Large Radiolucency, Right Posterior Mandible
Can you make the correct diagnosis?
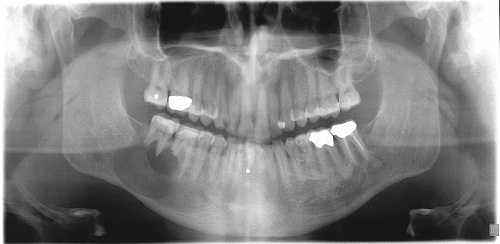
This is a 54-year-old white male who was referred to the Department of Oral Surgery, UW SOD for a swelling in the right mandible involving teeth #s 29-32.
Sorry! you are incorrect
The sharp edge resorption of tooth #31 and the small satellite radiolucency distal to the large radiolucency can indicate aggressive, perhaps even malignant, behavior. Langerhans cell histiocytosis is among the aggressively behaving lesions that should be considered. The age of the patient, however, is not supportive of this condition since LCH tends to occur in children and younger patients. The histology is also not supportive of LCH.
Langerhans cells are dendritic cells of bone-marrow origin. Langerhans cell histiocytosis is generally a disease of children, only rarely affecting adults. The old name for this condition was histiocytosis X, which was classified into eosinophilic granuloma (monostotic and polyostotic), Hand-Schuller-Christian disease, and Letterer-Siwe disease. The first two types (EG and HSC) are less aggressive and are chronic in clinical behavior while the last (LS) is more aggressive and acute in behavior. The currently used classification divides cases into the categories of unifocal, multifocal/unisystem and multifocal/multisystem. This classification also divides patients into low- and high-risk categories: patients with the unifocal and multifocal/unisystem types are considered low risk, while those with the multifocal/multisystem type are high risk. In other words, if the disease affects one organ, whether in one or more sites (i.e. bone, lymph nodes, skin or pituitary gland), it is considered to be a low-risk type; if the disease involves multiple organs such as the lungs, liver, spleen and bone marrow (multifocal and multisystem), it is considered to be a high-risk type. LCH usually presents with pain and swelling but can also be asymptomatic. The bony lesions are usually aggressively lytic, especially those of the mandible. More than 50% of cases affect children under 10 years of age, with a male predilection. Adult LCH most commonly affects the bones, especially the jaws and skull bones in general. LCH of the jaw bone usually presents as either localized severe periodontitis or generalized severe periodontitis, and rarely as localized, well-demarcated radiolucency. Radiographically, the bony lesions are sharply radiolucent and the jaw lesions give the impression of teeth “floating” in space due to the significant bone destruction. LCH can also affect the skin, the lymph nodes, and less commonly the pituitary and lungs.
Langerhans cells are CD1a positive and for that reason, immunohistochemistry staining is very helpful. They are also S-100 and CD45 positive. Langerhans cells can also be comfortably identified by the H & E stain. Treatment includes curettage especially of the jaw lesions. Chemotherapy and low-level radiotherapy have also been effective. The unifocal disease has an overall 95% survival rate, types with two-organ involvement have an overall survival rate of 75%, and the more organs are involved, the less favorable the prognosis.
Congratulations! You are correct
Again, the sharp-edge tooth resorption and the small satellite lesion should make one think of an aggressive, if not an outright malignant, process. Malignant neoplasms such as plasmacytoma should be included in the differential diagnosis of such an aggressively behaving lesion. Multiple myeloma occurring primarily or initially in the mouth is by far less common than in the jaw bones, these being among the many bones afflicted by the disease in individuals with diagnosed multiple myeloma.
Plasmacytoma is an isolated manifestation of multiple myeloma. Plamacytoma or multiple myeloma is a clonal neoplastic proliferation of plasma cells (myeloma cells) which are terminally differentiated B-lymphocytes. It is most common in individuals 60-75 years of age, occurs more in males, and is rare in persons under 40 years of age. It is twice as common in blacks as it is in whites In the US. It occurs most commonly in bone and in a multicentric manner (multiple locations at the same time), hence the name multiple myeloma. This malignant neoplasm presents more commonly in bone but is also described in soft tissue without bony involvement (extramedullary). About 40-50% of bone-isolated plasmacytomas will progress to multiple myeloma while only 10-12% of soft tissue plasmacytomas will progress to multiple myeloma. Normal plasma cells are immunoglobulin producing cells including IgA, IgD, IgG, IgM, and IgE. Neoplastic plasma cells tend to produce any of these antibodies, but predominantly IgG and IgA. The most common clinical presentation is severe bone pain, especially that of the lumbar spine which is usually aggravated with movement. Bone lesions occur in 70% of patients and usually lead to hypercalcemia, bone fracture and vertebral collapse. Hypercalcemia may lead to soft tissue calcifications. The most common bones affected by multiple myeloma are the vertebrae, skull, mandible, ribs, pelvis, clavicles and scapula. Jaws are affected in about 30% of cases. Extramedullary tissue such as the liver, spleen and lymph nodes can also be affected. Patients with multiple myeloma are susceptible to anemia and therefore often experience fatigue and weakness. They can also develop renal failure due to monoclonal light chain (Bence Jones protein). About 15% of patients develop amyloid deposition in a variety of soft tissues, including the G-I tract and the oral cavity, specifically the tongue. Amyloid in the tongue can present as small yellow nodules or plaques; they can be deep seated within the tongue, causing slurring. They can also occur around the eyes, again as small yellow plaques or nodules. Radiographically, multiple myeloma has a distinct presentation of “punched out” radiolucencies but the radiolucency can also be ill defined. This is particularly true of the skull lesion. The mandible and maxilla can be affected, but the radiographic presentation is not as distinct as in the case of skull lesions. It is important to note that histology and immunohistochemistry alone cannot differentiate between an isolated case of plasmacytoma and the full disease of multiple myeloma. Pathologists usually render the histologic diagnosis of plasmacytoma while oncologists render the clinical diagnosis of multiple myeloma.
Histologically, the biopsy of a patient with isolated plasmacytoma or a patient with the full disease of multiple myeloma demonstrates sheets of monotonous mononuclear cells with plasmacytic differentiation. The atypical plasma cells usually show nuclear and cellular atypia. Mitosis is usually present. The neoplastic cells are monoclonal; this can be supported by an immunohistochemistry stain with kappa or lambda light chains. They are also specific with CD138, a marker for plasmacytoid cell. The final diagnosis of multiple myeloma is determined through a combination of histology, serum and urine protein electrophoresis, blood test for myeloma protein (monoclonal gammopathy), and radiographic changes. Treatment includes chemotherapy, bisphosphonates to control hypercalcemia, bone marrow transplant and radiation therapy. The overall prognosis depends on age; younger patients have a better prognosis than older patients.
References
- Bonet J, Manuel MJ et al. Eosinophilic granuloma of the jaws: a report of three cases. Med. Oral. 2001; 6: 218-224.
- Favara BE, Feller AC, Pauli M et al. Contemporary classification of histiocytic disorders. Med Pediatr Oncol 1997; 29: 157–66.
- Baumgartner I, von Hochstetter A, Baumert B et al. Langerhans cell histiocytosis in adults. Med Pediatr Oncol 1997; 28: 9–14.
- Malpas JS, Norton AJ. Langerhans cell histiocytosis in the adult. Med Ped Oncol 1996; 27: 540–6.
- Akhtar K, Laghari NA, Haq AU, Anees M, Rehman SU, Alam MI. Multiple myeloma in younger age.. J Coll Physicians Surg Pak. 2009 Jan;19(1):62-3.
- Poggio CE. Plasmacytoma of the mandible associated with a dental implant failure: a clinical report. Clin Oral Implants Res. 2007 Aug;18(4):540-3. Epub 2007 Apr 30.
- Canger EM, Celenk P, Alkan A, Günhan O. Mandibular involvement of solitary plasmacytoma: a case report. Med Oral Pathol Oral Cir Bucal. 2007 Jan 1;12(1):E7-9.
- Souza LN, Farias LC, Santos LA, Mesquita RA, Martelli H Jr, De-Paula AM. Asymptomatic expansile lesion of the posterior mandible. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2007 Jan;103(1):4-7. Epub 2006 Oct 16.
- Neville BW. Oral & Maxillofacial pathology. 2nd ed. Philadelphia: W.B. Saunders; pages 604-607, 2009.
- Gardner DG, Heikinheimo K, Shear M, Philipsen HP, Coleman H. Ameloblastomas. In: Barnes L, Eveson JW, Reichart P, Sidransky D, editors. WHO Classification of Tumours: Pathology and Genetics of Head and Neck Tumours. Lyon: IARC Press; 2005.
- Julio César Bisinelli, Sérgio Ioshii, Luciana Borges Retamoso, Simone Tetü Moysés, Samuel Jorge Moysés and Orlando Motohiro Tanaka. Conservative treatment of unicystic ameloblastoma. American Journal of Orthodontics and Dentofacial Orthopedics. Volume 137, Issue 3, March 2010, Pages 396-400.
- Nakamura N, Higuchi Y, Mitsuyasu T, Sandra F, Ohishi M. Comparison of long-term results between different approaches to ameloblastoma. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2002;93:13–20.
- Reichart P.A., Philipsen H.P., Sonner S, Ameloblastoma: biological profile of 3677 cases, Eur J Cancer B Oral Oncol 31B (1995), pp. 86–99.
Sorry! you are incorrect
The expansion, the location and the radiographic findings of the basically unilocular radiolucency may make one think unicystic ameloblastoma. However, the age of the patient is not in support of such a diagnosis. Neither is the sharp resorption of the mesial root of tooth #31 or the small, round radiolucency distal to the larger pathology (below the inferior alveolar canal). The clinical findings of perforated buccal bone and almost missing lingual bone are also not supportive of the behavior of cystic ameloblastoma. In addition, 90% of cystic ameloblastomas occur in association with an impacted tooth resembling a dentigerous cyst. This may also represent a solid type of ameloblastoma, but the lack of clear multilocular radiographic changes makes it unlikely. The histology in this case was not supportive of any type of ameloblastoma.
Ameloblastoma is one of the most common benign neoplasms of odontogenic origin. It accounts for 11% of all odontogenic neoplasms/hamartomas. It is a slow-growing, persistent, and locally aggressive neoplasm of epithelial origin. It affects a wide range of age distribution but is mostly a disease of adults, at an average age of 33, with equal sex distribution. Reports from Africa and India show a male predilection; it also has a predilection for occurrence in black patients. The location and age of this patient can be consistent with an ameloblastoma. The unilocular radiolucency is unusual for the solid type but is consistent with the 10% of the unicystic ameloblastomas that occur in an extra-follicular manner. About 85% of ameloblastomas occur in the posterior mandible; most of these occur in the molar-ramus area, and some occur in the anterior mandible. Three types are described including solid ameloblastoma which is characteristically expansile, radiolucent and multilocular and not consistent with this case. The unicystic type is radiographically unilocular but in 90% of the time is associated with the crown of an impacted tooth. The other 10% are unilocular radiolucency usually associated with teeth such as between teeth. The patients constituting this group are much younger in age and are around 14-20 years of age. The third type occurs on the gingival without bony involvement and is known as peripheral ameloblastoma. Clinically, it resembles a reactive gingival swelling such as pyogenic granuloma or peripheral ossifying fibroma. It is rare and accounts for less than 1% of all ameloblastomas.