Maxillary gingival and palatal swellings
Can you make the correct diagnosis?
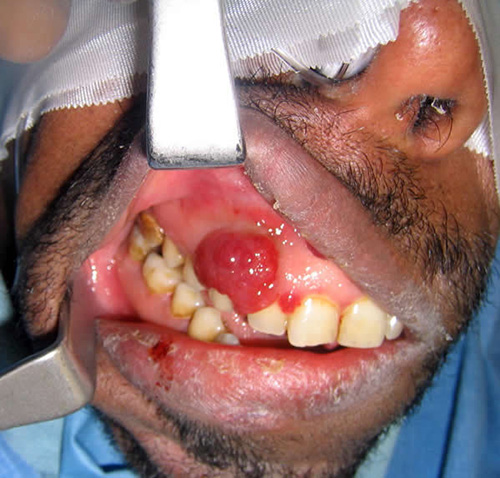
This is a 44-year-old African-American male who first presented to his physician for a skin problem and scaling of the scalp. The skin problem was diagnosed as psoriasiform dermatitis and was treated with desonide 0.05% ointment twice a day. For the scalp scaling, he was using ketoconazole 2% and selenium sulfide shampoos on a regular basis.
Sorry! you are incorrect
Pyogenic granuloma constitutes 85% of all reactive gingival swellings, representing a profuse mass of vascular granulation tissue (1). It can be induced by local irritants such as excessive plaque, sharp fillings and dental calculus; it sometimes forms in an extraction socket in response to an irritant left in the socket. It can occur anywhere in the oral cavity and skin, especially the tongue, lips, fingers and nail beds (1). In the mouth, it occurs most commonly in the gingiva, especially the maxillary buccal and interproximal gingiva (1-2). Occasionally, it may surround the tooth. It is usually highly vascular, fast-growing, exophytic, lobular, sessile, and ulcerated or covered by psuedomembrane. The color changes from red to pink when it starts to heal. It occurs at any age and sex with a slight predilection for young females; it affects 1% of pregnant females. Pyogenic granuloma is usually painless except during eating, when bleeding and pain is described (1). Histologically, it presents as a mass of loose and vascular granulation tissue, usually with ulcerated or eroded surface epithelium and many inflammatory cells. A range of treatment modalities are available, including excision with removal of the local irritant, laser surgery, or intralesional injection with absolute alcohol, steroids or botulinum toxin (2-3). Scaling and polishing prior to surgical removal helps shrink the lesion. The prognosis is good, although recurrence is possible, especially during pregnancy. Multiple pyogenic granulomas have been described, but rare. The histology was not supportive of pyogenic granuloma.
Congratulations! You are correct
Kaposi’s sarcoma (KS), malignant lymphoma and cervical cancer are three AIDS-defining malignant neoplasms. KS is the most common, affecting 50% of AIDS patients and accounting for approximately 90% of all cancers in this group (8). However, it must be mentioned that since the introduction of HAART antiviral treatment of AIDS patients, the incidence of KS has gone down (11).
About 71% of AIDS-related KS cases affect the oral cavity combined with skin and visceral lesions (8). In about 22% of these patients the oral cavity is the primary site for KS and, at times, it is the only affected site (8). It is a malignant neoplasm of vascular origin believed to be of endothelial origin, mainly lymphatic endothelium. It usually presents in multiple areas all at the same time. Recently, a report concluded that it can be induced by human herpes virus 8 (HHV8) (7-10); in this case, it is obviously oncogenic rather than infectious and reactive in nature. HHV8 has been described in other malignant neoplasms such as AIDS-related body cavity lymphoma (9).
Four types of KS are described (7, 9): classic, AIDS-related, immuno-suppression-associated and the African type. The classic type of KS is a rare and non-aggressive disease and is especially rare in the oral cavity (7, 9). It is usually slow-growing, predominantly affecting older males of Mediterranean origin including Italians, Greeks and Ashkenazi Jews (7, 9), and occurs as multiple reddish-purple lesions on the lower extremities. AIDS-related KS is aggressive in clinical behavior (7, 9) and affects mostly young homosexual and bisexual males in the US and heterosexual males in African countries; it occurs in the oral cavity and on the skin of the head and neck, trunk, etc. The mouth, especially the palate, is a frequent site of occurrence as described above (accounting for 71% of cases). It may present as flat to nodular purplish-red lesion(s). It is usually asymptomatic, but may be painful. The immuno-suppression type is associated with organ transplant patients, especially kidney transplant patients (7, 9, 12). It is described in other patients, especially those on low-dose prednisone. It has also been described in cancer patients who are on long-term chemotherapy. This type also affects patients of Mediterranean origin. The African type is endemic in some parts of Africa (8, 9), and is further classified into two types: an aggressive and fatal type that occurs in children and a less aggressive form that occurs in adults. The latter is more common on the extremities, while the former is associated with lymphadenopathy and is more generalized. The aggressive form may also be associated with AIDS (9).
KS is made up of irregular vascular spaces that fail to complete. Several types are described including patch, plaque and nodular (9). The latter is much easier to diagnose than the former two; in particular, cases at the patch stage of the disease can be misinterpreted as reactive in nature (9). Our case was not difficult to diagnose since it was the nodular type. The Immunohistochemistry stain for HHV 8 was strongly positive (Fig 6) as was the CD31 (blood vessels) stain (Fig 5). Histologically, it is very difficult to differentiate KS from bacillary angiomatosis, a vascular lesion associated with cat-scratch bacillus. The latter is usually excluded via special stains for the micro-organism.
Treatment of KS depends on the clinical subtype and stage, the extent of the disease, whether it presents in singles or multiples, and whether it involves the skin/mucosa or the visceral organs. Many factors are involved in deciding on a specific mode of treatment. Single skin lesions of the classic type respond well to electron beam radiation therapy. Radiation of single oral lesions is not as successful given the oral complications from radiation treatment, including mucositis, xerostomia and osteoradionecrosis. Local intralesional injections have also been described to be useful in some single lesions including those of the oral cavity. Systemic chemotherapy is used for more advanced and disseminated types of the disease. The prognosis varies and depends on the subtype; clearly, classic KS has a much better prognosis than AIDS-related KS or the African type affecting children.
Treatment
The surgery was performed under general anesthesia. Intravenous medications were placed. The patient was intubated without complications using nasal endotracheal intubation. The lesion at the junction of the hard and soft palate was removed first using electrocautery and coag to help obtain hemostasis. Pressure was also placed using sponge packs. The bleeding was primarily venous. Attention was then directed to the anterior hard palate and anterior maxilla. Hemostasis was obtained using electrocautery on the coag setting, along with Gelfoam impregnated with thrombin overlaid over the surgical areas.
The excisional biopsy of the three lesions included the lesion at the junction of hard and soft palate, the palatal aspect of anterior maxilla behind teeth numbers 6, 7, 8, 9, 10, and 11 and the labial aspect of the anterior maxilla. The patient reported an uneventful postoperative course. He did not complain of any pain or discomfort. He was placed on Peridex oral rinse and oxycodone for pain.
References
- Fantasia JE, Damm DD. Red nodular lesion of tongue. Pyogenic granuloma. Gen Dent. 2003 Mar-Apr;51(2):190, 194.
- Ichimiya M, Yoshikawa Y, Hamamoto Y, Muto M. Successful treatment of pyogenic granuloma with injection of absolute ethanol. J Dermatol. 2004 Apr;31(4):342-4.
- Pham J, Yin S, Morgan M, Stucker F, Nathan CA. Botulinum toxin: helpful adjunct to early resolution of laryngeal granulomas. J Laryngol Otol. 2004 Oct;118(10):781-5.
- Flaitz CM, Peripheral giant cell granuloma: a potentially aggressive lesion in children.
Pediatr Dent. 2000 May-Jun;22(3):232-3. - Chaparro-Avendano AV, Berini-Aytes L, Gay-Escoda C. Peripheral giant cell granuloma. A report of five cases and review of the literature. Med Oral Patol Oral Cir Bucal. 2005 Jan-Feb;10(1):53-7; 48-52.
- Neville BW, Damm DD, Allen CM, Bouquot JE. Peripheral giant cell granuloma. In: Oral and Maxillofacial Pathology, 2nd edition. Philadelphia: W.B. Saunders, 2002. p. 449-451.
- Brown EE, Fallin D, Ruczinski I, Hutchinson A et al. Associations of classic Kaposi sarcoma with common variants in genes that modulate host immunity. Cancer Epidemiol Biomarkers Prev. 2006 May;15(5):926-34.
- Lager I, Altini M, Coleman H, Ali H. Oral Kaposi’s sarcoma: a clinicopathologic study from South Africa. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2003 Dec;96(6):701-10.
- Fletcher CDM. Diagnostic histopathology of tumors. Second Edition. Churchill-Livingston, 2000. Pages 61-66.
- Kalpidis CD, Lysitsa SN, Lombardi T, Kolokotronis AE et al. Gingival involvement in a case series of patients with acquired immunodeficiency syndrome-related Kaposi sarcoma. J Periodontol. 2006 Mar;77(3):523-33.
- Martinez V, Caumes E, Gambotti L, Ittah H. Remission from Kaposi’s sarcoma on HAART is associated with suppression of HIV replication and is independent of protease inhibitor therapy. Br J Cancer. 2006 Apr 10;94(7):1000-6.
- Tan HH, Goh CL. Viral infections affecting the skin in organ transplant recipients: epidemiology and current management strategies. Am J Clin Dermatol. 2006;7(1):13-29.
- Chan YC, Giam YC. Guidelines of care for cutaneous haemangiomas. Ann Acad Med Singapore. 2005 Jan;34(1):117-23.
- Whang KK, Cho S, Seo SL. Excision of hemangioma and sculpting of the lip using carbon dioxide laser. Dermatol Surg. 2004 Dec;30(12 Pt 2):1601-2; author reply 1602.
- Benedetto AV. News in treatment of angiomas. J Eur Acad Dermatol Venereol. 2004 Mar;18(2):122-3
- Lambrecht JT, Stubinger S, Hodel Y. Treatment of intraoral hemangiomas with the CO2 laser. Schweiz Monatsschr Zahnmed. 2004;114(4):348-59.
Sorry! you are incorrect
Hemangioma is a family of benign developmental vascular anomalies occurring at infancy. They progress through two stages of growth: a rapid growth phase followed by an involution phase (13-14). Vascular lesions are most common in infants. Lymphangiomas occur at birth and progress with age, while hemangiomas typically occur a few weeks after birth and continue to grow rapidly for the first year; they stop growing and begin to involute within the subsequent few years. Hemangiomas are benign proliferations of blood vessels with many classifications; capillary and cavernous hemangiomas are the most common types. Capillary hemangiomas affect 1% of all newborns in the United States (15-16). Half of all hemangiomas occur in the head and neck area, especially the tongue. They are the most common cause of macroglossia (13-16). They can also occur on the buccal mucosa and lips. In addition, hemangioma has a slight predilection for occurrence in females. The lesion can present as flat or exophytic, smooth-surfaced or lobular, and localized or diffuse; though usually single and localized, it can also present in multiples. Superficial hemangiomas are bright red, while the deep lesions are purplish-red in color; they blanch on pressure unless thrombosed. The vast majority will regress and resolve within the first ten years of age (13). Treatment of hemangioma depends on its size, its relationship to other anatomical structures and the rate of blood flow. Observation is important since many spontaneously involute, especially capillary hemangiomas. If a hemangioma persists, local topical application of injections with corticosteroids has a 75% success rate of involution within two weeks to two months post-injection (15). Several complications are described with local and systemic use of steroids; interferon alfa-2a has also been successfully used (15). Surgical procedures include excisional scalpel surgery for smaller lesions and laser removal for larger lesions. Laser use includes CO2; argon and other types of laser have also been used with variable rate of success (14-16). Prognosis depends on the size and whether it is a soft tissue or bony lesion: it can range from good to extremely poor with gross facial deformity and compromised function. Multiple and large and diffuse hemangiomas are described, but not commonly. The histology is not supportive of a hemangioma.
Sorry! you are incorrect
Peripheral giant cell granuloma constitutes less than 5% of all reactive gingival swellings, and consists of a hyperplastic mass of vascular granulation tissue with many osteoclast-like multinucleated giant cells. It presents as a lobular, purplish-blue exophytic nodule exclusively on the gingiva, both edentulous and dentate, and usually anterior to the molars (4-5). It originates from either the periodontal ligament or the periosteum. It occurs across a wide age range, especially in children, young adults, and females (2:1 female to male ratio) (4-6). It presents as either sessile or pedunculated and smooth surfaced or lobular; though usually painless, it can occasionally be ulcerated, painful and accompanied by bleeding (4-6). Like pyogenic granuloma, it is usually present either on the buccal or lingual gingiva or between teeth, but it can occasionally surround the teeth (4-6) and act aggressively by displacing teeth much like a sarcoma (4). It can also resorb the underlying bone in a smooth and concave “saucer-like” manner. Complete excision including curettage of underlying bone is the preferred treatment. It has a good prognosis with recurrence rate of approximately 10-20% (6). Peripheral ossifying fibroma occurs as a single lesion and in association with teeth and rarely on an edentulous alveolar ridge. Neither the clinical presentation or the histology are supportive of this diagnosis.