Large Multilocular, Expansile Radiolucency, Right Posterior Mandible
Can you make the correct diagnosis?
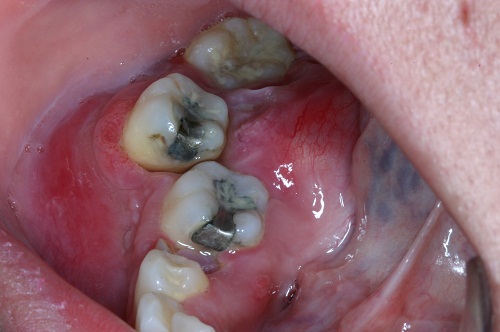
This is a 26-year-old Hispanic female who presented to her dentist with mild pain and very large swelling on the right posterior mandible.
Sorry! you are incorrect
The location of posterior mandible, the ballooning expansion, the multilocular radiolucency, the age of the patient and may be even the gender are all supportive of the diagnosis of aneurysmal bone cyst which should be kept high on the differential diagnosis list. The histology however, is not supportive of ABC.
Aneurysmal bone cyst is a disease of the young, usually occurs before the age 20. It is not common in the jaws. There is a slight female predominance and it is more common in the mandible. The etiology of ABC is unknown but is believed to be due to high-pressure hemorrhage while central giant cell granuloma (CGCG) is due to low-pressure hemorrhage. Clinical Features include pain and swelling. Radiographically, ABC presents as multilocular or honeycombed expansile radiolucency with thinning leading to ballooning or ‘blow out’ distention of bone which is highly suggestive of ABC. Histopathology: ABC is similar to CGCG but with sinusoidal blood spaces. Treatment consists of thorough curettage of the lesion.
Congratulations! You are correct
The location of posterior mandible, the expansion, the multilocular radiolucency are the classic clinical and radiographic presentation of ameloblastoma. The age of the patient however is a little on the young side. The histology is positive for ameloblastoma.
About 85% of ameloblastomas occur in the posterior mandible; most of these occur in the molar-ramus area, and some occur in the anterior mandible. About 15% occur in the maxilla, the vast majority of these in the posterior maxilla, in patients around the age of 60 and tend to have a worse prognosis than those of the mandible.
Ameloblastoma is characteristically expansile, radiolucent and multilocular in nature. However, it can be unilocular and associated with impacted teeth resembling a dentigerous cyst. The latter types of ameloblastoma are known to be less aggressive than the multilocular solid lesions. Three clinical types of ameloblastoma are described: the solid type (radiographically multilocular), the cystic type (radiographically unilocular and usually associated with an impacted tooth), and the peripheral type (soft tissue, usually gingival ameloblastoma). The present case is of the solid type and is multilocular in appearance. Ameloblastoma, if not treated, can reach very large sizes, causing facial disfigurement. It loosens, displaces and resorbs adjacent teeth. With the exception of jaw expansion, it is usually asymptomatic unless infected, in which case it can be mildly painful. Parasthesia and anesthesia are extremely rare, unless the lesion is very large in size. Also, ameloblastoma tends to expand rather than perforate the cortical bone; if the latter occurs with extension into the adjacent soft tissue, it has a higher tendency for recurrence and therefore a worse prognosis than cases in which the ameloblastoma is completely encased by bone. As mentioned above, three clinical types of ameloblastomas are described, the solid type being the most common. The solid type is treated with complete surgical removal with clean margins through resection or en bloc. Curettage is not recommended for the solid type because it is associated with a higher recurrence rate. Ameloblastoma has a good prognosis overall but is known to have a high recurrence rate, particularly in the posterior maxilla, from inadequate surgery (tumor extending to the surgical margins). Long-term follow-up is required. Recurrence is related to the treatment modality.
References
- Reichart PA, Philipsen HP. Et al. Ameloblastoma: biological profile of 3677 cases. Eur J Cancer B Oral Oncol 1995;31B:86–99.
- Adekeye EO, McLavery K. Recurrent ameloblastoma of the maxillofacial region. Clinical features and treatment. J Maxillofac Surg 1986;14:153-157.
- Gardner DG. Some current concepts on the pathology of ameloblastomas. J Oral Maxillofac Surg 1996;82:660-669.
- Parashari UC, Khanduri S, Upadhyay D, Bhadury S, Singhal S. Radiologic and pathologic correlation of aneurysmal bone cysts at unusual sites. J Cancer Res Ther. 2012;8(1):103-5.
- Galal Omami, BDS, MSc, Dennis Gianoli, Alan Lurie. Enormous aneurysmal bone cyst of the mandible: case report and radiologic-pathologic correlation. Oral Surgery, Oral Medicine, Oral Pathology, 2012.
- Sharma R, Marwah N. Odontogenic myxoma of the mandible: a case report. Indian J Pathol Microbiol. 2003;46:84-86.
- Simon EN, Merkx MA. Odontogenic myxoma: a clinicopathological study of 33 cases. Int J Oral Maxillofac Surg. 2004;33:333-337.
- Moshiri, S., Oda, D.et al. Odontogenic myxoma: a clinical and immunohistochemical study. J Oral Path 1992;21:401-403.
Sorry! you are incorrect
The location, the obvious expansion, the multilocular radiolucency, the age of this patient are all supportive of odontogenic myxoma. The histology is not supportive of odontogenic myxoma.
Odontogenic myxoma should not be mistaken for soft tissue myxoma, which is a relatively common lesion of the soft tissue. It is rare in the mouth; it occurs more commonly in areas such as the heart. When it does occur in the mouth, odontogenic myxoma occurs in the jaw bones, usually in the tooth-bearing areas of the jaw. It is an uncommon, benign, but locally aggressive neoplasm. Nearly all cases so far have been described in the jaw bones. Therefore, it is of tooth origin, and is believed to be from the mesenchymal portion of a tooth germ, most likely of the dental papilla. It has the potential for extensive bony destruction and extension into the surrounding structures. It is less common than odontomas and ameloblastomas, constituting around 17% of all odontogenic tumors. For that reason, a pathologist who is not familiar with the histology of a tooth germ can mistake a myxoid dental follicle for an odontogenic myxoma. Almost 75% of odontogenic myxomas occur in patients around 23-30 years of age with a slight female predilection (1:1.5 male-to-female ratio). It rarely occurs in patients over 50 or under 10 years of age. It occurs almost equally in the maxilla and mandible with a slight predilection for the posterior mandible. A few cases are described in the ramus and condyle, non-tooth bearing areas. Odontogenic myxoma is slow-growing, persistent and destructive. Most cases are expansile and can displace and resorb teeth. In the maxilla, they usually invade the maxillary sinuses and, in rare cases, cross the midline to the opposing sinus. Radiographically, the majority present as expansile and multilocular, though some are unilocular with or without scalloped borders, and rare cases present with a diffuse and mottled appearance which can be mistaken for a malignant neoplasm. Grossly, this lesion is gelatinous in nature, making curettage alone difficult; the more fibrotic odontogenic myxomas (also known as odontogenic myxofibroma or fibromyxoma) have more body and are easier to curette. Histologically, it is made up of loose and delicate fibrous connective tissue. The fibroblasts are stellate and are suspended on a delicate network of collagen fibrils.
The treatment of choice is surgical excision ranging from segmental resection with clear bony margins of up 1.5cm to prevent recurrence of the neoplasm. Curettage with and without cauterization is used for treatment, but is associated with a high recurrence rate. Reconstruction can be immediate or delayed, and can include an autologous bone graft from the anterior or posterior iliac crest. Fibula-free vascular osteocutaneous bone graft is another reconstructive modality, as is distraction osteogenesis. The patient is usually hospitalized for a short period of time following resection and placed on intravenous antibiotics while in the hospital to prevent secondary infection of the surgical site, especially if immediate bone grafting is accomplished. Immediate postoperative follow up is weekly for approximately one month, then monthly for the next five months and twice a year for the next five years.