Multiple Pigmented Lesions on the Gingiva
Can you make the correct diagnosis?
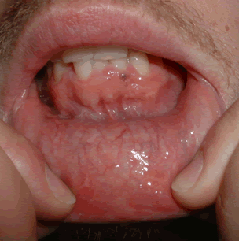
This is a 26-year-old white male who was referred to the Department of Oral and Maxillofacial Surgery at the University of Washington for evaluation of multiple pigmented lesions on the left anterior mandibular labial gingiva.
Sorry! you are incorrect
Pigmented lesions of the mouth can be caused by endogenous (melanin, blood, hemosiderin) or exogenous (metal, carbon) particles. The exogenous pigment is best exemplified by amalgam tattoo; the endogenous, by melanin producing lesions which include racial pigmentation, post inflammatory pigmentation, smoker’s melanosis, melanotic macules, pigmented nevi and malignant melanoma.
Melanotic macules present as oval-shaped brown and flat lesions less than 5 mm in diameter (1) on the lower lip, and are called labial melanotic macules. In 85% of cases, labial melanotic macules are located close to the midline. They can also occur within the oral cavity, where they are called oral melanotic macules. The latter most commonly occur on the gingiva, followed by the buccal mucosa. Oral melanotic macules can occur at any age, with a 2:1 prevalence in females. They usually present as a solitary lesion, but multiples have been described. When multiple macules are identified, it is necessary to rule out other diseases such as Addison’s disease and Peutz Jeghers syndrome.
Histologically, in focal areas, the basal cell layer actively produces and releases melanin (1). These lesions, especially those that occur rapidly, are usually excised to rule out malignant melanoma. The clinical presentation in this case can be suggestive of oral melanotic macules; the histology, however, does not support this diagnosis.
Congratulations! You are correct
Malignant melanoma (MM), whether on the skin or in the oral cavity, has the same cell of origin: the melanocyte. Despite the common cell origin, these lesions have different clinical behavior. The mucosal melanomas are very rare and are more aggressive in behavior than those of the skin. They usually affect adults with an average age of 55; occasionally, affects patients under 30 years of age which is the case in our patient (7). Skin MM used to have a poor prognosis but that has changed significantly; in 1950, the 5-year survival rate for skin MM was 50%, while today it is 90% (6, 8). However, mucosal melanomas still carry a dismal 5-year survival rate of not higher than 38% (7). Skin MM, like mucosal melanoma, occurs mostly in adults around 50 years of age and rarely affects children.
Cutaneous malignant melanoma is the third most common skin epithelial malignancy (following basal cell carcinoma and squamous cell carcinoma) but by far the most aggressive of the three. In the United States alone, over 50,000 cases are diagnosed annually with about 8,000 dying of the disease each year (6). It has been on the increase since 1960 and has recently plateaued. In the 1960s, 1 in 600 individuals were expected to develop MM in their lifetime, compared with 1 in 71 in 2001. Australia has the highest number of skin MMs: a number that has been doubling every 10 years (9). The etiology of MM and its rate of increase are complex and are beyond the scope of this discussion. However, it is important to mention that multiple factors seem to play a role the development of the MM and its progression. The most important factor is exposure to ultraviolet light which is logical on the skin but does not explain the oral, nasal, and other non-sun exposed areas that develop MM. It has been suggested that the age of the individual at the time of exposure is important (6-10): it is suggested that sunburns, especially blistering sunburns in childhood, increase the risk of developing MM in adulthood. Genetics play a significant role in MM, especially in patients born in families with a history of this disease. For instance, patients from families with a history of dysplastic mole syndrome or patients who have a first relative with malignant melanoma are at a higher risk of developing the disease (6-10). 70% of cutaneous MMs occur in a preexisting pigmented nevus.
Pigmented nevi are common and have a one in a million chance of transformation to MM. This does not necessitate surgical removal, but rather suggests that practitioners should be attentive to alterations in nevi such as changes in color, shape and size; ulceration and/or bleeding; inflammation; pain; and a diameter change of greater than 7mm. These are the clinical criteria used in England (10) to assess clinical presentation of MM. Bleeding and ulceration of a pigmented nevus should be viewed seriously, and the lesion should be soon biopsied or completely removed and submitted for microscopic evaluation.
The clinical features of MM in the United States follow the ABCDE rule: asymmetry, borders, color, diameter and enlargement. A pigmented lesion that is asymmetrical with irregular borders (especially borders with notching), uneven coloration (a range of tan to dark brown as is the case with our patient), larger than 6 mm in diameter, and continues to enlarge showed be viewed with suspicion and biopsied immediately.
The oral mucosa is rarely affected by MM and for that reason, the etiology of this disease in the mouth is still unclear. Local melanosis and tobacco use have been implicated. Race also appears to play a role; for example, 7.5% of all reported oral melanomas affect those of Japanese descent and 10% affect those of Ugandan descent, compared with less than 1% of the Caucasians.
Cutaneous MM, however, occurs at a much higher rate in Caucasians than in those with brown or black skin, with a rate of 1:83 in whites compared to 1:1176 in dark-skinned individuals (8). Mucosal melanomas are extremely rare compared to cutaneous melanomas; they constitute less than 1% of all MMs. For that reason, it is always prudent to first rule out metastatic MM to the oral cavity from the skin when a biopsy of an oral pigmented lesion confirms the diagnosis of MM. 80% of oral MMs affect the palate and the maxillary gingiva. Mandibular gingiva can be affected, but rarely. Cutaneous MMs occur mostly on the interscapular area of the back and back of the legs (6). 25% occur in the head and neck area, including the face, eyes, nose and mouth (7). In the oral cavity, they present as flat, multiple, graded or uneven coloration, irregular borders and sometimes ulcerated. They are usually asymptomatic; pain is described only rarely.
Histologically, MMs demonstrate radial and vertical growth patterns. Vertical is important because it plays an important role in predicting prognosis; for that reason, the depth of invasion is always reported. Depth of invasion in skin MMs is fully established following Clark and Breslow’s staging according to depth (6). Obviously, the deeper the tumor invasion, the higher the microscopic staging and the worse the clinical behavior. Determining prognosis is not simple, though; other factors play a role in worsening the prognosis, such as the location, age and gender of the patient.
Treatment
Surgery is the treatment of choice treatment for MM of the oral cavity. Under general anesthesia, the pigmented lesions were widely excised with clean surgical margins (Fig 2). Two surgeries were performed to achieve complete clean margins. In order to achieve clean margins, the pigmented lesions, the surrounding normal gingiva, some normal mucosa of the left anterior mandibular vestibule, and multiple vital and healthy teeth had to be removed. The surgical site was adapted and grafted with AlloDerm. A Copack dressing was applied and allowed to set. On follow-up visits, the patient reported minimal discomfort; subsequent follow-up visits showed complete healing. A removable anterior prosthesis was fabricated by his dentist. The patient is kept on follow-up visits of three-month intervals. Radiation and chemotherapy may be used in advanced cases.
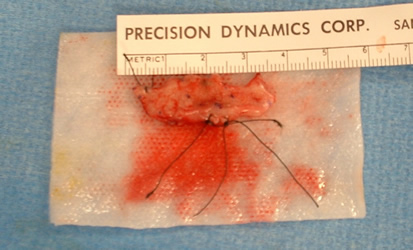
Figure 2. This is the entire soft tissue surgical specimen from the first surgery. It is placed flat and labeled with sutures for margin identification. This represents the soft tissue portion of the surgical specimen. Teeth and bone were also removed but are not shown.
References:
- Cicek Y, Ertas U. The normal and pathological pigmentation of oral mucous membrane: a review. J Contemp Dent Pract. 2003; 4: 76-86.
- Shah, G, Alster, TS. Treatment of an amalgam tattoo with a Q-switched alexandrite (755 nm) laser. Dermatol Surg 2002; 28: 1180-1181.
- Sarswathi TR, Kumar SN et al. Oral melanin pigmentation in smoked and smokeless tobacco users in India. Indian J Dent Res. 2003; 14: 101-106.
- Braithwaite, SS, Clasen, RA et al. Silent corticotroph adenoma: case report and literature review. Endocr Pract. 1997; 3: 297-301.
- Erickson QL, Faleski EJ et al. Addison’s disease: the potentially life-threatening tan. Cutis. 2000 Jul;66(1):72-74.
- Langley, RM, Fitzpatrick, TB et al. Cutaneous melanoma. Quality Medical Publishing inc., St Lois, MO. 1998.
- Rapidis, AD, Apostolidis, C et al. Primary malignant melanoma of the oral mucosa. J Oral Maxillofac Surg. 2003; 61: 1132-1139.
- Rigel, DS, Friedman, RJ et al. The incidence of malignant Melanoma in the United States: issue as we approach the 21st century. Am J Acad Dermatol 1996; 34: 839-847.
- Whiteman, DC, Valery, P et al. Risk factors for childhood melanoma in Queensland, Australia. Int J Cancer 1997; 70: 26-31.
- Healsmith, MF, Bourke, JF et al. An evaluation of the revised seven-point check list for the early diagnosis of cutaneous malignant melanoma. Br J Dermatol 1994; 130: 48-50.
Sorry! you are incorrect
Amalgam tattoo is the most common pigmented lesion in the oral cavity. It is an example of a local deposition of exogenous metallic material from a dental filling, usually the silver metal found in amalgam (2). It is deposited on the collagen fibers in connective tissue, around small blood vessels, in the basement membrane, between muscle fibers, and in other tissues present in the area. Amalgam tattoo occurs as a result of metal implantation in lacerated mucosa during a dental filling or the removal of an old amalgam filling. They can also be the result of amalgam falling in the dental socket following an extraction or in area of an apicoectomy sealing. It is like any cutaneous tattoo, it leads to a permanent coloration of the mucosa, usually flat and grey to bluish-black in color. Occasionally, they can be exophytic or nodular; this is usually a result of foreign body reaction to the metal. The margins can be irregular or well-defined. They can enlarge and give the impression of lateral spread; this happens during the first months of implantation, but once the area heals, the lateral spread ceases. They most commonly occur on the alveolar mucosa, buccal mucosa, and gingiva (2), but have been described on the palate, floor of mouth and tongue. They can be viewed radiographically, especially within a socket if present in clusters. Histologically, they present as granular black material deposited on the surrounding thin collagen fibrils. Sometimes, foreign body reaction with foreign-body-type giant cells, chronic inflammation and scarring are present. Sometimes, an incisional biopsy is recommended to eliminate the possibility of other, more serious diseases; otherwise, there is no need for treatment. The clinical presentation and the histology of this case are not supportive of this diagnosis.
Sorry! you are incorrect
In the United States alone, there are over 65 million tobacco users. 56 million are cigarette smokers and 12 million use smokeless tobacco. There are also 40 million ex-users. Heavy cigarette, cigar and pipe smokers stimulate the melanocytes to actively produce melanin in the area where most smoke comes in contact with the mucosa. The melanin production is believed to be a protective effect against tobacco elements, such as nicotine, which is known to bind melanin. It is the same phenomenon as tanning of the skin when exposed to the ultraviolet light. Smoking-related melanin production produces a flat light brown pigment, usually diffuse, present on the facial anterior gingiva (3). It occurs on the mandible more often than the maxilla in heavy cigarette smokers. In addition, it tends to occur on the commissure and buccal mucosa in heavy pipe smokers and on the hard palate in reverse smokers. The histology consists mostly of excessive melanin production arranged in small clusters in the superficial lamina propria. Neither the clinical presentation nor the histology is supportive of this diagnosis.
Sorry! you are incorrect
Addison’s disease is an endocrine disorder affecting all ages and both sexes equally. It is characterized by muscle weakness, fatigability, nausea, vomiting, anorexia, weight loss, hypotension, and sometimes salt craving (4-5). It can also present with skin and mucosal darkening referred to as “bronzing,” which may affect the mouth at an early stage of the disease in the form of multiple flat and pigmented lesions. Addison’s disease occurs as a result of low cortisol and sometimes of low aldosterone, both of which are produced by the adrenal glands. The symptoms occur gradually because the disease does not occur until 90% of the functioning cells in the adrenal cortex are lost. Two types are described: primary and secondary. Primary Addison’s is direct loss of adrenal function (5), while secondary Addison’s is a result of pituitary gland dysfunction leading to decreased production of ACTH hormone (4). The main etiology of primary Addison’s is autoimmune destruction of adrenal cells (5); other factors have been proposed such as infection, tumor metastasis, and hemorrhage. Cortisol is essential in balancing a number of systems in the body, including the cardiovascular system, the immune system, metabolic activity, and several other vital activities that maintain a healthy and functioning body. Aldosterone helps control water and salt balance as well as blood pressure. Cortisol is released in response to the pituitary producing ACTH; therefore, low cortisol production by the adrenal gland in primary Addison’s disease translates into high serum levels of ACTH, which can prove to be a good test for determining a diagnosis of Addison’s disease. Additionally, high ACTH is associated with stimulating a melanocyte-stimulating hormone which leads to excessive production of melanin, thereby bronzing the skin and pigmenting the oral mucosa, scars, skin folds and skin in pressure areas. In the secondary type, the ACTH level is low because of a disease that this preventing the pituitary to release the hormone (4). Low ACTH inhibits the adrenal gland from production of cortisol. The clinical symptoms related to low cortisol are the same as those of the primary Addison’s. Dentists may be the first to discover Addison’s if patients complain of multiple brown pigments in the mouth that occurred recently in the absence of clinical history such as smoking and ingestion of drugs such as birth control pills. The best test for Addison’s is plasma ACTH level, which is high in the primary type and low in the secondary type. Once the diagnosis is established, steroid supplements are the treatment of choice for the primary type. Secondary Addison’s is treated according to the cause of the pituitary dysfunction. Neither the clinical presentation nor the histology of this case are supportive of Addison’s disease.