January 2009: Diffuse, large swelling right palate
Can you make the correct diagnosis?
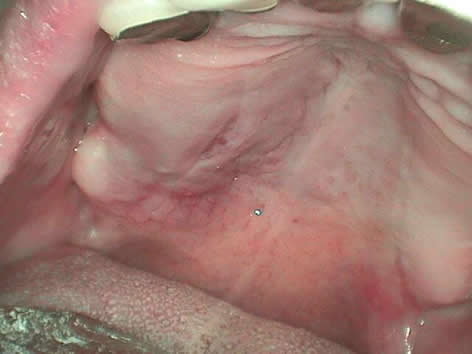
This is an 81-year-old white female whose chief complaint was that her partial denture was impinging on the right side of her palate, where a large swelling was identified. The palatal swelling was of one month’s duration. The partial denture pushed into the swelling, causing some tenderness in the area. The swelling was diffuse, soft and deep with red overlying mucosa and a groove (Figure 1). It was described to be 2.0 x 1.0 x 0.75 cm in size.
Sorry! you are incorrect
With a partial denture pushing on the palate, necrotizing sialometaplasia would be a logical condition to consider in the differential diagnosis. The histology in this case, however, is not supportive of it.
Necrotizing sialometaplasia is a spontaneous, self-healing, rapidly growing benign inflammatory lesion primarily affecting the minor salivary gland tissue (1). It usually heals within three months of occurrence. Clinically, however, it is an aggressive looking lesion. It is of unknown etiology, but transient local ischemia is suggested as a possible etiology (1-3). The latter is seen with recent dental injections to the area; the vasoconstrictor effect of dental injections is believed to induce local ischemia. The local infarction hypothesis is supported by the histology of necrotic acini with intact cell membrane which is seen in coagulative necrosis. It is more common in the fourth and fifth decade of life, and occurs more often in males (2:1 male: female ratio). The palate in general, and the junction of hard and soft palate in particular, are the most common locations of occurrence, accounting for about 75% of cases. The condition presents as single, bilateral (3) or multiple ulcers. The ulcers are deep and necrotic with a flat edge. They can reach more than three centimeters in size. The clinical symptoms, when present, include mild pain or parasthesia. The clinical presentation can be mistaken for a malignant neoplasm such as adenoid cystic carcinoma or surface squamous cell carcinoma. No treatment is recommended, but a biopsy is recommended to establish the baseline diagnosis. Most lesions heal within ten weeks after biopsy (1-3).
Sorry! you are incorrect
Given the grayish color and fluctuant nature of the early presentation, mucous-producing neoplasms should be included on the differential diagnosis. The histology, however, is not supportive of this diagnosis.
Mucoepidermoid carcinoma is a malignant neoplasm of salivary gland origin that can present as a smooth-surfaced swelling or a non-healing ulcer on the palate. It occurs in a wide age range (9-11). Three histologic types are reported: low, intermediate and high; the low-grade type is more common in the oral cavity (9). Mucoepidermoid carcinoma accounts for 10% of all salivary gland neoplasms (9-11). While the majority occur in the parotid gland, some also occur in minor salivary glands, especially the palate, tongue, buccal mucosa, lips, and retromolar pad areas (9-11). It can occur at any age with a predilection for occurrence in young people (9). Studies by the Armed Forces Institute of Pathology (AFIP) find 44% of cases occurring in patients under 20 years of age, most commonly on the palate (9). Their youngest patient was nine months old. The low-grade lesions are slow-growing and painless, and not encapsulated; they sometimes resemble a mucocele, especially those at the retromolar pad area (10-11). Retromolar pad area mucoceles are rare, and for that reason it is best to biopsy early to exclude the possibility of a mucoepidermoid carcinoma masquerading as a mucocele. High-grade lesions tend to be more common in the parotid gland; they present as rapidly growing, painful lesions with facial nerve paralysis and sometimes with regional lymph node metastasis. Histologically, mucoepidermoid carcinoma consists of a variety of cell types and architectural patterns which constitute the three histologic gradings. Although low-grade mucoepidermoid carcinoma is characterized by an abundance of mucous-producing cells and duct-like structures with cystic dilation, the mere presence of certain types of cells and architecture should not be used to determine the histologic grade. Complete surgical removal with clean margins is the preferred treatment for the low-grade type. Radiotherapy has also been successfully used, especially when the tumor involves the surgical margins (9-11).
Sorry! you are incorrect
Given the location of occurrence and the fact that the patient wears a partial denture, soft tissue swellings–especially those related to ill-fitting dentures–should be included on the differential diagnosis. The clinical presentation in this case, however, is not supportive of denture-related reactive lesions such as epulis fissuratum or inflammatory papillary hyperplasia. Benign or malignant soft tissue neoplasms should still be included on the differential diagnosis. The histology in this case was not supportive of any of the soft tissue reactive or neoplastic conditions.
The palate is a common location for soft tissue swellings regardless of whether they are reactive or neoplastic, or whether they are benign or malignant (4-8). Reactive soft tissue swellings of fibrous connective tissue origin are commonly associated with ill-fitting dentures (5-6, 8) or with dentures that are worn 24 hours a day without proper cleaning (7). The latter presents as small papillary red lesions on the hard palate while denture hyperplasia (epulis fissuratum) presents as redundant folded tissue in the facial aspects of the alveolar ridge, more often in the anterior maxilla or mandible (5-6). The swelling in this patient does not fit the description of any of the denture-related hyperplasias described above.
Soft tissue neoplasms (4, 6), i.e. peripheral nerve neoplasms such as neurofibromas and schwannomas, can occur on both the anterior and posterior hard palate. Smooth and skeletal muscle neoplasms, especially rhabdomyosarcomas, can occur on the palate and are common in the head and neck area; these are especially common in the pediatric population. Lipomas are rare in the mouth and are especially rare on the palate.
Congratulations! You are correct
Non-Hodgkin’s lymphoma is a malignant neoplasm of lymphocyte origin, mostly of B-lymphocyte but can also be of T-lymphocyte origin. Several of skin lymphomas are of T-lymphocyte origin (12-16). The head and neck region is a frequent site for lymphomas, especially the Waldeyer’s ring. However, the oral cavity is not a common site except in certain types such as African type Burkitt’s lymphoma. Around 60,000 cases of NHLs are reported annually in the U.S.A. and about one third die of the disease. Diffuse large B cell lymphoma (DLBCL) and follicular lymphoma (FL) are the most common types with DLBCL being more common than FL and more aggressive in behavior. Clinically, FL is a low-grade malignancy with better prognosis than many NHLs. It occurs almost exclusively in adults, mostly in elderly patients with median survival rate of approximate 8–10 years (14-15). This disease has a spectrum of biological behavior ranging from very mild form that spontaneously reverses itself to those that would progress to a more aggressive type simulating DLBCL. About 85% of the cases have the t(14;18)(q32;q21) translocation (15) which results in over expression of the BCL-2 (14) oncogene leading to the inactivation of the programmed cell death of the B-lymphocytes. Treatment depends on the clinical stage of the disease and on the histologic grade. Mild forms of the disease are treated with local radiation while the more advanced cases are treated with chemotherapy combined with radiation. Cytotoxic T-lymphocyte gene therapy is used as well for the more advanced and recurring type of FLs.
References
- Brannon RB, Fowler CB, Hartman KS. Necrotizing sialometaplasia: a clinicopathological study of sixty nine cases and review of the literature. Oral Surg Oral Med Oral Pathol 1991; 72:317-25.
- Keogh PV, O’Regan E et al. Necrotizing sialometaplasia: an unusual bilateral presentation associated with antecedent anaesthesia and lack of response to intralesional steroids. Case report and review of the literature. Br Dent J. 2004; 196: 79-81.
- Sandmeier D, Bouzourene H. Necrotizing sialometaplasia: a potential diagnostic pitfall. Histopathology. 2002;40:200-201.
- Neville B, Damm D et al. Textbook of Oral & Maxillofacial Pathology. Saunders; 2009: third edition.
- Freitas JB, Gomez RS, De Abreu MH, Ferreira E Ferreira E. J Oral Rehabil. 2008 May;35(5):370-4. Relationship between the use of full dentures and mucosal alterations among elderly Brazilians.
- Mujica V, Rivera H, Carrero M. Prevalence of oral soft tissue lesions in an elderly Venezuelan population. Med Oral Patol Oral Cir Bucal. 2008 May 1;13(5):E270-4.
- Poulopoulos A, Belazi M, Epivatianos A, Velegraki A, Antoniades D. The role of Candida in inflammatory papillary hyperplasia of the palate. J Oral Rehabil. 2007 Sep;34(9):685-92
- Naveen Kumar J, Bhaskaran M. Denture-induced fibrous hyperplasia. Treatment with carbon dioxide laser and a two year follow-up. Indian J Dent Res. 2007 Jul-Sep;18(3):135-7
- Auclair PL, Ellis GL. Mucoepidermoid carcinoma. In Ellis GL, Auclair PL, Gnepp DR, editors. Surgical pathology of the salivary glands. Philadelphia: W.B. Saunders, 1991. p. 269-298.
- Hicks J, Flaitz C. Mucoepidermoid carcinoma of salivary glands in children and adolescents: assessment of proliferation markers. Oral Oncol. 2000 Sep;36(5):454-60
- Brandwein MS, Ivanov K, Wallace DI, Hille JJ, Wang B, Fahmy A, Bodian C, Urken ML, Gnepp DR, Huvos A, Lumerman H, Mills SE. Mucoepidermoid carcinoma: a clinicopathologic study of 80 patients with special reference to histological grading. Am J Surg Pathol 2001; 25:835-45.
- Epstein JB, Epstein JD, Le ND, Gorsky M. Characteristics of oral and paraoral malignant lymphoma: a population-based review of 361 cases. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2001, 92:519-525.
- Urquhart A, Berg R. Hodgkin’s and non-Hodgkin’s lymphoma of the head and neck. Laryngoscope 2001, 111:1565-1569.
- Aster JC, Longtine JA. Detection of BCL2 rearrangements in follicular lymphoma. Am J Pathol. 2002;160:759–763.
- Horsman DE, Okamoto I, Ludkovski O, et al. Follicular lymphoma lacking the t(14;18)(q32;q21): identification of two disease subtypes. Br J Haematol. 2003;120:424–433.
- van der Waal RI, Huijgens PC, van der Valk P, van der Waal I. Characteristics of 40 primary extranodal non-Hodgkin lymphomas of the oral cavity in perspective of the new WHO classification and the International Prognostic Index. Int J Oral Maxillofac Surg 2005, 34:391-395.