland neoplasms (5-7). While the majority occur in the parotid gland, some also occur in minor salivary glands, especially the palate, tongue, buccal mucosa, lips, and retromolar pad areas (5-7). It can occur at any age with a predilection for occurrence in young people (5). Studies by the Armed Forces Institute of Pathology (AFIP) find 44% of cases occurring in patients under 20 years of age, most commonly on the palate (5). Their youngest patient was nine months old. The low-grade lesions are slow-growing and painless, and not encapsulated; they sometimes resemble a mucocele, especially those at the retromolar pad area (5-7). Retromolar pad area mucoceles are rare, and for that reason it is best to biopsy early to exclude the possibility of a mucoepidermoid carcinoma masquerading as a mucocele. High-grade lesions tend to be more common in the parotid gland; they present as rapidly growing, painful lesions with facial nerve paralysis and sometimes with regional lymph node metastasis. Histologically, mucoepidermoid carcinoma consists of a variety of cell types and architectural patterns which constitute the three histologic gradings. Although low-grade mucoepidermoid carcinoma is characterized by an abundance of mucous-producing cells and duct-like structures with cystic dilation, the mere presence of certain types of cells and architecture should not be used to determine the histologic grade. Complete surgical removal with clean margins is the preferred treatment for the low-grade type. Radiotherapy has also been successfully used, especially when the tumor involves the surgical margins (5-7).
Sorry! you are incorrect
The location and ulcerated surface is consistent with the diagnosis of necrotizing sialometaplasia. The two-year duration, however, is not. The histology is also not supportive of this diagnosis.
Necrotizing sialometaplasia is a spontaneous, self-healing, rapidly growing benign inflammatory lesion primarily affecting the minor salivary gland tissue (8). It usually heals within three months of occurrence. Clinically, however, it is an aggressive-looking lesion. It is of unknown etiology, but transient local ischemia is suggested as a possible etiology (8-10). The latter is seen with recent dental injections to the area; the vasoconstrictor effect of dental injections is believed to induce local ischemia. The local infarction hypothesis is supported by the histology of necrotic acini with intact cell membrane which is seen in coagulative necrosis. It is more common in the fourth and fifth decade of life, and occurs more often in males by a ratio of 2 to 1. The palate, especially the junction of hard and soft palate, is the most common location of occurrence, accounting for about 75% of cases. The condition presents as single, bilateral (10) or as multiple ulcers. The ulcers are deep and necrotic with a flat edge. They can reach more than three centimeters in size. The clinical symptoms, when present, include mild pain or parasthesia. The clinical presentation can be mistaken for a malignant neoplasm such as adenoid cystic carcinoma or surface squamous cell carcinoma. No treatment is recommended, but a biopsy is recommended to establish the baseline diagnosis. Most lesions heal within ten weeks after biopsy (8-10).
Congratulations! You are correct
This is a common low-grade malignant neoplasm of minor salivary gland origin. It is most common in minor salivary glands and is very rarely described in major salivary glands (11-13). It is characterized by a slow infiltrative growth pattern, bland and uniform cytology, and variations in histological patterns, occasionally simulating pleomorphic adenoma and other times simulating adenoid cystic carcinoma (13). PLGA was first reported by Batsakis as terminal duct carcinoma; with time, it went through a number of name changes and polymorphous low grade adenocarcinoma is the most used name today (11-13). This slow growing, painless, rarely metastasizing neoplasm most commonly (in up to 70% of cases) occurs on the palate, followed by the buccal mucosa and upper lip. The lesion is usually exophytic and can be ulcerated or with intact surface mucosa. It affects patients in the fifth and sixth to eighth decade and is more common in females (11-13). It is also reported in children, but rarely. A range of histological patterns are described including tubular, trabecular, papillary, papillary cystic, cribriform or solid. Cytologically, the cells are uniform and the nuclei are bland. Mitosis is rare; perineural invasion is common and is described in about 76% of cases (13). The connective tissue stroma is usually hyalinized but can occasionally be mucinous or chondro-myxoid in appearance. The latter would be reminiscent of the connective tissue stroma of pleomorphic adenoma. The treatment of choice is complete surgical removal with clean margins and the prognosis is excellent. The ten year survival rate is 95%; recurrence and metastasis occur at a rate of around 10-15% (13).
References
- Waldrom CA. Mixed tumor (pleomorphic adenoma) and myoepithelioma. In Ellis GL, Auclair PL, Gnepp DR, editors. Surgical pathology of the salivary glands. Philadelphia: W.B. Saunders, 1991. p. 165-186.
- Foote FW Jr., Frazell EL. Tumors of the major salivary glands. Atlas of tumor pathology, Section IV, Fascicle 11, 1st Series. Washington DC: Armed Forces Institute of Pathology, 1954.
- Bablani D, Bansal S, Shetty SJ, Desai R, Kulkarni SR, Prasad P, Karjodkar FR. Pleomorphic adenoma of the cheek: a case report and review. J Oral Maxillofac Surg. 2009 Jul;67(7):1539-42.
- Witt RL, Rejto L. Pleomorphic adenoma: extracapsular dissection versus partial superficial parotidectomy with facial nerve dissection. Del Med J. 2009 Mar;81(3):119-25.
- Auclair PL, Ellis GL. Mucoepidermoid carcinoma. In Ellis GL, Auclair PL, Gnepp DR, editors. Surgical pathology of the salivary glands. Philadelphia: W.B. Saunders, 1991. p. 269-298.
- Hicks J, Flaitz C. Mucoepidermoid carcinoma of salivary glands in children and adolescents: assessment of proliferation markers. Oral Oncol. 2000;36(5):454-60
- Brandwein MS, Ivanov K, Wallace DI, Hille JJ, Wang B, Fahmy A, Bodian C, Urken ML, Gnepp DR, Huvos A, Lumerman H, Mills SE. Mucoepidermoid carcinoma: a clinicopathologic study of 80 patients with special reference to histological grading. Am J Surg Pathol 2001; 25:835-45.
- Brannon RB, Fowler CB, Hartman KS. Necrotizing sialometaplasia: a clinicopathological study of sixty nine cases and review of the literature. Oral Surg Oral Med Oral Pathol 1991; 72:317-25.
- Keogh PV, O’Regan E. Necrotizing sialometaplasia: an unusual bilateral presentation associated with antecedent anaesthesia and lack of response to intralesional steroids. Case report and review of the literature. Br Dent J. 2004; 196: 79-81.
- Sandmeier D, Bouzourene H. Necrotizing sialometaplasia: a potential diagnostic pitfall. Histopathology. 2002;40:200-201.
Sorry! you are incorrect
Given the patient’s history of lung cancer, one has to consider tumor metastasis. The location, however, is not supportive of such diagnosis. Neither is the histology.
Cancer metastasis to the oral cavity is neither specific nor common. Although it constitutes fewer than 1% of all oral malignant neoplasms, it may have a devastating result to the patient mainly because metastasis to other sites has already developed or is inevitable (14-16). Theoretically, any malignant neoplasm can metastasize to the oral cavity, but in actuality few do and out of the ones that do, the majority are carcinomas rather than sarcomas. The most common malignant neoplasms that metastasize to the mouth are from the breast, lung, kidney and prostate (14-16). Malignant neoplasms from the thyroid, pancreas, colon, and liver have also been described. Breast cancer is the most common neoplasm to metastasize to the oral cavity altogether; however, lung and prostate cancers are the most common neoplasms to metastasize to the oral cavity in men. In the most cases, the oral presentation is a secondary diagnosis where the primary diagnosis of the distant organ has been already made and the patient has had or is undergoing treatment for it, as was the case with this patient’s lung cancer. Rarely, the oral lesion is the first manifestation of the disease. By far the most common location of occurrence is the posterior mandible, where 80% of cases occur, followed by the gingiva. The maxilla is a rare location for tumor metastasis. It is mostly described in adults over the age of 30 and rarely in children. Pain and swelling are the most common clinical symptoms, which was the case with this patient. They may also present as asymptomatic, simulating a periapical lesion or it can cause anesthesia and parasthesia, especially when it involves the inferior alveolar canal. The latter results in so-called “numb-chin syndrome.” Tooth loosening, displacement and sharp resorption have also been described. Gingival swelling like a pyogenic granuloma, as in this case, has also been described. The radiographic appearance of irregular bony destruction is also common for a metastatic tumor. The majority of neoplasms cause bony destruction with ill-defined borders, the moth-eaten appearance of some bony destruction indicating aggressive behavior. It is also important to mention that at times, well-demarcated lesions with a benign morphology, as well as cystic radiographic morphology, have also been described. Metastatic neoplasms from the prostate may also be bone-forming, resulting in either radiopaque or mixed radiopaque and radiolucent lesions misdiagnosed as a benign fibro-osseous lesion.
The diagnosis of tumor metastasis to the oral cavity carries a poor prognosis because the oral cavity is usually not an isolated site and tends to project more disseminated clinical behavior (14-15). Patients are typically treated with chemotherapy and the five-year survival rate is very low.