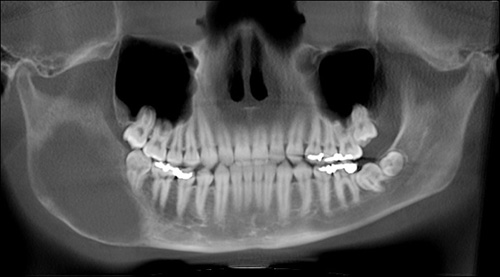
Large radiolucent/radiopaque lesion right posterior mandible and ramus
Can you make the correct diagnosis?
This is a 17-year-old Hawaiian male whose chief complaint is of right facial swelling and asymmetry of six months’ duration.
Sorry! you are incorrect
The location (posterior mandible and ramus), the jaw expansion leading to facial asymmetry, the radiographic changes and the age of the patient are all consistent with aneurysmal bone cyst. The histology, however, is not.
Aneurysmal bone cyst (ABC) has a tumor-like clinical behavior but is not a true neoplasm. It occurs more commonly in long bones and the vertebrae (1-3). It also affects the jaws, but rarely. In the jaws, the mandible is more commonly affected by a ratio of 3:1; the posterior mandible, angle and ramus are the most common locations (1-3). This lesion occurs before the age of 20 and is slightly more common in females. The etiology for this condition is unknown but some investigators believe it to be due to high-pressure hemorrhage. Bone expansion, asymmetry, pain and swelling are common clinical presentations (1-3). Aspiration may yield blood. Radiographically, ABC presents as honeycombed or multilocular but can also be a unilocular radiolucency. Expansion and thinning leading to ballooning or ‘blow out’ distention of bone are highly suggestive of this condition. Histologically, it is made up of granulation tissue with blood-filled sinusoidal spaces with scattered multinucleated giant cells and bony trabeculae. This lesion is best treated with thorough curettage but resection is used in large cases.
Sorry! you are incorrect
The radiographic changes, the clinical behavior of expansion and asymmetry and the age of the patient are all consistent with fibrous dysplasia. Although the location is unusual for FD, it can still be included on the differential diagnosis. The histology however is not supportive of FD.
The etiology of fibrous dysplasia is unknown. The monostotic (one bone or bone complex area) form constitutes approximately 80% of all fibrous dysplasia cases while the polyostotic affects one or more bones with multiple lesions (4). However, FDs are expansile and disfiguring lesions, whether single or multiple, which differentiate them from the usually flat osteomas of Gardner’s syndrome. Monostotic FD, which involves the jaws, affects males and females equally. It occurs in childhood and at puberty and usually stops growing at age 30. It appears as an asymptomatic swelling of the maxilla or mandible; the maxillary lesion is the most common. It may involve bones other than the maxilla, including the zygoma, sphenoid and others. It is usually unilateral and is known to displace the teeth, but otherwise is firmly seated (4-6). The growth is usually slow, but rapid growth has been described, especially during puberty. The radiographic appearance, especially of the maxilla, is classically described as a ground glass appearance where fine radiopacity is noted. The mandibular lesions are much more deceptive because they tend to vary more, thus making diagnosis with a radiograph difficult. They range from cystic unilocular radiolucency to multilocular radiolucency to the classical ground glass radio-opacity (5-6).
Polyostotic fibrous dysplasia constitutes approximately 20% of FD cases (5). Two principle sub-types are described; Jaffe’s and Albright’s syndrome. The latter represents the more severe form with endocrine disturbances (precocious puberty in females). Polyostotic FD is more common in females than males (4-6). Multiple bones are affected including long bones in addition to the jawbones. The clinical presentation depends on the type. Albright’s is associated with hormonal changes, including precocious puberty and cafe au lait spots. Jaffe’s has multiple bones with FD and cafe au lait spots but no hormonal changes. Treatment may be necessary and is preferably performed after cessation of growth due to the high incidence of re-growth and requirement for secondary procedures. The surgeons decided against treatment and opted to keep the patient on close observation. Radiation therapy is contraindicated since significant incidence of development of osteosarcoma in the irradiated bone has been documented. Malignancies such as osteosarcoma arising in an area of FD that has not been irradiated have been described, but rarely; these occur mainly in irradiated lesions. The overall prognosis of this patient is good with close follow-up visits.
Sorry! you are incorrect
The location, expansion and radiolucent/radiopaque radiographic changes are consistent with brown tumor of hyperparathyroidism. The age and sex of the patient is not; neither is the histology.
Hyperparathyroidism is a condition caused by excessive production of parathyroid (PTH) hormone. It can be primary or secondary in type. Primary hyperparathyroidism is associated with an increase in PTH production, usually due to parathyroid gland hyperplasia, sometimes due to benign adenoma(s) of the gland(s) and rarely due to adenocarcinoma affecting one or more of the parathyroid glands (7-8). Brown tumor is more commonly associated with primary hyperparathyroidism. Secondary hyperparathyroidism is one of the sequelae of chronic renal disease (renal osteodystrophy); like the primary type, it is caused by increased parathyroid hormone (7-8). Primary hyperparathyroidism is three times more common in women and is more common in middle-aged patients. Clinically, both types may produce multiple bone lesions histologically indistinguishable from those produced by central giant cell granuloma (CGCG). It must be noted that CGCG is usually an isolated lesion, while hyperparathyroidism usually consists of generalized or multiple bony lesions affecting more than one bone or affecting multiple areas of one bone. The name ‘brown tumor’ reflects the chocolate-like color of the lesion. Primary hyperparathyroidism is associated with hypercalcemia, hypophosphatemia, and complications associated with hypercalcemia. Secondary hyperparathyroidism is usually associated with hypocalcemia but sometimes can have a normal calcium level with a high phosphate level (7-8). The signs and symptoms of hyperparathyroidism are designated by “stones, bones, moans and groans.” Radiographic features include generalized loss of bone density with loss of lamina dura and irregular radiolucent lesions (brown tumor), either single or multiple. The bone may have a ‘ground-glass’ appearance. Histopathologically, the brown tumor is made up of granulation tissue with aggregates of multinucleated giant cells, extravasated red blood cells and hemosiderin deposition. Treatment ranges from medical or surgical management of the underlying condition such as removal of hyperplastic or neoplastic glands, which should result in the resolution of the condition to renal dialysis and renal transplant. Enucleation and curettage of certain brown tumors is indicated.
Congratulations! You are correct
Juvenile ossifying fibroma (JOF) is a benign neoplasm of bone origin and is an aggressive variant of central ossifying fibroma of the jaws (9-12). It is by far more common in children under the age of 15. It is most common in the craniofacial bone, especially the maxilla. Two histologic variants are described, the trabecular and psammomatoid types. Trabecular JOF is histologically characterized by cellular connective tissue stroma interspersed with strands of trabeculae young bone with prominent osteoblastic rimming. Psammomatoid JOF is characterized by cellular connective tissue stroma with small and uniform cementum-like hard tissue resembling Psammoma bodies. Trabecular JOF occurs more commonly in the jaw bones; it is about twice as common in the maxilla as in the mandible. Psammomatoid JOF occurs more commonly in the paranasal sinuses (about 70% of cases) with 20% of cases occurring in the maxilla and 10% in the mandible (12). Trabecular JOF tends to occur in younger patients with a range of 8.5-12 years while Psammomatoid JOF affects older children with a mean age of 20-22. Both types are slightly more common in males (11).
Both types are benign but locally aggressive lesions simulating low-grade sarcoma behavior with a tendency for fast growth, invading the surrounding tissue and destroying bone. Both histological types have a high recurrence rate ranging from 30 to 56% (12). Treatment ranges from thorough curettage to resection to curettage with systemic subcutaneous interferon injections. The latter has been reported to be effective in inhibiting tumor growth and recurrence.
References
- Prasad S, Raghaviah AM, Sharma N, Einstein A and Raraswathi TR. Aneurysmal bone cyst of the mandible: Report of a case and review of the literature. JOMFP. 2007; 11: 38-41.
- Rousseau A, El Okeily M, Vidal N, Siberchicot F, Zwetyenga N. Aneurysmal bone cysts of the mandible. Rev Stomatol Chir Maxillofac. 2009 Dec;110(6):329-34.
- Roychoudhury A, Rustagi A, Bhatt K, Bhutia O, Seith A. Aneurysmal bone cyst of the mandible: report of 3 cases. J Oral Maxillofac Surg. 2009 Sep;67(9):1996-2004
- Parekh SG, Donthineni-Rao R et al. Fibrous Dysplasia. J Am Acad Orthop Surg. 2004;12:305-313.
- Tsai EC, Santoreneos S et al. Tumors of the skull base in children: review of tumor types and management strategies. Neurosurg Focus. 2002: 15;12(5).
- Zacharin M. Paediatric management of endocrine complications in McCune-Albright syndrome. J Pediatr Endocrinol Metab. 2005;18:33-41.
- Sutbeyaz Y, Yoruk O, Bilen H, Gursan N. Primary hyperparathyroidism presenting as a palatal and mandibular brown tumor. J Craniofac Surg. 2009 Nov;20(6):2101-4.
- Proimos E, Chimona TS, Tamiolakis D, Tzanakakis MG, Papadakis CE. Brown tumor of the maxillary sinus in a patient with primary hyperparathyroidism: a case report. J Med Case Reports. 2009 Jul 6;3:7495.
- Williams HK, Mangham C, Speight PM. Juvenile ossifying fibroma. An analysis of eight cases and a comparison with other fibro-osseous lesions. J Oral Pathol Med. 2000;29:13–18.
- Eversole LR, Leider AS, Nelson K. Ossifying fibroma. A clinicopathologic study of sixty-four cases. Oral Surg Oral Med Oral Pathol. 1985;60:505–511.
- Samir El Mofty Psammomatoid and trabecular juvenile Ossifying Fibroma of the craniofacial skeleton: Two distinct Clinicopathological entities. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2002; 93:296- 304.
- Johnson LC, Yousefi M, Vinh TN, Heffner DK, Hymans VJ and Hartman KS. Juvenile active ossifying fibroma, its Nature, Dynamics and Origin Acta Otolaryngol 1991; suppl 1 488: 1-40.