April 2010: Large unilocular radiolucency anterior maxilla
Can you make the correct diagnosis?
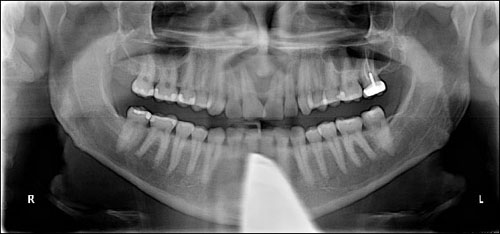
This is a 37-year-old male with a large, asymptomatic, unilocular and well-demarcated radiolucency in the anterior midline maxilla involving the mid-root to apices of teeth #s 7-10 (Figure 1).
Sorry! you are incorrect
Given the radiographic findings of a unilocular and well-defined radiolucency one has to consider a cyst(s) on the differential diagnosis. Being closely associated with the apices of the central and lateral incisors, a radicular cyst would be a reasonable consideration. The associated teeth, however, are vital; this indicates that it is not a periapical cyst. The histology is also not supportive of a periapical cyst.
Apical periodontal cyst, also known by a variety of other names including radicular and periapical cyst, is an inflammatory cyst and is the most common odontogenic cyst. It is the result of pulpitis/pulp necrosis, which mainly caused by a badly decayed tooth but can also be the result of tooth fracture, failed endodontic treatment or an old filling with secondary caries (1-2). It can occur at any age but is more common in adults in their fourth and fifth decade of life. It is usually present at the apex of a tooth but can be apical lateral to a tooth. It is usually asymptomatic and small (around 0.5-1.5 cm) in size but can occasionally reach large sizes. It can be symptomatic, i.e. painful and expansile, if infected. The infected cysts may break through the cortical bone in the form of a fistula, usually buccal or labial in the mandible and buccal or palatal in the maxilla. It is more common in males than females and slightly more common in the maxilla, especially the anterior maxilla (1-2). Radiographically, it presents as well-demarcated or corticated unilocular radiolucency at the apex of a tooth or apical and lateral of a tooth. Occasionally, the radicular cyst can be multilocular. It can also be associated with root resorption but rarely. Histologically, it is made up of a cystic structure lined by epithelium and supported by a connective tissue wall. The latter is usually chronically inflamed and frequently associated with abscess. Treatment ranges from conventional endodontic treatment to apicoectomy to extraction of the tooth with curettage of the cystic structure. It has a good prognosis.
Sorry! you are incorrect
Given the radiographic findings of a unilocular and well-defined radiolucency, a cyst has to be on the differential diagnosis. OKC would be considered, but the location of anterior maxilla is very uncommon for this OKC. The histology in this case is not supportive of OKC.
The odontogenic keratocyst (OKC) is an aggressive odontogenic cyst, known for its rapid growth and its tendency to invade the adjacent tissues, including bone. It has a high recurrence rate and is associated with basal cell nevus syndrome (5-6). It affects patients in the age ranges of 20-29 and 40-59, but cases in patients ranging in age from 5 to 80 years have been reported (5). The distribution between sexes varies from equal distribution to a male-to-female ratio of 1.6:1, except in children. Odontogenic keratocysts may occur in any part of the upper and lower jaw, with the majority (almost 70%) occurring in the mandible. They occur most commonly in the angle of the mandible and ramus (6). Anterior maxilla is a rare location for OKC but has been described (3-4). Radiographically, OKCs present predominantly as unilocular radiolucencies with well-defined or sclerotic borders; they may also present as multilocular radiolucencies, but rarely. OKCs commonly present as a unilocular radiolucency with scalloped borders. Teeth associated with OKC are vital. OKCs grow to sizes larger than any other odontogenic cysts. They usually penetrate the bone rather than expand it and grow in an anterior to posterior direction (5-6). Despite this aggressive growth, they often remain asymptomatic, thus growing to large sizes and hollowing the bone. Treatment of choice is surgery with cauterization, especially with Carnoy’s solution.
Congratulations! You are correct
The nasopalatine duct cyst (NPDC) is a developmental non-odontogenic cyst that only occurs in the anterior maxilla from the embryonic remnants of nasopalatine ducts. It is usually located between teeth #s 8 & 9 but can be as posterior as the mid palate and as anterior as the incisive papilla. It is the most common non-odontogenic oral cyst of the oral cavity (7-8). It occurs at any age, including in fetuses, but is most common in the fourth to sixth decade of life and is more common in males. It is usually asymptomatic and is discovered during routine dental examination. If infected, the patient complains of pain with swelling and even drainage; however, swelling is not common. When present, swelling is often in the incisive papilla area in smaller lesions but can be in the midpalate in larger lesions and may be buccal and midpalatal in very large lesions (7-8). Larger and infected NPDC can perforate bone. Radiographically, it usually presents as a bilateral, well-circumscribed, round, ovoid or heart-shaped radiolucency (7-8). Tooth displacement or diverging of the roots of the central incisors is commonly identified. Histopathologically, it is made up of a cystic cavity lined by either stratified squamous epithelium or pseudostratified ciliated columnar cells, or a combination of the two. The supporting connective tissue contains mucous glands, nerve bundles and blood vessels with smooth muscle lining. Depending on the size and clinical symptoms, treatment ranges from no treatment to surgical curettage if the cyst is infected or interfering with a prosthetic appliance. Recurrence is rare and prognosis is good.
References
- Souza LB, Gordón-Núñez MA, Nonaka CF, Medeiros MC, Torres TF, Emiliano GB. Odontogenic cysts: demographic profile in a Brazilian population over a 38-year period. Med Oral Patol Oral Cir Bucal. 2009 Dec 29.
- Avelar RL, Antunes AA, Carvalho RW, Bezerra PG, Oliveira Neto PJ, Andrade ES. Odontogenic cysts: a clinicopathological study of 507 cases. J Oral Sci. 2009 Dec;51(4):581-6.
- Damm DD, Fantasia JE. Oral diagnosis. Radiolucency of anterior maxilla. Odontogenic keratocyst. Gen Dent. 2005 Jul-Aug;53(4):308, 310.
- Marzella ML, Poon CY, Peck R. Odontogenic keratocyst of the maxilla presenting as periodontal abscess. Singapore Dent J. 2000 Dec;23(1 Suppl):45-8.
- Shear M. Odontogenic keratocysts: natural history and immunohistochemistry. Oral Maxillofacial Surg Clin N Am. 2003; 15: 347-362.
- Oda D, Rivera V et al. Odontogenic keratocyst: the northwestern USA experience. J Contemp Dent Pract. 2000 Feb 15; 1(2): 60-74.
- Jaume Escoda Francolí 1, Nieves Almendros Marqués 2, Leonardo Berini Aytés 3, Cosme Gay Escoda 4 Vasconcelos R, De Aguiar MF, Castro W, De Araújo VC, Mesquita. Nasopalatine duct cyst: Report of 22 cases and review of the literature. Med Oral Patol Oral Cir Bucal. 2008 Jul 1;13(7):E438-43.
- Robertson H, Palacios E. Nasopalatine duct cyst. Ear Nose Throat Dis. 1999 Oct;5(4):325-8.