Return to Case of the Month Archives
Multiple Papillary Lesions, Generalized, Oral Cavity
Dolphine Oda, BDS, MSc
doda@u.washington.edu
Contributed by
Dr. Michael Martin
Department of Oral Medicine, University of Washington, Seattle
Case Summary and Diagnostic Information
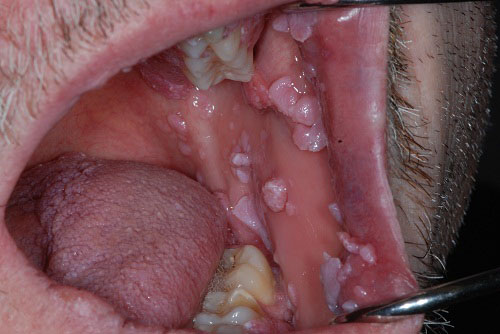
This is a 44-year-old white male with numerous pink/white papillary lesions, some of which are exophytic and many of which are flat and spongy.
Diagnostic Information Available
This is a 44-year-old white male with numerous pink/white papillary lesions, some of which are exophytic and many of which are flat and spongy (Figures 1 & 2). The papillary exophytic lesions are present on the lips, bilateral buccal mucosa and vestibule, tongue and floor of mouth. The flatter, spongier lesions are present on the gingiva and hard palate. These lesions are of over two years’ duration. The lesions on the buccal mucosa become trapped between teeth when eating, making it hard to chew. The patient has similar lesions in the peri-anal area that are being treated with topical 5 FU cream, while the oral lesions are treated with combined surgical removal and weekly intra-lesional injections with three million units of alpha interferon B.

Figure 1 Photograph represents the typical appearance of the oral cavity at multiple visits of the University of Washington Oral Medicine Clinic. Note the multiple, variable size pink/white papillary lesions of the buccal mucosa and spongy flat pink/red lesions of the gingiva (upper and lower).
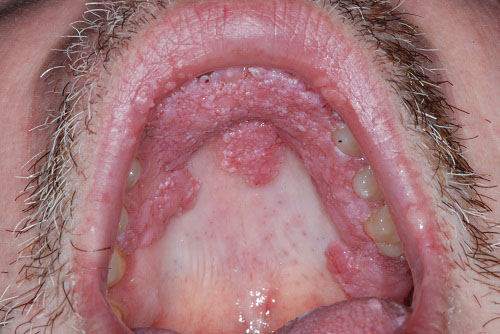
Figure 2 Photograph represents the typical appearance of the oral cavity at multiple visits of the University of Washington Oral Medicine Clinic. Note the generalized spongy flat pink/red lesions of the palatal gingiva and hard palate.
The patient’s past medical history includes multidrug-resistant HIV and previous poor compliance with HAART medications. Other medical problems include significant reactive airway disease and recurrent bronchial and pulmonary infections with several subspecies of Mycobacterium avium. He also has a history of heavy cigarette smoking which he stopped recently. He is on numerous medications including Isoniazid, Clarithromycin, Ciprofloxacin, INH and pyridoxine, Nystatin, Pyridoxine, Nasonex nasal spray, DuoNeb inhaler, Albuterol, Amlodipine, Fluticasone, Lisinopril, Bactroban, Darunavir, Etravirine, Raltegravir, Norvir, Pyridox topical and Dyazide.
The patient reported progressive development of white/pink papillary and flat spongy lesions occurring throughout the oral cavity, including the lips, bilateral buccal mucosa and vestibule, gingiva and palate. These lesions are not painful but some become trapped between teeth while eating, making it very difficult to chew. The papillary lesions are pedunculated while the spongy lesions are flat and sessile, involving most of the gingiva and palate.
Under local anesthesia, the larger pedunculated lesions, especially those that tended to become trapped between teeth, were excised and submitted for microscopic examination. The other lesions received weekly injections with three million units of alpha interferon B.
Histologic examination reveals multiple pieces of soft tissue composed of papillary surface epithelium (Figure 3) with an underlying fibrous connective tissue core. The latter was loose and vascular and was focally infiltrated by lymphocytes. The papillary projections ranged from blunt to elongated and were all covered by parakeratin of variable thickness. The keratin layer of some of the specimens was infiltrated by fungal hyphae and spores. The spinous layer showed evidence of cells with empty-looking cytoplasm and small nuclei consistent with koilocytes (Figure 4). The immunohistochemistry stain with antibody to human papilloma virus types 6/11, 16, etc (Figure 5) was strongly positive.
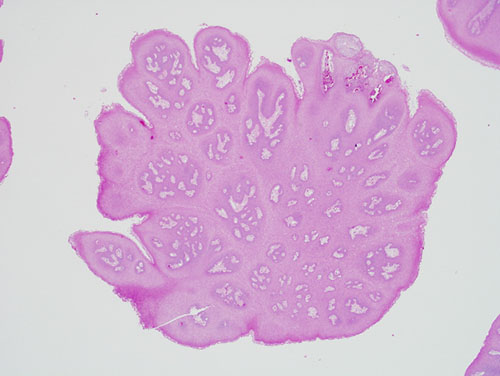
Figure 3 Low power (x40) H & E histology shows papillary epithelium covered by parakeratin and supported by fibrous connective tissue core.
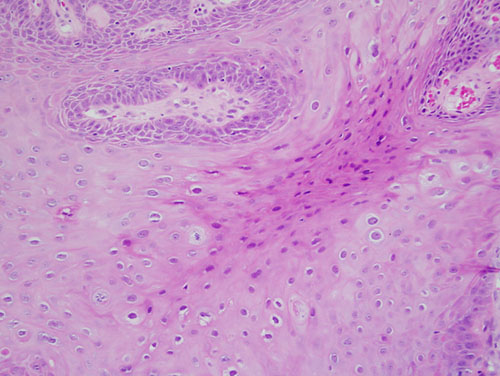
Figure 4 Low power (x100) H & E histology demonstrating spinous layer cells with mitosoid cells and koilocytes.
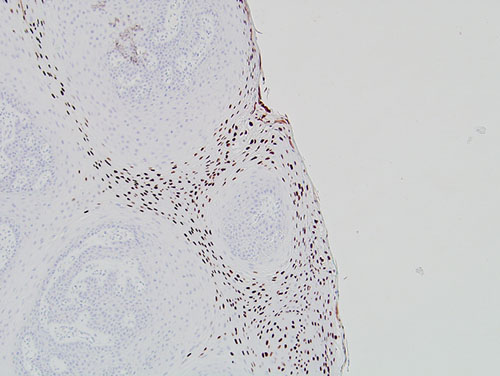
Figure 5 Low power (x100) Immunohistochemistry stain with antibody to HPV types 6/11, 16, demonstrating strong positive nuclear staining at the superficial spinous layer.
After you have finished reviewing the available diagnostic information