Generalized and persistent oral surface ulcerations
Can you make the correct diagnosis?
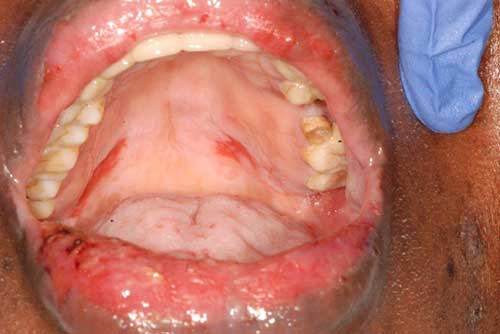
This is a 44-year-old black female who presented with generalized oral ulcers since September 2016.
Differential Diagnosis
The differential diagnosis for extensive, recurrent and persistent oral ulcers is complicated and includes a wide spectrum of diseases including:
- Infectious diseases especially those in herpes simplex virus family
- Immune mediated diseases including lichen planus/lichenoid mucositis; mucous membrane pemphigoid; pemphigus vulgaris and others.
- Drug induced in general there are many medication that can cause oral ulcers including chemotherapy type of medications but as common as NSAIDS
- Erythema multiforme (EM) family (major, minor) which can be the result of previous infection especially with herpes simples family; can be in relation with mycoplasma pneumonia infection or be drug induced
- Stevens Johnson syndrome (SJS) and toxic epidermal necrolysis (TEN) (which are currently considered separated from EM) & are more likely drug induced
- Hypersensitivity reactions to restorative dental material or others
- Nutritional deficiency especially with vitamin B and iron deficiency
- Graft vs. host disease (GVHD) in response to allogenic bone marrow transplant
- Oral manifestation and systemic diseases such as Behcet’s, cyclic neutropenia; PFAPA and paraneoplastic pemphigus
This is an extensive list to work through and a lot of information is needed to reach an applied differential diagnosis. The patient did not have any malignant neoplasms and had no history of allogeneic bone marrow transplant ruling out # 8. There was no nutritional deficiency when the condition started ruling out #7 and had no history of any hypersensitivity documented to oral restorative dental material or any systemic antigen ruling out #6. Lack of fever combined with over six months persistent severe ulcers in an otherwise healthy individual (no history of immune compromised conditions) rules out #1 especially that of blistering infectious viral diseases in the herpes family. Based on the history of multisystem involvement i.e. mouth, eyes, skin, genitals, we have to include EM, SJS, TEN; immune mediated diseases and oral manifestation of systemic diseases.
Sorry, you are incorrect!
Erythema multiforme (EM) is an acute, immune-mediated condition divided into major and minor representing a wide range of erythematous mucocutaneous lesions progressing to vesicles/bullae and ulcers. In this case, EM major will apply since both skin and mucosal lesions are present. EM minor tends to be cutaneous lesions without mucosal lesions. Currently EM major is separated from Stevens Johnson Syndrome (SJS) mainly where etiology applies. EM major can appear subsequent to a viral infection especially herpes virus. It can be associated with mycoplasma pneumonia infection or be drug induced similar to SJS. This is a self-limited condition lasting 2-6 weeks and occurs more in males around 20-40 years of age and more on the lips and anterior tongue. EM can occasionally recur and last for a year. Clinically EM major is high on the differential diagnosis but the diseases did not self-limit in six weeks; the patient did not have any viral or mycoplasma infections prior to the ulcers and was not taking and prescription or over the counter medications prior to the oral ulcers. The histology is not consistent with EM.
Sorry, you are incorrect!
Both Stevens-Johnson syndrome (SJS) and toxic epidermal necrolysis (TEN) are considered to be a spectrum of the same diseases representing severe mucocutaneous lesions ranging from blisters to severe surface ulceration and sloughing as is the case in this patient. The main etiology in both conditions is the ingestion of certain medications such as sulfa drugs and others like nonsteroidal anti-inflammatory drugs (NSAID). This disease occurs more commonly in females and at any age ranging from childhood to old age. It is also known to affect the skin and mucosa including the oral cavity, eyes and genitals. In the mouth, it can affect all areas but is more common on the lips and tongue. This condition tends to usually self-limit. This patient had persistent ulcers for over six months. The age, gender and the clinical presentation of ulcers on the skin and mucosa is consistent with SJS and TEN but like EM major, this patient was not taking any medications or over the counter drugs prior to the oral ulcers. The histology is not consistent with this SJS or TEN.
Congratulations, you are correct!
There are several chronic and persistent immune mediated diseases that can affect the oral mucosa, other mucosa and skin with clinical sign and symptoms as seen in this patient. Among them are erosive lichen planus; lichenoid mucositis; mucous membrane pemphigoid (MMP) and pemphigus vulgaris (PV).
Severe form of erosive oral lichen planus (LP) or even generalized lichenoid mucositis tends to present more commonly bilaterally and symmetrically on the buccal mucosa and vestibule. Erosive LP usually has some degree of striae of Wickham. The clinical presentation in this case is unlikely to be erosive LP or lichenoid mucositis but they should be placed on the differential diagnosis list.
Severe forms of mucous membrane pemphigoid can present with mucocutaneous ulcers. The clinical presentation of oral MMP does not apply in this case since up to 94% of oral MMP cases first present on the gingiva which is unlike this case where the gingiva is spared and the lips, tongue and soft palate are affected. Based on the clinical presentation, MMP stays on the differential diagnosis list but low at this point.
Pemphigus vulgaris is a rare family of serious acantholytic/blistering diseases that have the potential to be life threatening. This is an immune mediated disease where the immune system recognizes certain proteins in the desmosomes to be antigenic and targets them with IgG and C3 antibodies forming a complex that destroys the desmosomes causing breakdown of the spinous layer cells (acantholysis) forming blisters within the epithelium ultimately leading to break down of the epithelium and causing ulceration. This disease affects the skin and mucosa including oral (about 50% of cases), eyes, upper respiratory, genitals and other areas. It is described more in individuals with Jewish, Mediterranean, Indian, and Middle East ancestry. Pemphigus vulgaris occurs more commonly in females 40-60 years of age. In the oral cavity, it is more common on the lips, and soft palate area. The clinical symptoms; the persistence and progression of the disease; the age and gender are all consistent with this disease and so is the histology and the direct immunofluorescence staining.
Sorry, you are incorrect!
There are few systemic diseases that can present with persistent and severe skin and mucosal ulcers, one of which is Crohn’s disease; another is Behcet’s syndrome and yet another is paraneoplastic pemphigus.
Crohn’s disease usually affects under 20 or over 50 years of age. About 8% of these patients present with aphthous-ulcer type of lesions in the mouth (soft palate and vestibules) but also complain of GI symptoms of diarrhea and constipation and pain. It is rare that the oral ulcers would be so severe. Usually skin ulcers and eyes are not described. The age, the lack of GI symptoms and the skin, ocular and mucosal involvement argues against Crohn’s disease. The histology was not consistent with Crohn’s disease.
Behcet’s syndrome is common in Middle East and Far East countries but is not that common in Europe or the US. It is a type of vasculitis affecting a range of organs including skin, mucosa, the GI, nervous system, joints and other organs. Behcet Syndrome patients present with oral ulcers in the mouth indistinguishable from aphthous ulcers, anogenital ulcers and eye lesions. In the more affected countries (Middle and Far East) it is more common young patients 10-40 years of age with equal gender distribution but it tends to be more severe in young males. In the US and Europe, it tends to be more common in females around 20-40 years of age. The age, gender, persistent ulcers of the skin and mucosa are also consistent with Behcet’s but there were no GI symptoms; no neurological or arthritis reported. The histology was not consistent either.
Paraneoplastic pemphigus (PNP) usually presents with severe skin and mucosal ulcers. It is a serious skin and mucosa disease manifesting the host reaction to a visceral malignant neoplasm such as malignant lymphoma; lymphocytic leukemia and other mesenchymal and epithelial malignant neoplasm and non-malignant conditions. This patient did not have any malignant neoplasms to report.