Well-Demarcated Radiolucency with Sharply Angulated Tooth Resorption
Can you make the correct diagnosis?
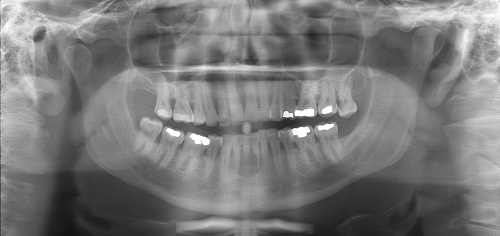
This is a 42-year-old white male with a one-year history of an aggressive radiolucency of the anterior mandible causing a sharp edge and irregular resorption of teeth #s 23 & 24.
Sorry! you are incorrect
The sharp-edged tooth resorption and the more raggedy tooth resorption one year later indicates an aggressive, if not an outright malignant, process. Various rare metastatic malignancies should be included in the differential diagnosis of such an aggressively behaving lesion. However, the patient has no history of any malignant neoplasm; furthermore, malignant neoplasms usually metastasize to the posterior mandible. The patient’s lack of a history of a malignant neoplasm elsewhere should not prevent the inclusion of metastasis on the differential diagnosis since in rare cases; the oral manifestation can be the first sign of a silent primary malignancy. However, the histology in this case is not supportive of any metastatic disease.
Cancer metastasis to the oral cavity is neither specific nor common. Although such cases constitute less than 1% of all oral malignant neoplasms, it may have a devastating result to the patient mainly because metastasis to other sites has already developed or is inevitable (1-3). Theoretically, any malignant neoplasm can metastasize to the oral cavity, but in actuality few do and of the ones that do, the majority are carcinomas rather than sarcomas. The most common malignant neoplasms that metastasize to the mouth are from the breast, lung, kidney and prostate (1-3). Malignant neoplasms from the thyroid, pancreas, colon, and liver have also been described. Breast cancer is the most common neoplasm to metastasize to the oral cavity altogether. Lung and prostate cancers are the most common neoplasms to metastasize to the oral cavity in men. In most cases, the oral presentation is a secondary diagnosis when the primary diagnosis of malignancy in a distant organ has been already made and the patient has had or is undergoing treatment for it. In rare cases, the oral lesion is the first manifestation of the disease. By far the most common location is the posterior mandible, where 80% of cases occur, followed by the gingiva. This condition is mostly described in adults over the age of 30 and rarely in children. Pain and swelling are the most common clinical symptoms. Metastatic lesions may also present as asymptomatic, simulating a periapical lesion, or with gingival swelling like a pyogenic granuloma. They can cause anesthesia and parasthesia, especially when they involve the inferior alveolar canal. The latter results in so-called “numb-chin syndrome.” Tooth loosening, displacement and sharp resorption have also been described. The radiographic appearance of the borders can range from moderately well demarcated to diffusely irregular. The majority of neoplasms cause bony destruction with ill-defined borders; the moth-eaten appearance of some bony destruction indicates aggressive behavior. It is also important to mention that at times, well-demarcated lesions with a benign morphology, as well as cystic radiographic morphology, have also been described. Metastatic neoplasms from the prostate and, rarely, from the breast can be bone-forming, resulting in radiopaque or mixed radiolucent and radiopaque lesions misdiagnosed as benign fibro-osseous lesions.
Tumor metastasis to the oral cavity carries a poor prognosis because the oral cavity is usually not an isolated site and tends to project a more disseminated clinical behavior (1-3). Patients are typically treated with chemotherapy and the five-year survival rate is very low.
Sorry! you are incorrect
Again, the sharp-edged tooth resorption and the more raggedy tooth resorption one year later indicates an aggressive, if not an outright malignant, process. Malignant neoplasms such as plasmacytoma should be included in the differential diagnosis of such an aggressively behaving lesion. Primary plasmacytoma of the mouth is very rare but is common in individuals with diagnosed multiple myeloma; however, this patient would be young for this condition and has no history of multiple myeloma. The histology is not supportive of plasmacytoma.
Plasmacytoma is an isolated manifestation of multiple myeloma. Multiple myeloma is a clonal neoplastic proliferation of plasma cells (myeloma cells), which are terminally differentiated B-lymphocytes. It is most common in individuals 60-75 years of age, occurs more often in males, and is rare in persons under 40 years of age (4-7). It is twice as common in blacks as in the general population. It occurs most commonly in bone and in a multicentric manner (multiple locations at the same time), hence the name multiple myeloma (4-7). This malignant neoplasm presents more commonly in bone but is also described in soft tissue without bony involvement (extramedullary). About 40-50% of bone-isolated plasmacytomas will progress to multiple myeloma while only 10-12% of soft tissue plasmacytomas will progress to multiple myeloma (4-7). Normal plasma cells, which are immunoglobulin-producing cells, can produce IgA, IgD, IgG, IgM, and IgE. Neoplastic plasma cells can produce any of these antibodies but tend to produce IgG and IgA. The most common clinical presentation of plasmacytoma is severe bone pain, especially that of the lumbar spine, which is usually aggravated with movement (4-7). Bone lesions occur in 70% of patients and usually lead to hypercalcemia, bone fracture and vertebral collapse. Hypercalcemia may lead to soft-tissue calcifications. The most common bones affected by multiple myeloma are the vertebrae, skull, mandible, ribs, pelvis, clavicles and scapula. Jaws are affected in about 30% of cases (4-7). Extramedullary tissue such as the liver, spleen and lymph nodes can also be affected. Patients with multiple myeloma are susceptible to anemia and therefore often experience fatigue and weakness. They can also develop renal failure due to monoclonal light chain (Bence Jones protein). About 15% of patients develop amyloid deposition in a variety of soft tissues, including the G-I tract and the oral cavity, specifically the tongue. Amyloid in the tongue can present as small yellow nodules or plaques; they can be deep seated within the tongue, causing slurring. They can also occur around the eyes, again as small yellow plaques or nodules (4). Radiographically, multiple myeloma has a distinct presentation of “punched out” radiolucencies but the radiolucency can also be ill defined. This is particularly true of skull lesions. The mandible and maxilla can be affected, but the radiographic presentation is not as distinct as that of skull lesions (4-7). It is important to note that histology and immunohistochemistry alone cannot differentiate between isolated cases of plasmacytoma and the full diseases of multiple myeloma. Pathologists usually render the histologic diagnosis of plasmacytoma while oncologists render the clinical diagnosis of multiple myeloma.
Histologically, the biopsy of a patient with isolated plasmacytoma or a patient with the full disease of multiple myeloma demonstrates sheets of monotonous mononuclear cells with plasmacytic differentiation. The atypical plasma cells usually show nuclear and cellular atypia. Mitosis is usually present (4-7). The neoplastic cells are monoclonal; this can be supported by an immunohistochemistry stain with kappa or lambda light chains. They are also specific with CD138, a marker for plasmacytoid cell. The final diagnosis of multiple myeloma is determined through a combination of histology, serum and urine protein electrophoresis, blood test for myeloma protein (monoclonal gammopathy), and radiographic changes. Treatment includes chemotherapy, bisphosphonates to control hypercalcemia, bone marrow transplantation, and radiation therapy. The overall prognosis depends on age; younger patients have a better prognosis than older patients.
Sorry! you are incorrect
The presence of a radiolucency in the anterior mandible resorbing teeth in a sharp-edged manner should make one think of sarcomas as well. Chondrosarcoma is the most likely sarcoma to occur in this location and in a patient of this age, but chondrosarcomas rarely present as completely radiolucent. Fibrosarcoma can also be included on the differential diagnosis, but this condition is extremely rare in the jaws. The histology in this case is not supportive of any sarcoma, including chondrosarcoma.
Chondrosarcoma is a malignant mesenchymal neoplasm of cartilage origin. It is uncommon, especially in the jaws. However, it is still much more common than its benign counterpart (chondroma) in the jaws. It is more common in the maxilla, especially in the incisor area. It can occur at any age but is more common in males around the sixth decade of life (8-10). Unlike osteosarcoma, it has a low tendency for metastasis. In general, the prognosis is better than that of osteosarcoma, but it varies depending on the stage of the disease. It commonly presents as an asymptomatic swelling with buccal and lingual expansion. Patients may experience unexplained paresthesia, headache, and the loosening and loss of teeth as well as tooth resorption. Radiographically, it presents as a mottled, ill-defined radiolucency with snowflake or punctate calcifications (8-10). It is very rare for chondrosarcoma to be completely radiolucent. Sometimes, the teeth will show a widened periodontal ligament space. Histologically, it is characterized by immature and pleomorphic cartilage, but at times the cartilage is benign-looking. It is rare for the cartilage to calcify or differentiate and form bone (8-10). Therapy for chondrosarcoma ranges from wide local excision to radical resection with or without chemotherapy, depending on the stage of the disease. The prognosis ranges from good to poor.
Congratulations! You are correct
Although sharp and raggedy-edged tooth resorption is not a characteristic of central giant cell granuloma (CGCG), this lesion was histologically typical of CGCG and the patient’s blood test was negative for hyperparathyroidism.
Jaffe first coined the term “reparative” for central giant cell granuloma. Most pathologists have since dropped the term “reparative” for lack of evidence that the pathogenesis is a reparative process. CGCG is described as a non-neoplastic process and yet can behave in a very aggressive and expansile manner, destroying bone and displacing teeth. Over 60% of CGCG cases occur in patients younger than 30 years of age, with twice as many occurrences in females as in males. CGCG is classified into aggressive and non-aggressive types; the aggressive type tends to occur in younger patients and causes disfiguration, especially after surgery. Over 70% of cases occur in the mandible anterior to the first molar tooth. This lesion has also been described in other cranio-facial and small long bones such as those of the hands and feet (11-15).
The usual treatment for CGCG is surgery, ranging from curettage and en bloc to resection (11-12). The latter is used in aggressive and recurring cases (11). In the past ten years or so, alternatives to surgery have emerged with successful results, saving some patients from facial disfigurement. Steroid injections (14) are the most successful alternative treatment thus far; they require injections weekly or every 2-3 weeks, have no known side effects (even in children), and are the least expensive alternative treatment. Other treatments include: calcitonin injections or nasal spray (15), which require daily injections or a nasal spray of salmon calcitonin for about a year and are safe for pregnant females; and interferon alfa-2a injections (13-15), which are administered 2-3 times per week for several months and are the most expensive alternative treatment. A report by Carlos and Sedano (13) from Guatemala presented four patients with large CGCG cases treated with steroid injections. They demonstrated that regular steroid injections led to remarkable responses in all four patients without any side effects. All four patients had initial biopsies confirming the histological diagnosis of CGCG and had endocrine testing to rule out hyperparathyroidism. Two were pediatric patients, two-and-a-half and six years of age, with large lesions of the mandible and maxilla, respectively. They responded more rapidly to steroid injections than did the other two patients, who were adults of 31 and 34 years of age with large lesions of the maxilla and mandible, respectively. Injections were administered every two to three weeks. Complete healing, with small residual radiolucency requiring no further treatment, was noted in three of the patients. One patient, the six-year-old boy, had a maxillary swelling that was reduced from 5 cm in size to only 0.5 cm after four injections. The surgical specimen from the six-year-old consisted of fibrocollagenous stroma with few giant cells in comparison to the original biopsy, which consisted of loose and vascular granulation tissue with many giant cells. Fibrocollagenous stroma, with or without giant cells, has been described in association with both calcitonin and steroid treatment (14-15). There was no evidence of recurrence in these patients after 2-7 years of follow-up, nor were there any steroid-related complications in any of the patients. One must keep in mind that this report involves a very small number of cases; few firm conclusions can be reached, but the results are remarkable and show a more favorable outcome than surgical intervention, particularly in large and aggressively behaving pediatric cases.
References
- A. Hirshberg and A. Buchner, Metastatic tumours to the oral region. An overview. Oral Oncol. 1995; 31: 355–360.
- Ivan der Waal, RIF, Buter, J. Oral metastases: report of 24 cases. Br J Oral Maxillofac Surg. 2003; 41: 3-6.
- Uhler IV, Fahs GR, Dolan LA. Metastasis of cervical carcinoma to the mandible: report of a case. J Am Dent. Assoc. 1972; 85: 363-364.
- Akhtar K, Laghari NA, Haq AU, Anees M, Rehman SU, Alam MI. Multiple myeloma in younger age.. J Coll Physicians Surg Pak. 2009 Jan;19(1):62-3
- Poggio CE. Plasmacytoma of the mandible associated with a dental implant failure: a clinical report. Clin Oral Implants Res. 2007 Aug;18(4):540-3. Epub 2007 Apr 30.
- Canger EM, Celenk P, Alkan A, Günhan O. Mandibular involvement of solitary plasmocytoma: a case report. Med Oral Patol Oral Cir Bucal. 2007 Jan 1;12(1):E7-9.
- Souza LN, Farias LC, Santos LA, Mesquita RA, Martelli H Jr, De-Paula AM. Asymptomatic expansile lesion of the posterior mandible. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2007 Jan;103(1):4-7. Epub 2006 Oct 16.
- Neville BW. Oral & maxillofacial pathology. 2nd ed. Philadelphia: W.B. Saunders; pages 664-666, 2009.
- Anil S, Beena VT et al. Chondrosarcoma of the maxilla. Case report. Aust Dent J. 1998;43:172-174.
- Hayt MW, Becker L et al. Chondrosarcoma of the maxilla: panoramic radiographic and computed tomographic with multiplanar reconstruction findings. Dentomaxillofac Radiol. 1998;27:113-116.
- Whitaker SB, Vigneswaran N, Budnick SD, Waldron CA. Giant cell lesions of the jaws: evaluation of nucleolar organizer regions of varying behavior. J Oral Pathol Med 1993; 22(9):402-5.
- Tallan EM, Olsen KD, McCaffrey TV, Unni KK, Lund BA. Advanced giant cell granuloma: a twenty-year study. Otolaryngol Head Neck Surg 1994; 110(4):413-8.
- Carlos R, Sedano HO. Intralesional corticosteroids as an alternative treatment for central giant cell granuloma. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2002; 93(2):161-6.
- O’Regan EM, Gibb DH, Odell EW. Rapid growth of giant cell granuloma in pregnancy treated with calcitonin. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 200; 92(5):532-8.
- Collins A. Experience with anti-angiogenic therapy of giant cell granuloma of the facial bones. Ann R Australas Coll Dent Surg 2000; 15:170-5.