Generalized Discoloration of the Gingiva and Palate
Can you make the correct diagnosis?
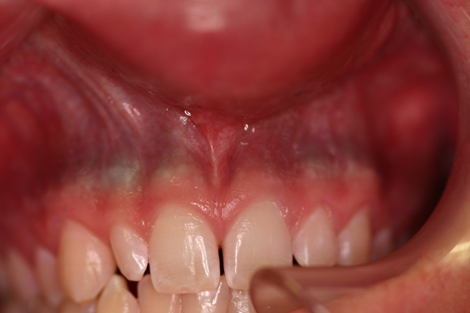
This is an otherwise healthy 17-year-old white male who has had two years of treatment with minocycline for acne. He was referred by his general dentist, Dr. Robert Stockton, for evaluation of discolored oral mucosa, especially in the gingiva and palate.
Diagnostic Information Available
Congratulations. You are Correct!
Discoloration of the oral mucosa after drug use has been described for decades in relationship to a number of drugs and has been attributed to either direct stimulation of the melanocyte activity or to the deposition of pigmented drug metabolites. It can sometimes be the result of combined processes. Several drugs are known to cause mucosal and skin pigmentation including antimalarial agents (particularly chloroquine and hydroxychloroquine), chlorpromazine, birth control pills, AZT, and ketoconazole, a few among many others (1).
Tetracycline, especially its semisynthetic derivative minocycline, has been implicated in oral soft and hard tissue discoloration since 1984. Minocyline is used for the treatment of inflammatory acne and is known for its broad spectrum activity against aerobic and anaerobic gram-negative and gram-positive organisms. Oral mucosal and hard tissue pigmentation is described in up to 4% of long-term users (over eight months), especially at doses of 100 or more milligrams per day (2-4). The bone pigmentation ranges from grey-green to grey-blue and is caused by accumulation of quinone from the degradation of the aromatic ring of the drug. Similar color is deposited along the apical roots. The mucosal discoloration is most commonly found in band-like blue-black discoloration along the attached gingiva (Figs 1 & 2) and the alveolar mucosa. It is also described in the central part of the hard palate. The mucosal discoloration is only a reflection of the discolored bone and roots and is not a true soft tissue discoloration; however, soft tissue discoloration is described on the tongue and skin (2-4). The latter is more common in scar areas, especially acne scar areas, and is bluish-grey in color. Teeth can be discolored, but rarely. If affected, the affected teeth are usually permanent and are along the middle and incisal thirds. Unlike tetracycline, minocycline is a weak chelator and does not bind to calcium very well; in addition, the teeth do not fluoresce when exposed to ultraviolet light. The discoloration may or may not subside upon discontinuation of the drug since it is deposited on the bone and teeth. If it subsides, it usually takes several months to years.
To be complete, it must be mentioned that multiple macular or diffuse pigmentation of the gingiva or oral mucosa carries a long list of differential diagnoses that goes beyond drug use and includes racial pigmentation, multiple melanotic macules, smoker’s melanosis, Peutz-Jeghers syndrome, Addison’s disease, heavy metal poisoning, postinflammatory hyperpigmentation, and melasma among many others.

Figure 1. This clinical photograph represents the band-like grayish blue pigmentation of the maxillary anterior gingiva.
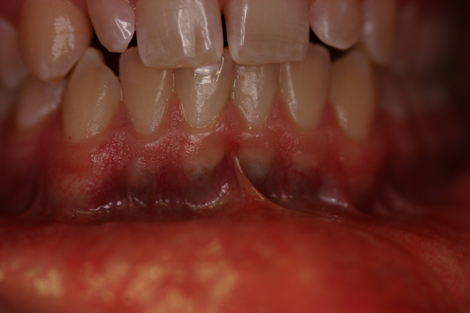
Figure 2. This clinical photograph represents the band-like grayish blue pigmentation of the mandibular anterior gingiva.
Treatment
The patient was advised to stop minocycline treatment. He was advised to switch to another acne medication such as Accutane® if such treatment was still necessary. He was placed on vitamin C for its antioxidant properties. The patient will be kept under periodic observation.
References
- Cicek Y, Ertas U. The normal and pathological pigmentation of oral mucous membrane: a review. J Contemp Dent Pract. 2003; 4: 76-86
- Treister NS, Magalnick D, et al. Oral mucosal pigmentation secondary to minocycline therapy: report of two cases and a review of the literature. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2004 Jun;97(6):718-25
- LaPorta VN, Nikitakis NG, Sindler AJ et al. Minocycline-associated intra-oral soft-tissue pigmentation: clinicopathologic correlations and review. J Clin Periodontol. 2005; 32:119-122.
- Herbers AH, Gerlag PG Bluish-grey pigmentation of fingernails, gingiva, teeth and peri-oral region. Minocycline. Neth J Med. 2004 Feb;62(2):58, 65
- Sarswathi TR, Kumar SN et al. Oral melanin pigmentation in smoked and smokeless tobacco users in India. Indian J Dent Res. 2003; 14: 101-106.
- Gavren BA, Lumerman H et al. Multiple pigmented lesions of the lower lip. J Oral Maxillofac Surg. 2002 Apr;60(4):438-45
- Gorlin RJ, Cohen Jr. et al. Syndromes of the head and neck, 3rd edition. Oxford: Oxford University Press, 1990. p. 399-402.
- Braithwaite, SS, Clasen, RA et al. Silent corticotroph adenoma: case report and literature review. Endocr Pract. 1997; 3: 297-301.
- Erickson QL, Faleski EJ et al. Addison’s disease: the potentially life-threatening tan. Cutis. 2000 Jul; 66(1):72-74.
Sorry, this is not the correct diagnosis.
In the United States alone, there are over 65 million tobacco users; 56 million smoke cigarettes, and 12 million use smokeless tobacco. There are also 40 million former tobacco users. Heavy cigarette, cigar and pipe smokers stimulate the melanocytes to actively produce melanin in the area where most smoke comes in contact with the mucosa. This is believed to be a protective effect against certain tobacco elements; for example, melanin is known to bind to chemicals such as nicotine. This phenomenon is also true of the melanin production when exposed to the sun; it also is a protective process against ultraviolet light and its oxidative effect on the skin cells. Smoking-related melanin production produces flat light brown pigment, usually diffuse, and present on the facial anterior gingival (1, 5). It is more commonly present on the mandible than the maxilla in heavy cigarette smokers (5), the commissure and buccal mucosa of heavy pipe smokers, and the hard palate in reverse smokers. The histology of the brown pigment is due to excessive melanin production. In this case, the patient has no history of tobacco use.
Sorry, this is not the correct diagnosis.
This is an inherited, autosomal dominant condition with 35% mutation. It is also known as Hereditary Intestinal Polyposis Syndrome (7). The polyps have a 10% tendency for malignant transformation. The dentist has an advantage for diagnosing this disease due to the characteristic presentation of multiple peri-oral flat and small brown spots (6-7). They are less than 5mm in size and can affect the anterior tongue, lips, around the eyes, nose, hands and feet. The brown spots represent excessive production of melanin. The histology of the polyps depends on whether or not they are benign or malignant. There is no need to treat the pigmented spots, but the patient should be referred to a gastroenterologist for evaluation of the intestinal polyps. The clinical history and presentation of this case is not supportive of Peutz-Jegher’s Syndrome.
Sorry, this is not the correct diagnosis.
Addison’s disease is an endocrine disorder affecting all ages and both sexes equally. It is characterized by muscle weakness, fatigability, nausea, vomiting, anorexia, weight loss, hypotension, and sometimes salt-craving (8-9). It can also present with skin and mucosal darkening, referred to as “bronzing,” which may affect the mouth at an early stage of the disease in the form of multiple flat and pigmented lesions (8-9). Addison’s disease occurs as a result of low cortisol and sometimes low aldosterone, both of which are produced by the adrenal glands. The symptoms occur gradually; it takes 90% loss of the functioning cells in the adrenal cortex in order for the disease to occur (8-9). Two types are described: primary and secondary. The primary type consists of direct loss of adrenal function while the secondary type is due to the pituitary gland dysfunction leading to decreased production of ACTH hormone. The main etiology of the primary Addison’s is autoimmune destruction of adrenal cells; other factors have been proposed such as infection, tumor metastasis, and hemorrhage. Cortisol is essential in balancing a number of systems in the body including the cardiovascular system, the immune system, metabolic activity and several other vital activities that maintain a health and function. Aldosterone helps control water and salt balance as well as blood pressure. Cortisol is released in response to the pituitary producing ACTH. Therefore, low cortisol production by the adrenal gland in primary Addison’s disease translates in high serum levels of ACTH, which can prove to be a good test for determining a diagnosis of Addison’s disease. Additionally, high ACTH is associated with stimulating the melanocyte stimulating hormone (MSH), which leads to excessive production of melanin, bronzing of the skin (both sun and non-sun exposed), pigmentation of the oral mucosa, pigmentation of scars, skin folds and skin in pressure areas. In the secondary type, the ACTH level is low because of a disease that this preventing the pituitary to release the hormone that inhibits the adrenal gland from producing cortisol. The clinical symptoms related to low cortisol production are similar in both types. Dentists may be the first to discover Addison’s if patients complain of multiple brown pigments in the mouth occurring recently in the absence of history such as smoking and drug ingestion such as birth control pills (1, 6). The best test for Addison’s is the plasma ACTH level, which is high in the primary type and low in the secondary type. Once the diagnosis is established, steroid supplements are the treatment of choice for the primary type. The clinical presentation of this case is not supportive of Addison’s disease.