Single deep ulcer, lateral tongue
Can you make the correct diagnosis?
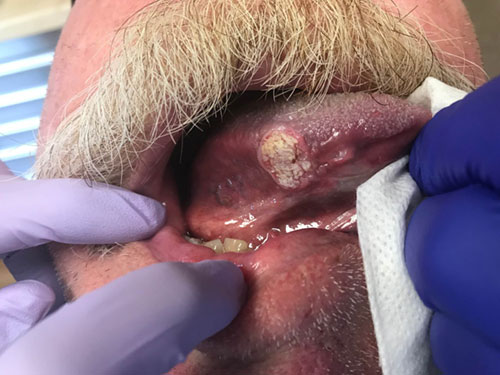
This is a 65-year old white male who was referred by his dentist to an oral surgeon for the evaluation of a single deep ulcer on the right lateral/ventral border of tongue (Figure 1).
Sorry, you are incorrect!
A single deep ulcer on the lateral border of tongue should make one think of traumatic ulcer. The duration of being present for several months when combined with age, gender and history of chronic and heavy tobacco use are all features arguing against traumatic ulcer. The histology is not that of traumatic ulcer.
Traumatic ulcers of the oral cavity can occur at any age, more commonly on the anterior and lateral tongue. The most common cause is accidental sharp bite of the tongue but other sources of trauma can be implicated such as a sharp tooth, an ill-fitting denture or a sharp denture edge or a broken filling. Chronic single ulcers in general and especially those associated with dentures may have rolled borders because of the scarring that is associated with healing. The rolled border-type ulcers are frequently mistaken for squamous cell carcinoma (SCC). Elimination of the source of trauma should help healing of the ulcer within two to three weeks. Sometimes, however, the source of trauma is difficult to identify, and even when identified and removed, the ulcers do not heal and may remain persistent for months. A biopsy of a non-healing ulcer is warranted for two reasons: to rule out malignancy, such as squamous cell carcinoma, and to stimulate healing.
Sorry, you are incorrect!
A single deep ulcer on the lateral border tongue present for several months in a male are all characteristics consistent with TUGSE. It occurs at all ages, so the age of this patient fits the older age spectrum. The site is also consistent but TUGSE tends to occur more posterior and dorsal of tongue. The history of heavy chronic tobacco use argues against TUGSE. The histology is not that of TUGSE.
In the past, TUGSE was also called “traumatic granuloma”, “eosinophilic ulcer” and “eosinophilic granuloma” of the tongue (which is not related to eosinophilic granuloma of the bone as in Langerhans cell Histiocytosis). Over 60% of TUGSE cases occur on the posterior lateral and dorsal tongue with a history of trauma. They are rarely reported in other oral sites i.e. lips and buccal mucosa. It is usually an isolated single lesion and usually as deep single ulcer but in about 7% of cases TUGSE can present in multiple and in form of an exophytic lesion. TUGSE may affect patients of all ages, including infants (Riga-Fede disease occurs during the first year of life as a result of chronic trauma in the sublingual area to baby’s lower incisors during breastfeeding). TUGSE tends to occur more commonly in males than females. Histologically, these ulcers are deep lesions involving the underlying muscle, which may explain the process of slow healing and the tissue eosinophilia. Healing may take up to eight weeks; sometimes more. Clinically, TUGSE tend to be deep ulcers with rolled borders that can clinically be mistaken for SCC.
Congratulations, you are correct!
The nonhealing single deep ulcer of several months duration, the history of around fifty years of heavy cigarette smoking, the age, gender and site of lateral border of tongue are all consistent with the clinical presentation of tobacco-associated oral squamous cell carcinoma (SCC). The histology is that of SCC.
Tobacco-associated Oral SCC is an aggressive neoplasm that currently ranks as the fifth most common malignant neoplasm worldwide and accounts for an estimated 75% of oral malignancies. Oral SCC occurs predominantly in males over the age of 40 years, with an observed male to female ratio of 2:1 generally and 1.4:1 in the USA. Excluding the outer lip, the most common sites (in decreasing order) are ventral and lateral surfaces of tongue (25-50%), floor of mouth (15%), gingiva (12%) and soft palate (9%). The buccal mucosa and retromolar pad areas (3%) have a relatively low incidence of occurrence unless the patient is a chronic smokeless tobacco user. Oral SCC varies in presentation from deceptively innocent-looking to obviously malig¬nant. It may present as a non-healing ulcer, or as red, white or mixed red-and-white lesions. Characteristic signs of oral SCC are non-healing ulcer, ulcer with rolled borders, fungation, fixation and induration.
Tongue SCC is usually found on the lateral and ventral surfaces. The dorsal surface of tongue is very rarely involved. Usually, SCC of the posterior tongue is more aggressive than that of the anterior tongue. Around 78% of base of tongue SCCs show early metastasis, especially to regional lymph nodes; in this group about 69% of tongue carci-nomas show evidence of metastasis at admission. Oral SCC is most commonly associated with chemically induced mutagenesis, specifically tobacco and alcohol use. Tobacco use is described in over 75% of oral SCC patients. Tobacco and alcohol have been shown to act synergistically in the development of oral SCC.
Sorry, you are incorrect!
The oral cavity is a site where a number of acute and chronic infectious diseases occur as a local disease or as a manifestation of a systemic disease. They include diseases of viral, fungal and bacterial origin. They usually present in multiple or in a diffuse manner ranging from ulcers to small and nodular lesions to verrucoid lesions. Rarely would infectious diseases present as a single ulcer with rolled border, simulating an OSCC. Those include ulceration induced by mycobacterium tuberculosis, deep fungal infection such as blastomycosis and histoplasmosis and chancre of primary syphilis. Oral manifestations of tuberculosis and histoplasmosis are unusual without lung involvement and a disseminated disease and occur more in immune compromised patients. Gingiva and the mandibular vestibule are more common locations but tongue can occasionally be affected. Chancre can occur in any location, including the tongue, lips and hard palate. As mentioned previously, single oral ulcers of infectious disease origin are a rare occurrence and should be kept low on the differential diagnosis list. The histology in this case was not supportive of an infectious process.