Severe localized periodontitis; right posterior mandible
Can you make the correct diagnosis?
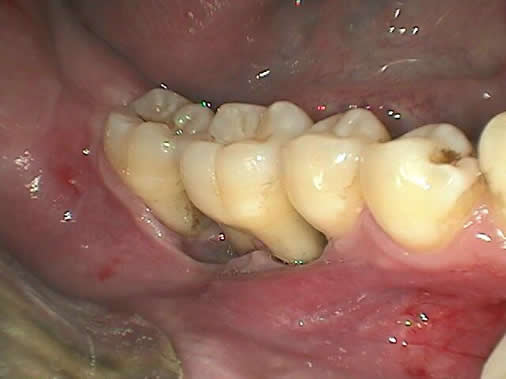
Figure 1 Photograph taken at first clinical presentation. Note the severe periodontitis with gingival recession involving teeth #s 29-31
This is a 27-year-old white male who presented with less than a year history of a lesion in the posterior mandible with symptoms of pain, gingival swelling, and ulceration around teeth #s 29-31.
Congratulations! You are correct
Langerhans cells are dendritic cells of bone-marrow origin. The disease Langerhans’ cell histiocytosis is generally a disease of children rarely affecting adults. The old name for this condition is histiocytosis X classified into eosinophilic granuloma (monostotic and polyostotic, Hand-Schuller-Christian and Letterer-Siwe disease. The first two types (EG and HSC) are less aggressive and are chronic in clinical behavior while the last (LS) is more aggressive and acute in behavior. The currently used classification breaks patients into unifocal, multifocal/unisystem and multifocal/multisystem. This classification also divides patients into low and high risk categories. Low-risk patients would include the unifocal and multifocal/unisystem and the high-risk would include multifocal/multisystem patients. If the disease affects one organ be it in one site or multiple sites of one organ (i.e. bone, lymph nodes, skin or pituitary gland), it is considered to be low-risk type. If the disease involves multiple organs such as the lungs, liver, spleen and bone marrow (multifocal and multisystem), it is considered to be high-risk type.
Langerhans cells are CD1a positive and for that reason, immunohistochemistry staining is very helpful. They are also S-100 and CD45 positive. Langerhans cells can also be comfortably identified by the H & E stain.
The lytic lesion in the posterior mandible (if taken alone) would be considered as unifocal/unisystem LCH with excellent prognosis. However, this patient has multiple small lesions in other bone (still considered unisystem but multifocal). He also has potential lesion in his pituitary gland given his past history of diabetes insipidus and “pituitary swelling”. This clinical presentation is still considered low-risk type. LCH usually presents with pain and swelling but can also be asymptomatic. The bony lesions are usually aggressively lytic especially those of the mandible. As mentioned above, this disease rarely occurs in adults and that more than 50% of the cases affect children under 10 years of age, with male predilection.
Adult LCH most commonly affects the bones especially the jaws and skull bones in general. LCH of the jaw bone usually presents as either localized severe periodontitis (as is the case in this patient) or generalized severe periodontitis. It can also affect the skin, lymph nodes, pituitary (not common) and lungs (not common). Radiographically, the bony lesions are sharply radiolucent and the jaw lesions give the impression of teeth “floating” in space due to the significant bone destruction.
Treatment includes curettage especially of the jaw lesions. Chemotherapy and low-level radiotherapy have also been effective. The unifocal disease has an overall 95% survival rate, the two organ involvement has a 75% overall survival rate and the more organs are involved, the less favorable the prognosis.
References
- Bonet J, Manuel MJ et al. Eosinophilic granuloma of the jaws: a report of three cases. Med. Oral. 2001; 6: 218-224
- Favara BE, Feller AC, Pauli M et al. Contemporary classification of histiocytic disorders. Med Pediatr Oncol 1997; 29: 157–66.
- Baumgartner I, von Hochstetter A, Baumert B et al. Langerhans cell histiocytosis in adults. Med Pediatr Oncol 1997; 28: 9–14.
- Malpas JS, Norton AJ. Langerhans cell histiocytosis in the adult. Med Ped Oncol 1996; 27: 540–6.
- Sasaki, T., D. R. Moles, et al. (2005). “Clinico-pathological features of squamous cell carcinoma of the oral cavity in patients <40 years of age.” J Oral Pathol Med 34(3): 129-33.
- Sarkaria JN, Harari PM. Oral tongue cancer in young adults less than 40 years of age: rationale for aggressive therapy. Head Neck 1994; 16: 107 11.
- Llewellyn CD, Johnson NW, Warnakulasuriya KA. Risk factors for squamous cell carcinoma of the oral cavity in young people a comprehensive literature review. Oral Oncol 2001; 37: 401 18.
- Cakmak SS, Soker M et al. Non-African Burkitt’s lymphoma manifesting at the jaw and as a right orbital mass in a child. J Pediatr Ophthalmol Strabismus. 2003; 40: 306-308.
- Chetty R, Hlatswayo N, et al. Plasmablastic lymphoma in HIV+ patients: an expanding spectrum. Histopathology. 2003 Jun; 42(6): 605-9.
- Carbone A. Emerging pathways in the development of AIDS-related lymphomas. Lancet Oncol. 2003 Jan; 4(1): 22-9.
- Oda, D., Persson, R., Sabbath, D., Haigh, W.G., Penn, I., and Aziz, S. Oral presentation of post-transplantation lymphoproliferative disorder: an unusual manifestation. Transplantation. 61:435-440, 1996.
- Penn I, First MR. Development and incidence of cancer following cyclosporine therapy. Transplant Proc 1986; 18 (suppl 1): 210.
- Penn I, Hammond W, Brettschneider L, Starzl TE. Malignant lymphomas in transplantation patients. Transplant Proc 1969; 1: 106.
Sorry! you are incorrect
Oral SCC of the gingiva is not common especially in young patients and especially in patients with no risk factors (no history of smoking). The histology is not supportive of gingival SCC.
Oral SCC affects males over the age of 40 years, with an observed male to female ratio of 2:1 generally and 1.4:1 in the United States. The most common sites of occurrence are the tongue, the ventral and lateral surfaces, the floor of mouth, the soft palate area followed by gingiva in about 12% of the cases. Of the 12%, half of the gingival SCCs resorb the underlying bone.
The incidence of oral squamous cell carcinoma in patients under the age of 40 constitutes 0.4-8.3% of all oral SCC cases and is on the increase. It is generally believed that oral SCC in young patients has a more aggressive behavior and therefore worse prognosis than that in the older population. However, there are reports that claim that oral SCC in young patients has a better prognosis. Tobacco use, both in cigarette and smokeless forms, is widely known to be strongly associated with oral SCC of the older population; it is a factor in up to 90% of cases. Some studies report that smoking is not a significant risk factor in the younger population with oral SCC. However, Llewellyn et al demonstrated that smoking before age 16 and excessive drinking are significant risk factors in the oral SCC in young population. Other proposed risk factors include human papilloma virus, especially type 16 to be more prevalent in the tonsillar and laryngeal carcinomas and other parts of the oral cavity. Determination of the prognosis of oral SCC in both age groups is based on the clinical stage and histologic classification.
Sorry! you are incorrect
Given the clinical and radiographic changes, this presentation would be supportive of severe localized periodontitis. However, the age, the lack of family history of juvenile periodontitis and the lack of risk factors such as smoking are not supportive of the diagnosis of severe chronic periodontitis. The histology is not supportive of this diagnosis.
Periodontitis is characterized by inflammation of the gingiva, destruction of the periodontal ligament and bone loss. It is more common in older patients, smoker and/or drinker with poor oral hygiene. It can also be associated with systemic diseases such as uncontrolled diabetes mellitus, AIDS, leukemis, and neutropenia.
Sorry! you are incorrect
The age of the patient, the aggressive bony destruction and the localized nature of this case would be clinically supportive of a non-Hodgkin’s type lymphoma (NHL), be it Burkitt’s or any other type of B-Cell lymphoma. The histology is not supportive of this condition.
Malignant lymphoma is a family of diseases, most of B and T-lymphocyte origin. In the USA, about 85% of the NHL cases are of B-lymphocyte origin and about 20-40% occur outside the lymph nodes as the primary lesion. In the oral cavity, NHL may affect the soft tissue such as the palate or the bone. It may be isolated to the mouth or be part of a systemic disease. Clinically, they may appear as slowly enlarging soft and bluish lesion on the soft palate or destructive, ulcerating lesion in the jaw or soft tissue. Lymphomas of the mouth can present as a non-healing ulcer, rapidly growing and ulcerating nodule or a very destructive bony lesion. NHL is primarily a disease of older males, but certain types such as lymphoblastic and Burkitt’s lymphomas occur in children. About 40,000 cases are reported annually in the U.S.A. with a 50% death rate. NHL has gone through an evolution of classifications. The latest divides lymphomas into: Low grade up to 40%, intermediate up to 60% and high grade around 5%. The etiology ranges from unknown to viral i.e. Burkitt’s and plasmablastic lymphoma in association with Epstein Barr Virus (EBV). Other etiologies include chemicals, immunosuppression, autoimmune diseases. The latter would include patients with Sjogren’s syndrome being at forty fold increase in susceptibility to developing lymphoma than the general population. The risk for lymphoma increases in immunosuppressed patients such as AIDS and organ transplant patients. EBV virus seems to play a major role in lymphomas of AIDS and organ transplant (immune suppressed patients). Treatment includes chemotherapy and/or radiation.