Recurrent large anterior mandibular unilocular radiolucency
Can you make the correct diagnosis?
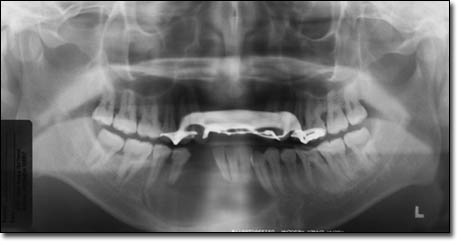
This is a 28-year-old Asian male of slender build. He first presented on August 8, 1990 with a large anterior mandibular expansion.
Sorry! you are incorrect
The large unilocular radiolucency is radiographically consistent with one of the ways that an odontogenic keratocyst would present and for that reason, it should be included on the differential diagnosis. OKC is an aggressive cyst known for its rapid growth and its tendency to invade the adjacent tissues, including bone. It has a high recurrence rate and is associated with bifid rib basal cell nevus syndrome (1, 2). The majority of patients are in the age ranges of 20-29 and 40-59, but cases in patients ranging in age from 5 to 80 years have been reported. The distribution between sexes varies from equal distribution to a male-to-female ratio of 1.6:1, except in children (1, 2). Odontogenic keratocyst predominantly affects Caucasian populations and, if one may judge from the limited evidence provided by the literature, is chiefly of Northern European descent (1).
Odontogenic keratocysts may occur in any part of the upper and lower jaw, with the majority (almost 70%) occurring in the mandible. They occur most commonly in the angle of the mandible and ramus (1). Radiographically, OKCs present predominantly as unilocular radiolucencies with well-defined, sclerotic or scalloped borders. They may also present as multilocular radiolucencies. Larger OKCs tend to expand bone, but mildly—obvious clinical expansion should be viewed with suspicion for a neoplasm. It can present in an area of an extracted tooth simulating a residual cyst as is the case with this patient. OKCs grow to sizes larger than any other odontogenic cysts. They usually penetrate the bone rather than expand it and grow in an anterior to posterior direction (3). Despite this aggressive growth, they often remain asymptomatic, thus growing to large sizes and hollowing the bone.
Odontogenic keratocysts are significant clinical entities due to their tendency for recurrence and destructive behavior. They are known to have a high recurrence rate, ranging from 13% to 60% (1, 2). Complete surgical removal is the treatment of choice. Surgery includes enucleation, curettage, enucleation and peripheral ostectomy, to resection depending on the radiographic presentation, location and clinical behavior. Surgery combined with Carnoy’s solution or liquid nitrogen treatment has been effective in reducing recurrence rate (1, 2). At times, adjacent or associated teeth are extracted in the interest of complete removal. Some investigators advocate marsupialization and occasionally resection of the more aggressive cysts that tend to perforate buccal and lingual bone. Resection is a rare modality of treatment. Most cysts recur within the first three years while others may recur as late as after 16 years (1, 2). Conservative surgical removal and long-term follow-up is the treatment of choice by most clinicians. The histology of this case is not supportive of Odontogenic keratocyst.
Sorry! you are incorrect
Ameloblastoma is one of the most common benign neoplasms of odontogenic origin. It accounts for 11% of all Odontogenic neoplasms/hamartomas (4-6). It is a slow-growing, persistent, and locally aggressive neoplasm of epithelial origin. It affects a wide range of age distribution but is mostly a disease of adults, at an average age of 33, with equal sex distribution. Reports from Africa and India show male predilection. It has a prevalence to patients of black origin (5).
About 85% of ameloblastomas occur in the posterior mandible, most in the molar-ramus area, some in the anterior mandible. About 15% occur in the maxilla, the vast majority in the posterior maxilla as is the case in our patient.
Ameloblastoma is rarely described in children. It is characteristically expansile, radiolucent and multilocular in nature. It can however be unilocular and associated with impacted teeth resembling a dentigerous cyst (4-6). The latter are known to be less aggressive than the multilocular solid lesions. Three clinical types of ameloblastoma are described, the solid type (radiographically multilocular), the cystic (radiographically unilocular and usually associated with an impacted tooth) and peripheral type (soft tissue usually gingival ameloblastoma) (4-6).
Ameloblastoma, if not treated, can reach very large sizes with facial disfiguring. It loosens, displaces and resorbs adjacent teeth. With the exception of jaw expansion, it is usually asymptomatic unless infected where it can be mildly painful. Parasthesia, anesthesia is extremely rare, unless they are very large in size. Also, ameloblastoma tends to expand rather than perforate the cortical bone. If the later occurs with extension into the adjacent soft tissue, it would have a higher tendency for recurrence and therefore would have a worse prognosis than those completely encased by bone (4-6).
The solid type is treated with complete surgical removal with clean margins through resection or en bloc. Thorough curettage is recommended for the unicystic type and conservative removal for the peripheral type. Resected jaws may require secondary reconstruction (7). All three types have an overall good prognosis. The histology of this case is not supportive of an ameloblastoma.
Congratulations! You are correct
Ghost cell odontogenic tumor (GCOT) is a rare neoplasm of tooth origin (8-9). It is believed to be the end spectrum of a cyst/neoplasm entity known as calcifying odontogenic cyst (COC) which constitutes around 1% of all odontogenic cysts (8-9). Praetorius et al (8) were the first to classify COC into cystic and neoplastic (solid) types, referring to the cystic type of COC as Type 1 and the solid type as Type 2. They further classified the cystic type into subtypes A, B and C: A denoting a simple cyst, B an odontoma-producing cyst, and C a cyst with ameloblastomatous proliferating. The solid type was called dentinogenic ghost cell tumor because of its tendency to produce dentinoid hard material. The nomenclature for the solid type has evolved over time and today this entity is known by a variety of names, including GCOT (8-10).
COC and GCOT vary in their age, location and sex predilection. COC tends to occur around the third decade, with a patient age range of 7-82 years (9-10). It occurs equally in the maxilla and mandible, usually anterior to the first permanent molar, though it has a predilection for occurrence in the maxilla in the younger age range. It occurs equally in males and females (9-10). GCOT, however, favors the mandible over the maxilla, usually anterior to the first permanent molar but more commonly in males over fifty years of age (10). The behavior of GCOT is more persistent than that of its cystic counterpart. It tends to recur more often, and with multiple recurrences, it may transform into a malignant neoplasm (10-12). It is also important to mention that both COC and GCOT may occur in bone (more commonly) or in soft tissue (in the gingiva without a bony component, also known as peripheral COC or peripheral GCOT (8-10)).; The peripheral counterpart of both lesions is less aggressive than the intra-osseous type (9).
Histologically, GCOT ranges from ameloblastoma-like epithelial proliferation including a palisaded and polarized basal cell layer with stellate-reticulum-like suprabasilar proliferation intermixed with clusters of ghost cells. The more aggressive epithelial features, with increased mitotic activity and hyperchromatic nuclei and nuclear pleomorphism, are described in recurring types as well as in those transforming to malignant and invasive neoplasms (11-12). Ghost cells vary in presentation from abundant to sparse. In our case, they were present in the original black but very sparse in the second recurrence (8-12).
Radiographically, COCs tend to be well defined radiolucencies with occasional small radiopacities. They can be present at the apex, between teeth, or associated with impacted teeth. GCOT can also be well defined with a corticated border, as is the case with this patient, in whom all three occurrences showed clearly defined borders (8-12).
Clinically, both COC and GCOT can expand the jaws and extend into the surrounding soft tissues and even the maxillary sinus. They can also resorb and displace teeth. GCOT can grow to as large as 10cm in diameter. Treatment ranges from thorough curettage to resection. The latter is suggested for the recurring and more aggressively behaving lesions. In this patient, the lesion was thoroughly curetted and treated with Carnoy’s solution.
As mentioned above, GCOTs have sometimes been described as eventually invading the surrounding tissue and behaving in a more malignant manner—particularly the recurring types (11-12). These lesions are rare and are treated with resection with clean surgical margins. Recurrence and local invasion is characteristic of this lesion, but not distant metastasis. The latter is rarely described.
References
- Shear M. Odontogenic keratocysts: natural history and immunohistochemistry. Oral Maxillofacial Surg Clin N Am. 2003; 15: 347-362.
- Oda D, Rivera V et al. Odontogenic keratocyst: the northwestern USA experience. J Contemp Dent Pract. 2000 Feb 15; 1(2): 60-74.
- Zachariades N, Papanicolaou S, Triantafyllou D. Odontogenic keratocysts: Review of the literature and report of sixteen cases. J Oral Maxillofac Surg. 1985; 43: 177-182.
- Reichart PA, Philipsen HP, Sonner S. Ameloblastoma: biological profile of 3677 cases. Eur J Cancer B Oral Oncol 1995;31B:86–99.
- Adekeye EO, McLavery K. Recurrent ameloblastoma of the maxillofacial region. Clinical features and treatment. J Maxillofac Surg 1986;14:153-157.
- Gardner DG. Some current concepts on the pathology of ameloblastomas. J Oral Maxillofac Surg 1996;82:660-669.
- Omandi BI, Guthua SW, Awange DO et al. Maxillary obturator prosthesis rehabilitation following maxillectomy for ameloblastoma: case series of five patients. Int J Prosthodont. 2004;17:464-468.
- Praetorius F, Hjorting-Hansen E, Gorlin RJ, Vickers RA. Calcifying odontogenic cyst: range, variations and neoplastic potential. Acta Odonotol Scand 1981;39:227-240.
- Gorlin RJ, Pindborg JJ, Clausen FP, Vickers RA. The calcifying odontogenic cyst: a possible analogue of the cutaneous calcifying epithelioma of Malherbe. Oral Surg Oral Med Oral Pathol 1962;15:1235-1243.
- Hong SP, Ellis GL, Hartman KS. Calcifying odontogenic cyst: a review of ninety-nine cases with reevaluation of their nature as cysts or neoplasms, the nature of ghost cells, and subclassification. Oral Surg Oral Med Oral Pathol 1991;72:56-64.
- Folpe AL, Tsue T, Rogerson L, Weymuller E, Oda D, True LD. Odontogenic ghost cell carcinoma: a case report with immunohistochemical and ultrastructural characterization. Oral Pathol Med 1998;27:185-189.
- Mc Coy BP, O Carroll MK, Hall JM. Carcinoma arising in a dentinogenic ghost cell tumor. Oral Surg Oral Med Oral Pathol 1992;74:371-378.
- Gardner DG. Residual cysts. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1997 Aug;84(2):114-115.
- Dimitroulis G, Curtin J. Massive residual dental cyst: case report.
Aust Dent J. 1998 Aug;43(4):234-237.
Sorry! you are incorrect
The unilocular and corticated radiolucency in an area of extracted teeth should include residual periapical cyst on the differential diagnosis. Periapical cyst is the most common odontogenic cyst and is of inflammatory origin (13-14). It arises from the odontogenic epithelium, such as the epithelial rests of Malassez, in response to an inflammatory process caused by tooth necrosis which in turn is caused by extensive caries or tooth fracture (13-14). They are typically in close contact with the affected tooth: usually at the apical portion, but sometimes laterally situated.
The preferred treatment is endodontic, although teeth are sometimes extracted. Extraction should be followed by curettage of the cystic structure; if the tooth is extracted and the cystic structure, granuloma or abscess is left untreated, the area will not completely heal, leaving behind the bony lesion as the residual periapical cyst or granuloma (13-14). Radiographically, it presents like any other jaw cyst as a unilocular radiolucency with a corticated border. It can be asymptomatic or it can be expansile. Histologically, it is similar to the conventional periapical cysts. The radiographic features in this case can be interpreted as residual cyst, but the histology is not consistent with this diagnosis. The histology of this case is not supportive of a periapical residual cyst.